Chapter 14:
Afghanistan and Pakistan
INTRODUCTION
In 1967, endemic smallpox in continental southern Asia extended over a contiguous block of countries from Afghanistan through West Pakistan, India, Nepal, Bhutan, and East Pakistan. Epidemiologically, this area could be subdivided into two parts: a western part consisting of Afghanistan and West Pakistan and an eastern part that included India, Bhutan, Nepal and East Pakistan. Separating these two parts was the heavily guarded border between India and West Pakistan. Few persons travelled across this border and, so far as is known, no cases of smallpox were imported across it after 1966. The health programme of West Pakistan functioned quite independently of that of East Pakistan, and in December 1971, when the latter province became the independent state of Bangladesh the two programmes were, of course, entirely separate. The programme in East Pakistan /Bangladesh is described in Chapter 16 and the programmes in India, Bhutan and Nepal in Chapter 15.
West Pakistan and Afghanistan were epidemiologically closely linked because numerous travellers moved freely across their long common border (Fig.14.1), including several hundred thousand nomads who lived in Pakistan in the winter and in Afghanistan in the summer. Smallpox spread easily across this border.
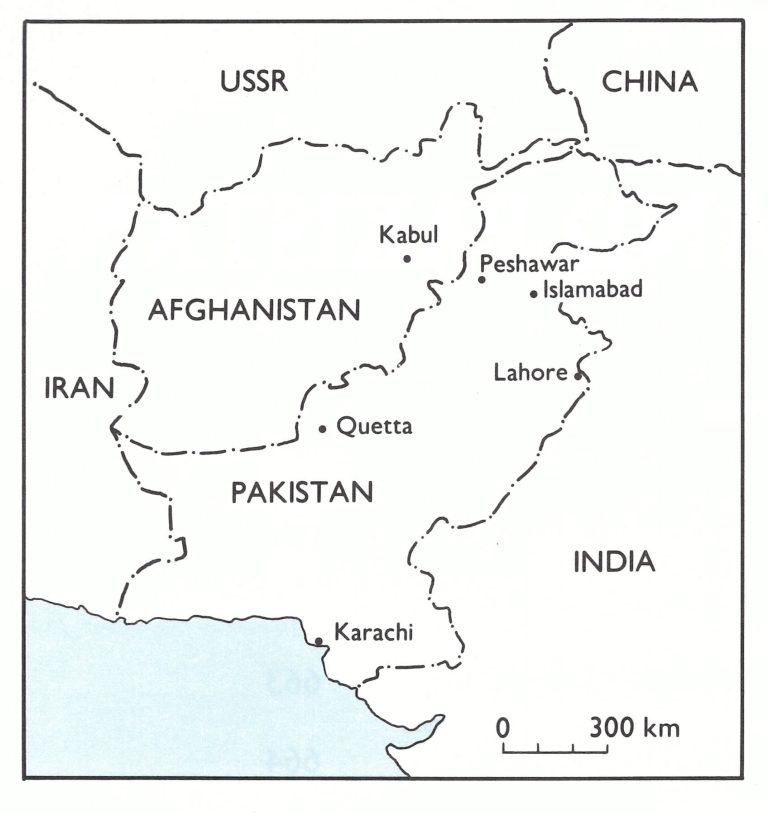
Fig 14.1 Afghanistan and Pakistan and adjacent countries.
Pakistan and Afghanistan are both Muslim countries but differ greatly in most other respects—politically and geographically, in historical and socio-economic development and in the manner in which their smallpox eradication programmes evolved. A WHOassisted vaccination campaign had begun in 1963 in Afghanistan. By 1967, encouraging reports from programme staff made it seem reasonable to expect that systematic vaccination in the towns and cities and a national outbreak-containment programme would rapidly interrupt transmission. This optimistic view faded a year later, when it was discovered that itinerant hereditary variolators were active throughout much of the country, particularly in the extensive remote mountainous areas, spreading smallpox as they travelled. Because Afghanistan was a country with few roads, a primitive health infrastructure and orthodox religious practices which impeded vaccination, it was feared that transmission might be sustained in isolated, virtually inaccessible areas despite the best efforts at control. As late as 1971, WHO senior staff believed that Afghanistan might be the endemic country most likely to thwart the ultimate goal of global eradication. An extraordinary programme and a heroic effort by Afghan and WHO staff were to produce yet another surprise when, in September 1972, Afghanistan succeeded in interrupting smallpox transmission.
Pakistan, in contrast to Afghanistan, had a comparatively well developed health infrastructure, extending throughout most of the country, and a population which generally could be easily reached by the relatively extensive network of roads. A programme of routine smallpox vaccination had been established since the late 19th century; variolation was rarely practiced. The epidemiological behaviour of smallpox in Pakistan had been characterized during 1966-1967 in a unique series of studies whose findings were to prove significant in shaping the strategy of eradication programmes in other countries. An important observation was that urban centres played a crucial role in sustaining smallpox transmission, especially during the summer and autumn, when the incidence was low. The investigators discovered, however, that even during the months of highest incidence and in what was considered to be a heavily infected district, the number of outbreaks was sufficiently small to require only a few teams to detect and contain them. Because they found the levels of vaccinial immunity to be already high in Pakistan, the investigators recommended that priority should be given to detecting and containing outbreaks, especially in urban areas and during the season of lowest incidence. Paradoxically, however, Pakistan was among the last countries to adopt a strategy based on these recommendations. Until 1973, national and WHO programme staff persisted in executing a mass vaccination campaign which was indifferently supported and not satisfactorily conducted. Despite the many factors favouring smallpox eradication, transmission was not interrupted in Pakistan until October 1974.
Meanwhile, there was little communication and virtually no coordination of activities between the programmes in the two countries. Numerous cases of smallpox were imported into Afghanistan from Pakistan and special surveillance programmes had to be developed to combat the threat they represented, which became all the more serious when Afghanistan succeeded in interrupting transmission more than 2 years earlier than Pakistan. The two programmes differed greatly and are discussed separately in this chapter.
AFGHANISTAN
Few of the endemic countries posed as many difficult and unusual challenges as did Afghanistan. In 1967, this isolated, landlocked country was in an early stage of economic and institutional development. The government structure was rudimentary, and in some remote areas the central authority was not recognized. The population—90% of which was illiterate—is estimated to have been 11.9 million in 1968 (United Nations, 1985), although no census had ever been taken.
The Hindu Kush mountain range, with peaks as high as 7500 metres, extends from the extreme north-east border with China towards the south-west, much of central Afghanistan having an altitude of more than 2000 meters (Fig. 14.2). Because of snow, this area was largely inaccessible for almost half the year. The southwestern part of the country is mainly desert, where the extreme heat precluded most programme activities during summer. Except for a single paved allweather road that circled the country, with occasional branches to provincial capitals, the roads were extremely poor, challenging even heavy-duty vehicles. There were no navigable rivers, no railway, and only limited air connections. Programme operations and efforts to communicate with the population were hampered by illiteracy and by the use of 3 different major languages— Dari, Pushtu and Uzbeki.
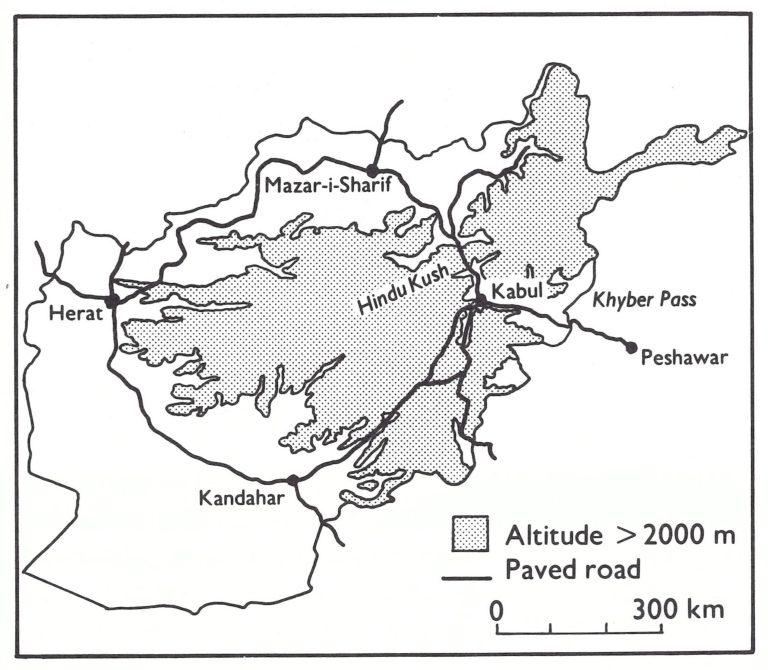
Fig 14.1 Afghanistan : topography and principal roads.
Most of the population lived in the 20 000 villages in rural areas and less than 15 % in the main cities of Kabul, Kandahar, Herat and Mazar-i-Sharif. Religious practices were strict among the predominantly orthodox Sunni Muslim rural dwellers, and religious leaders were highly influential. Of importance to smallpox eradication was the observance of purdah, whereby women were secluded within their homes and the male heads of house hold refused to permit them to leave the house for vaccination or to be vaccinated by male vaccinators.
The health structure was rudimentary. In 1965, there were reported to be 19 primary health centres and 60 hospital-clinics staffed by physicians who were responsible for both curative and preventive services, although few offered even the most elementary preventive measures (World Health Organization, 1965b).
Smallpox Control before 1963
For centuries, variolation had been practised throughout Afghanistan by traditional variolators, the technique usually being communicated from father to son. Many variolators travelled considerable distances in the course of their work. A fee of 10-15 afghanis (US$0.15-0.20) was the usual charge. Scabs (rarely pustular material) from a patient were collected and ground with a mortar and pestle, and the powder suspended in a liquid. The suspension was inoculated by scratch or by pinprick on the forearm or near the wrist. Variolators usually obtained fresh material each year, and therefore variolation tended to be performed during the autumn and winter months, after the number of cases had begun to increase.
Vaccination was all but unknown in Afghanistan until 1936, when a campaign was organized that succeeded in vaccinating 3 million persons over a 3-year period; liquid vaccine produced at a laboratory in Kabul was used (Berke, 1956). This laboratory continued to produce small amounts of vaccine which, during subsequent years, was primarily used in and around Kabul. Because the vaccine was of questionable potency, as well as being thermolabile, vaccinial immunity in 1967 was probably not high, even in Kabul.
In 1949, Afghanistan began to keep records of the number of cases of smallpox. Between 1949 and 1968, the annual total ranged from a low of 66 cases in 1966 to a high of 2179 cases in 1952. However, the figures had little meaning since the only cases reported were those which were diagnosed in the country’s few health centres. A simple calculation provides an approximation of the probable extent of underreporting. In a population of 10 million, each year about 300 000 would survive the perinatal period to constitute a new group of susceptible subjects. Because few individuals were successfully vaccinated, almost all would eventually become infected with smallpox. Thus, on average, 300 000 persons would experience smallpox each year, either by natural infection or as a result of variolation—i,e., more than 350 times the average of 840 cases reported annually between 1949 and 1963.

Plate 14.1. For hundreds of years, variolation had been widely practised throughout Afghanistan by hereditary variolators using kits such as these. Scabs were collected from a recovering patient and kept in a container such as a metal box (A) or horn (B). Before inoculation, the dried scabs were ground up, usually in a primitive mortar and pestle (B). A liquid such as honey or water with spices was added and a drop of the suspension was applied to the skin. This was then inoculated into the superficial layers of the skin, using a needle or lancet. Sometimes a special strip of cloth (B) was used, and reused repeatedly, to bind the site of the incision until a pustule formed.
Commencement of a WHO-assisted Vaccination Campaign, 1963
Following the Twelfth World Health Assembly’s resolution in 1959 to embark on the global eradication of smallpox, Afghanistan sought and obtained assistance from WHO to begin a special campaign. It was one of only a few countries to receive technical and material support from WHO for field activities in smallpox eradication during the period 1959-1966. A WHO adviser was assigned to Kabul in 1962; in March 1963, a vaccination campaign began in the capital. During the following year, the campaign was extended to 9 provinces (World Health Organization, 1965b). Freeze-dried vaccine provided by the USSR and locally produced liquid vaccine were used. By the end of June 1964, 392 026 of the 400 000 residents of Kabul were reported to have been vaccinated by a staff of 139 male vaccinators and 7 female vaccinators and auxiliary midwives. Twenty-five of the vaccinators were then kept in Kabul “to carry on the maintenance phase and to fight epidemics”, as the WHO adviser reported. The remainder were assigned to the provinces to work under the direction of provincial medical officers. Although large numbers of people were subsequently reported to have been vaccinated, the reports were thought to be greatly exaggerated.
In 1965, 3 additional groups, each composed of 70 vaccinators, were trained and dispatched to Kandahar, Ghazni, Wardak and Bamian Provinces (see Fig.14.3). Young physicians, conscripted for government service, were assigned to supervise each group but few were willing to leave Kabul. What was achieved is unknown because no records were kept.
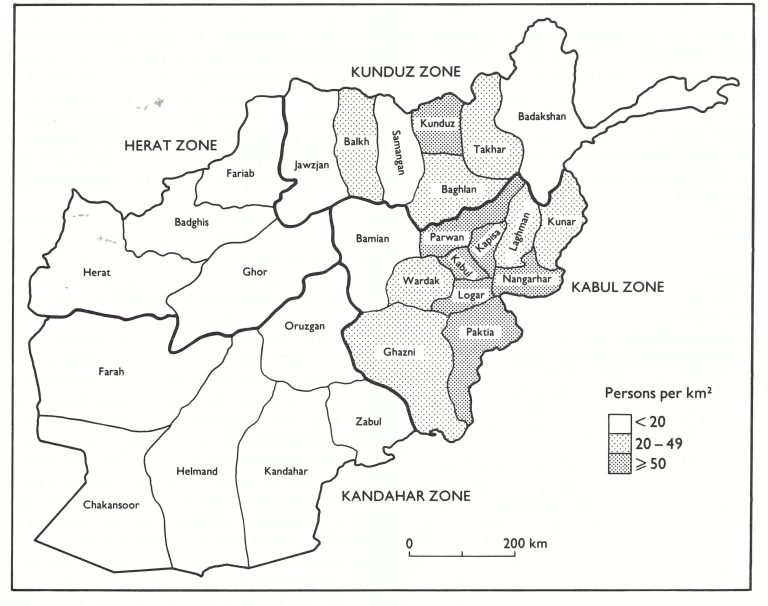
Fig 14.3 Afghanistan: operational zones established for smallpox eradication, and population density by province, 1969.
During the following 3 years, additional resources were provided by WHO, but little progress was made. At the end of 1968, the uncoordinated and poorly supervised series of activities could scarcely be characterized as a programme. The physician in charge of smallpox eradication was also responsible for all the country’s communicable disease control activities and could therefore devote little time to the smallpox eradication programme. Young medical graduates, carrying out their compulsory service, continued to be assigned to provide direction but few spent more than a month or two in the field before arranging to be transferred. In the staff hierarchy there were only a few sanitarians between the programme director and the vaccinators, and the turnover among them was almost equal to that of the physicians. The problems were further compounded by inadequate government funds and a complicated financial system which typically resulted in delays of 3 months or more in the payment of salaries and, frequently, a lack of funds to purchase petrol. Within the government structure, the execution of even simple tasks was timeconsuming. For any purchase, for instance, 3 responsible individuals were required to visit the bazaar to bargain, to obtain a receipt for the purchase, and then to report to an administrative section where the transaction could be recorded. The support provided by WHO contributed little. The WHO smallpox adviser devoted most of his time to the preparation of letters advising his Afghan counterpart as to what should be done and to the compilation of monthly reports. He rarely travelled out of Kabul. Two WHO nurses, assigned to the programme in 1967, likewise travelled little and, although sharing an office with the adviser, received most communications from him in the form of typed memoranda. Eighteen vehicles had been provided to the programme of which 9 were not sufficiently roadworthy to leave Kabul and 7 had been coopted for the use of various officials in the Ministry of Health. In April 1968, a medical officer responsible for smallpox eradication in the WHO Regional Office for South-East Asia reported in despair that no one knew where the provincial vaccinators were stationed or what they were doing. No records were kept, in part because most of the vaccinators were illiterate. The group of vaccinators in Kabul was periodically dispatched to the field when a report of an outbreak was received. They travelled in a large flatbed truck to the site with orders to vaccinate everyone in the area. After some days or weeks had elapsed, they gradually filtered back to Kabul. No report was prepared on what had been accomplished.
Meanwhile, the USA had been approached by the Afghan government and asked to send female volunteers to assist in vaccinating women throughout Afghanistan. Women, it was said, could not be vaccinated by male vaccinators nor could they leave their dwellings in most areas. The volunteers would be expected to work with Afghan women counterparts as members of teams vaccinating from house to house. The concept was attractive but unrealistic. A small contingent of United States volunteers could themselves vaccinate no more than a fraction of the population, and given the religious strictures of the country, the recruitment of Afghan women was all but impossible.
The unsatisfactory vaccine then being used presented no less of a problem. Although liquid vaccine production had ceased in Kabul, the freeze-dried vaccine provided through bilateral assistance did not meet accepted standards, as was attested by protocols provided by the production laboratory itself. Moreover, all vaccine was then being stored at room temperature, which caused it to deteriorate even further.
Finally, the scope of the smallpox problem itself was not comprehended. Early in 1967, the WHO adviser, noting that only 72 cases had been reported in 1965 and 66 cases in 1966, confidently estimated that in the entire country there probably were not more than 300 cases each year, most of them in children. If indeed there were so few cases, it could be inferred that there were comparatively few chains of transmission. Geneva staff, who were ignorant at that time of the moribund state of the programme, hopefully proposed an alternative strategy to country-wide vaccination: (1) intensive containment of known outbreaks by special teams; and (2) a programme of primary vaccination of children in the cities and towns. This, it was felt, might serve to concentrate resources in priority areas and alleviate the problem of supervising vaccinators so widely dispersed over the countryside. No action was taken, however.
When Henderson and Dr Jacobus Keja, of the WHO intercountry team advising on smallpox eradication, visited Afghanistan in October 1968, the full array of problems became apparent. Not only did they discover that the programme existed in name only, but they found that conditions in Afghanistan differed substantially from the situation described in reports and were far more serious than had hitherto been thought. Even with the woefully inadequate notification system, 334 cases were recorded in 1967 and 739 in 1968. Smallpox was far more widespread than had been supposed. Variolation was found to be common and some, perhaps many, of the outbreaks resulted from this practice. The fact that variolators were most active in the least accessible parts of the country was of particular concern. They retained infected scabs for 1-2 years and travelled considerable distances to perform inoculations. Moreover, because the government had begun to discourage the practice, villagers usually refused to identify the variolators, fearing that they would be punished. On the basis of these observations, it was suspected that smallpox transmission, perpetuated by variolation, might persist indefinitely among a remote, comparatively small population of susceptible persons. The optimistic outlook in 1967 that Afghanistan might soon interrupt transmission gave way towards the end of 1968 to fear that the country might prove to be the world’s last and possibly permanent reservoir of smallpox. The previously suggested strategy of vaccinating the more accessible members of the population, coupled with the search for cases and the containment of outbreaks, could not solve the problem caused by variolation. Special efforts would be needed to educate villagers about the hazards of variolation and to identify variolators and persuade them to stop their practice. It was recognized, however, that such efforts would be only partially successful because the identity of variolators was kept secret. Other measures were required. The only possible approach, apart from outbreak containment, appeared to be that of vaccination of the population at large to diminish the number of susceptible individuals available to variolators as clients and as a source of scabs. This would be particularly important in the remote areas in which variolation was most prevalent. Meanwhile, special efforts would be required to characterize epidemiologically all outbreaks so as to uncover evidence of variolation. Considering the poor record of achievement of the programme during the 6 years 1963-1968 the task appeared formidable, perhaps impossible.
Changes in the Strategy and Structure of the Eradication Programme, January 1969
During extended discussions between government officials and Henderson and Dr Keja, a new plan of operations was formulated. The key Afghan officials who provided the essential impetus in the design and implementation of the programme were the perceptive and energetic Dr Sayed M. Saidi, President of Preventive Medicine, and Dr A. Omar, Deputy Minister of Health. An agreement was signed by the government on 12 December 1968 and by WHO 3 weeks later. The plan called for the appointment of a fulltime Afghan medical director who was to be given sufficient authority and responsibility to direct the programme and the establishment of 4 operational zones (Fig. 14.3)—Kabul, Kandahar, Kunduz and Herat—with a zone office in each. A full-time medical officer and 3 sanitarians, assisted by a WHO adviser, would be assigned to each office . Each zone director was to be delegated full responsibility for the programme in his zone, with authority to discipline personnel and to recruit and train replacements, to requisition fuel for transport and pay for repair and maintenance, and to make all necessary travel arrangements for staff within the zone. Although the recommendations were administratively sound, such responsibilities had not previously been assigned to supervisory staff outside Kabul. Despite a conscientious effort to achieve the requisite delegation of authority, the lack of decentralized authority plagued the programme throughout its existence.
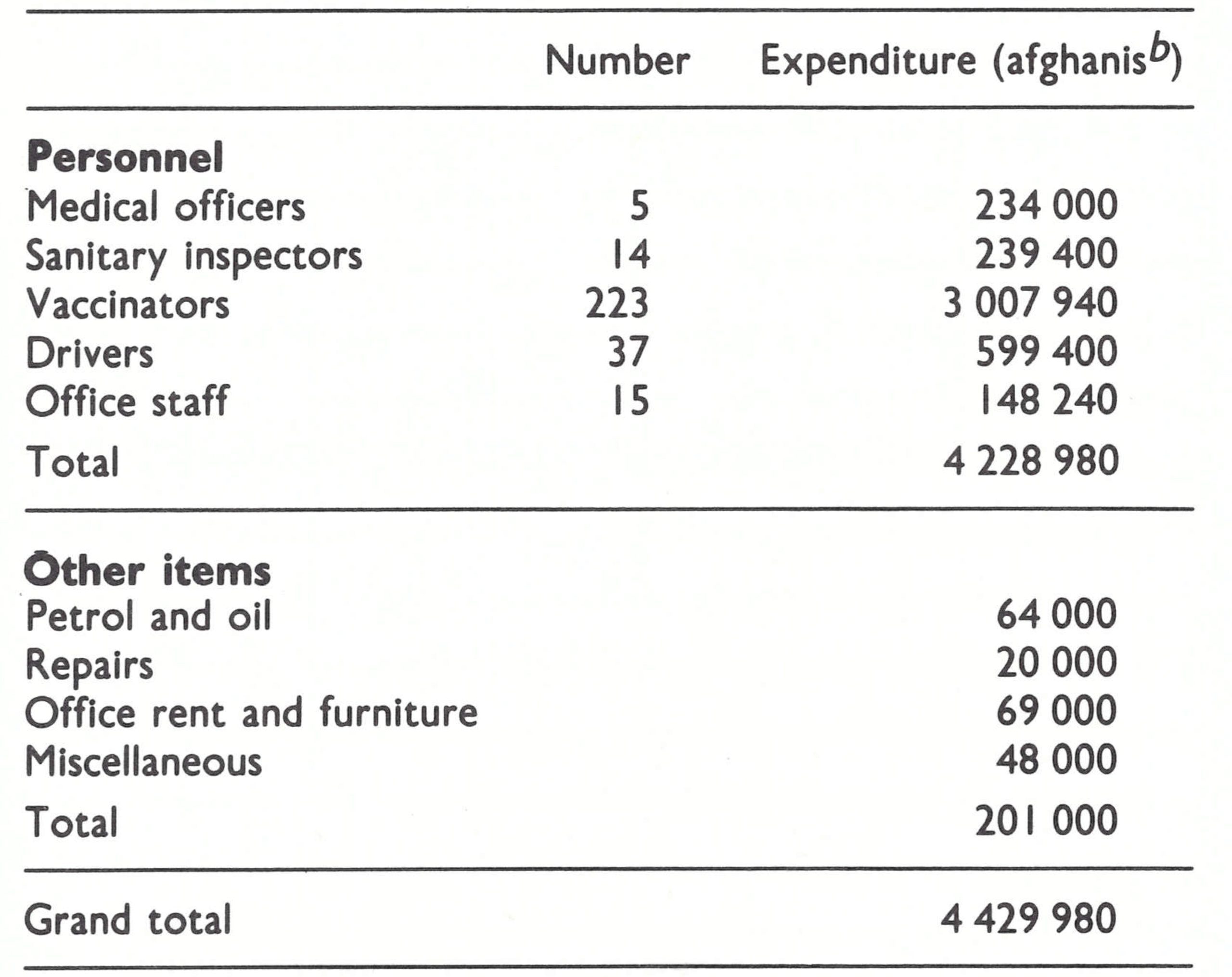
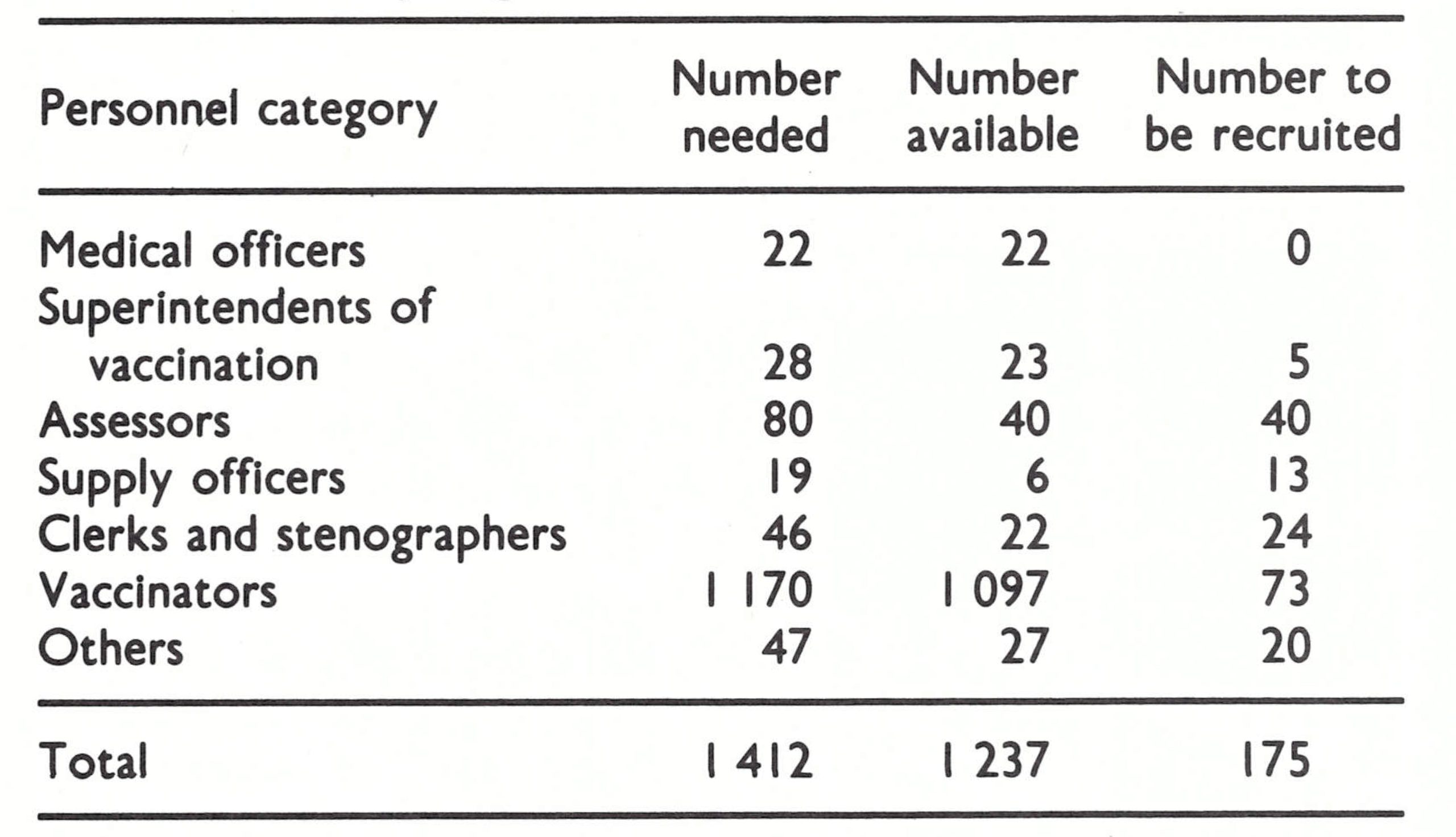
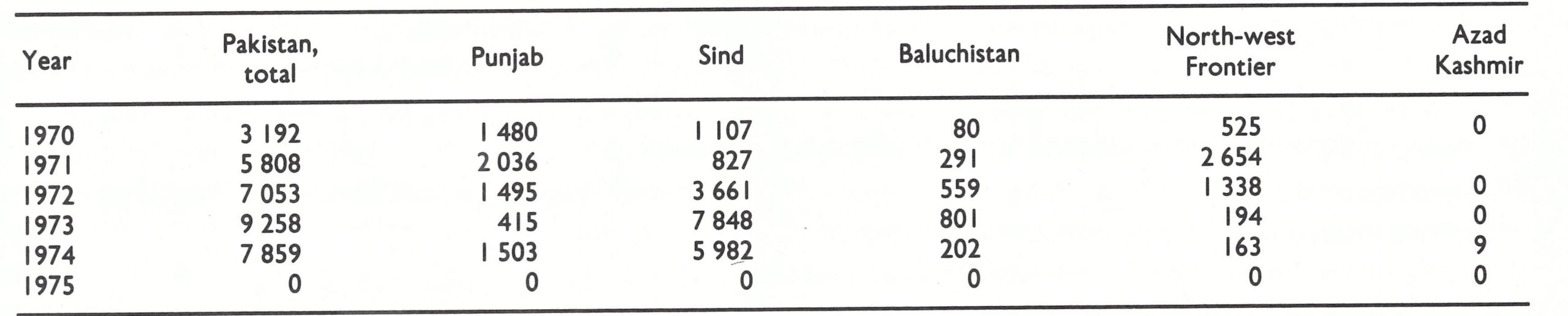
Personnel needs were identified and a budget was drawn up (Table 14.1). With only 4 motor vehicles and 6 motorcycles then available, it was recognized that the programme could not become fully operational until at least August 1969, when the delivery of an additional 44 vehicles, provided by WHO, was expected. Each province was allotted I vehicle each for the zone director, the WHO adviser, an outbreak-containment team and an assessment team, and 5 vehicles for the vaccination teams. Other vehicles were to be kept in reserve.
The plan called for vaccination teams to move systematically from village to village and from house to house, preceded 3-10 days earlier by a visit of the team’s leader to inform village leaders of the programme and to instruct them about the hazards of variolation. Instead of the name of each vaccinated person being recorded, vaccinations would be tabulated by age group on a tally sheet. An assessment team would visit a sample of children in the villages 1-3 weeks later to assess vaccination status, take rates following vaccination and the prevalence of variolation scars. Surveillance-containment teams would visit civil and health authorities in their respective zones to seek cooperation in reporting and to investigate and contain outbreaks.
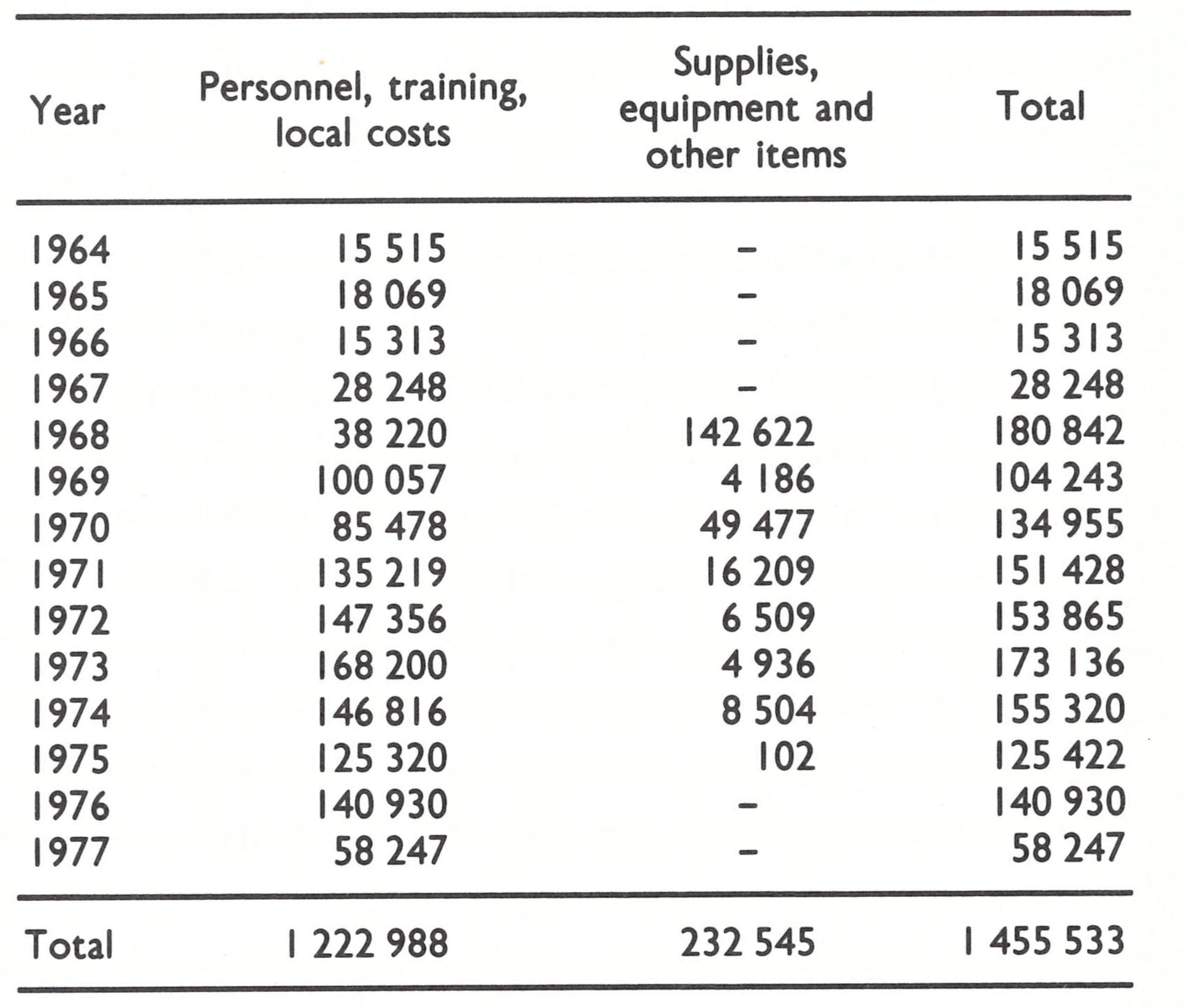
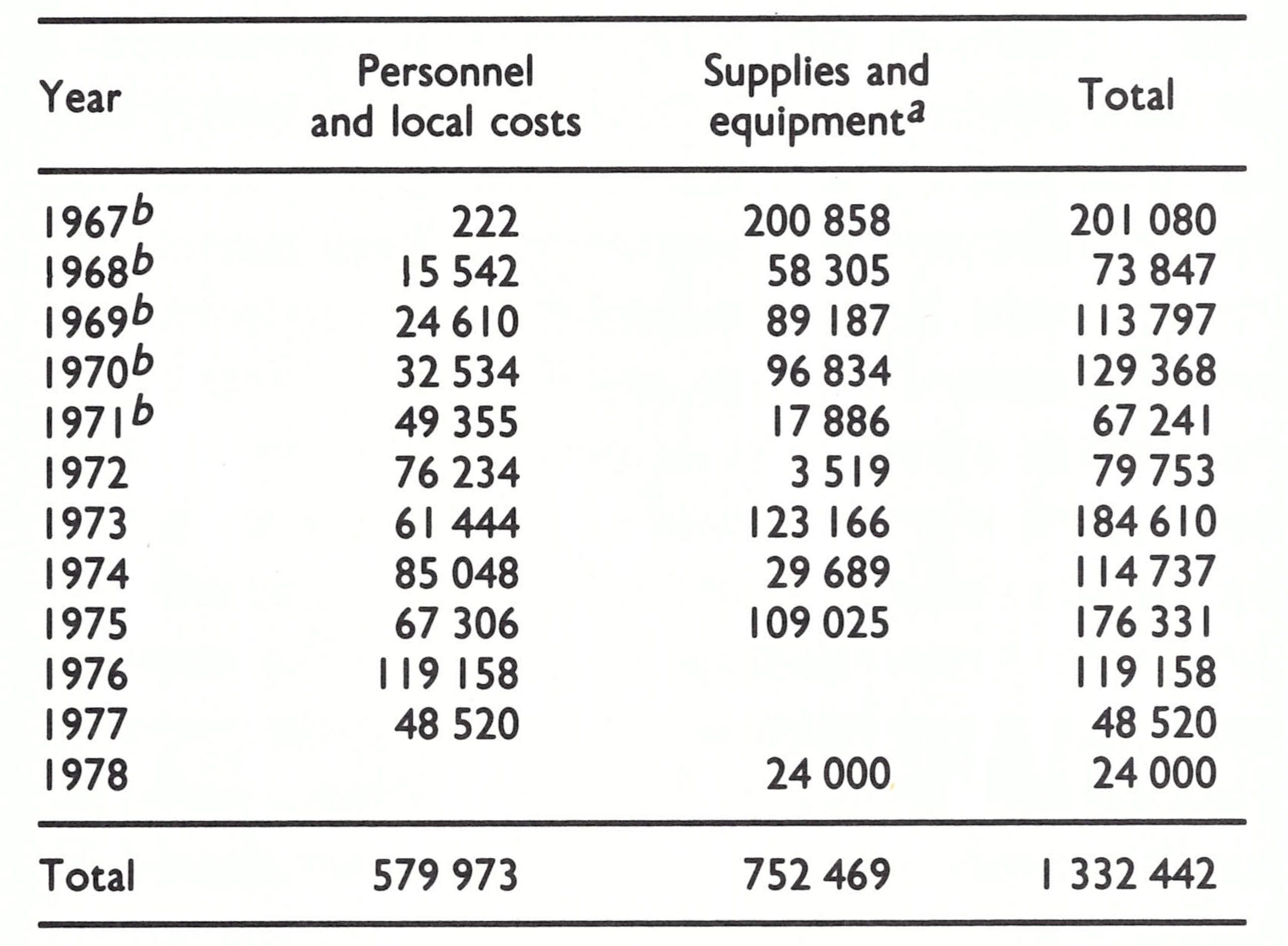
In addition to miscellaneous supplies such as refrigerators and office equipment, WHO agreed to provide up to 4 million afghanis (about US$60 000) each year for travel allowances for headquarters and zone staff and for petrol and vehicle maintenance and repairs. Eventually WHO provided Afghanistan with more than US$1.4 million in support of the programme (Table 14.2), an amount equivalent to about US$0.12 per head of population. In addition, freeze-dried vaccine was provided by the USSR and from contributions received by WHO.
In February 1969, Dr A. G. Rangaraj, a newly recruited senior WHO adviser on smallpox eradication, joined the programme, replacing the previous incumbent. Dr Rangaraj had served with distinction in the Indian Army Medical Service and brought to the programme a unique expertise and capability in programme organization and logistics. With the 2 WHO nurses already assigned, Miss Khin Mu Aye and Miss Ludmila Chicherukina, and later an additional epidemiologist, Dr V.V. Fedorov, an exceptionally effective WHO advisory team was created. In May 1969, the Afghan goverment appointed a no less determined and energetic full-time programme director, Dr Abdul Mohammad Darmanger, who ably fulfilled this role for the next 5 years.
Establishment of zone offIees and effective field activities
Most of the Afghan smallpox eradication programme staff lived in Kabul, and the attractions of urban life discouraged prolonged work in the field. It was felt that a second base of operations, outside Kabul, with staff recruited from the local area, would facilitate field work. An office-cum-dormitory was rented in Kandahar and some work began from this base as early as November 1968. The staff initially consisted of an Afghan medical officer as director, 6 sanitarians, 44 vaccinators, 3 drivers, a cleaner, several volunteers from the USA and the 2 WHO nurses. Work was frequently interrupted, however, because of numerous national and religious holidays and periodic strikes by Afghan staff when they failed to receive salary or travel allowances because of the complicated payment system. Another hindrance was the frequent change of zone medical directors (3 in the first 8 months alone), few of whom were anxious to undertake field work, or to live outside Kabul. Nevertheless, by June 1969, almost the whole population (742 000) of Kandahar, the largest province in the zone, had been vaccinated. Assessment showed that more than 90% of the population had been protected.
It became apparent during this period that, contrary to previous ideas, the 30 United States women volunteers were not essential to the work of vaccination. It was found that when village leaders were properly informed about the nature of the programme, women were usually permitted to be vaccinated by male vaccinators, although sometimes on the forearm or wrist rather than on the upper arm, the customary site of vaccination. From the investigation of outbreaks, it also became apparent that few cases occurred among women, most of whom by the age of puberty had experienced smallpox or had been variolated or vaccinated. Thus, even if some were missed during the vaccination campaign, only a small proportion would remain susceptible. Accordingly, the volunteers were reassigned to assessment and surveillance teams and some helped to establish the necessary administrative and support structure at headquarters and zone offices. They were a dedicated group and made important contributions to establishing the new programme, but when any of them left they were not replaced. Their number had dwindled to 9 by 1970 and to only 1 by 1971.
In July 1969, a third office was established in Baghlan Province, for Kunduz zone, with 2 team leaders, 2 sanitarians and 17 vaccinators. One of the WHO nurses was transferred to Baghlan and several United States volunteers were deputed to work in this office.
Not unexpectedly, a reorganization and reorientation of activities of the magnitude proposed in the plan of operations caused serious difficulties. A joint Afghan-WHO assessment team made an inspection visit in August 1969 and detailed in their report continuing major problems:
- The national programme office had no telephone, secretarial assistance, stationery, files, forms or records. Sanitarians appointed (as administrators) had neither the background nor the skills necessary to discharge their duties.
- The director had no apparent authority—i .e., he had no direct access to a defined budget, no authority either to establish or to enforce personnel policies and no authority to deploy assigned resources (e.g ., vehicles, subsistence allowance) without individual written authorization by his immediate superior. Indeed, his superiors appeared to act independently with smallpox eradication programme resources without prior consultation.
- Only 1 team in 5 in Kandahar zone had worked at all from mid-June to early August and then for only 1 week. In August, 13 of the 53 team members in Kandahar had been sent for military service. Field allowances were not being paid nor were funds available for petrol. These factors were responsible for a strike by vaccinators in Kunduz zone.
- The director’s lack of authority was illustrated by his inability to dispatch a truck to the airport to pick up a vaccine shipment ; this resulted in the vaccine remaining in a hot unventilated shed for 8 days.
- The director had been unable to obtain maps for field operations although the Malaria Institute could do so and tourists could buy them from the Cartographic Institute.
- All teams in Kabul zone had been assigned throughout the summer by Ministry officials to perform cholera vaccination.
- No provincial vaccinators were working with the teams, contrary to prior agreements.
- In Kabul zone, there was no zonal administrative structure and no defined plan of action.
- Vehicles had been out of operation for extended periods and reassigned to other programmes; 2 of 7 large vehicles provided by WHO could not be located, nor could one-third of the motor cycles provided.
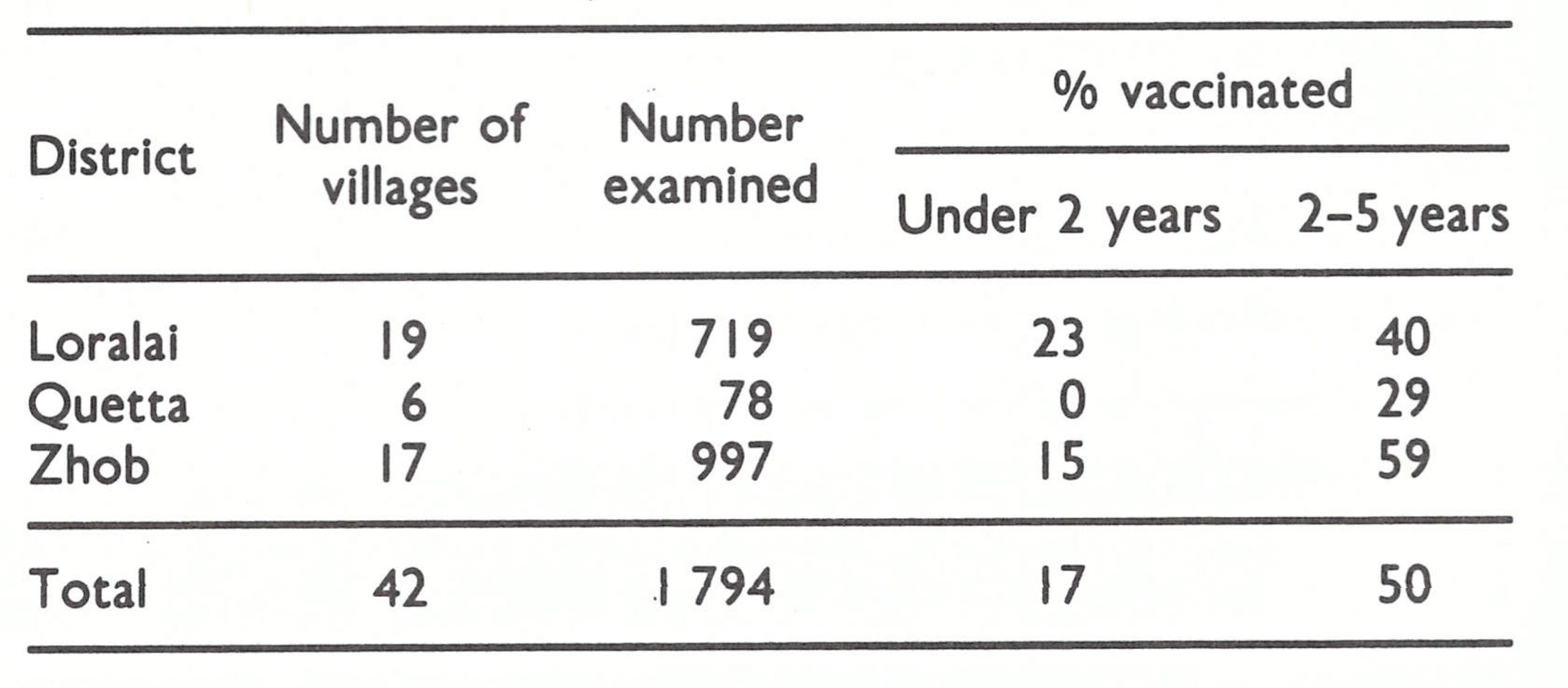
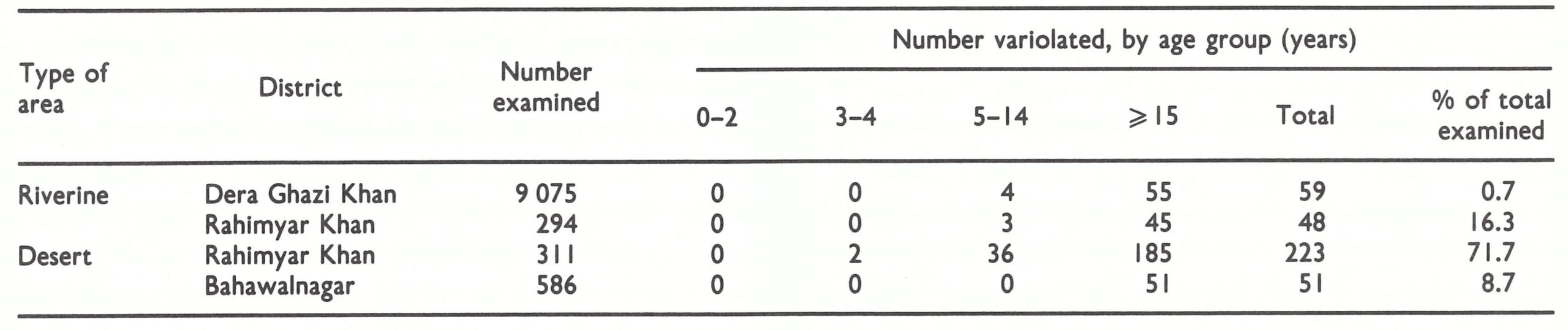
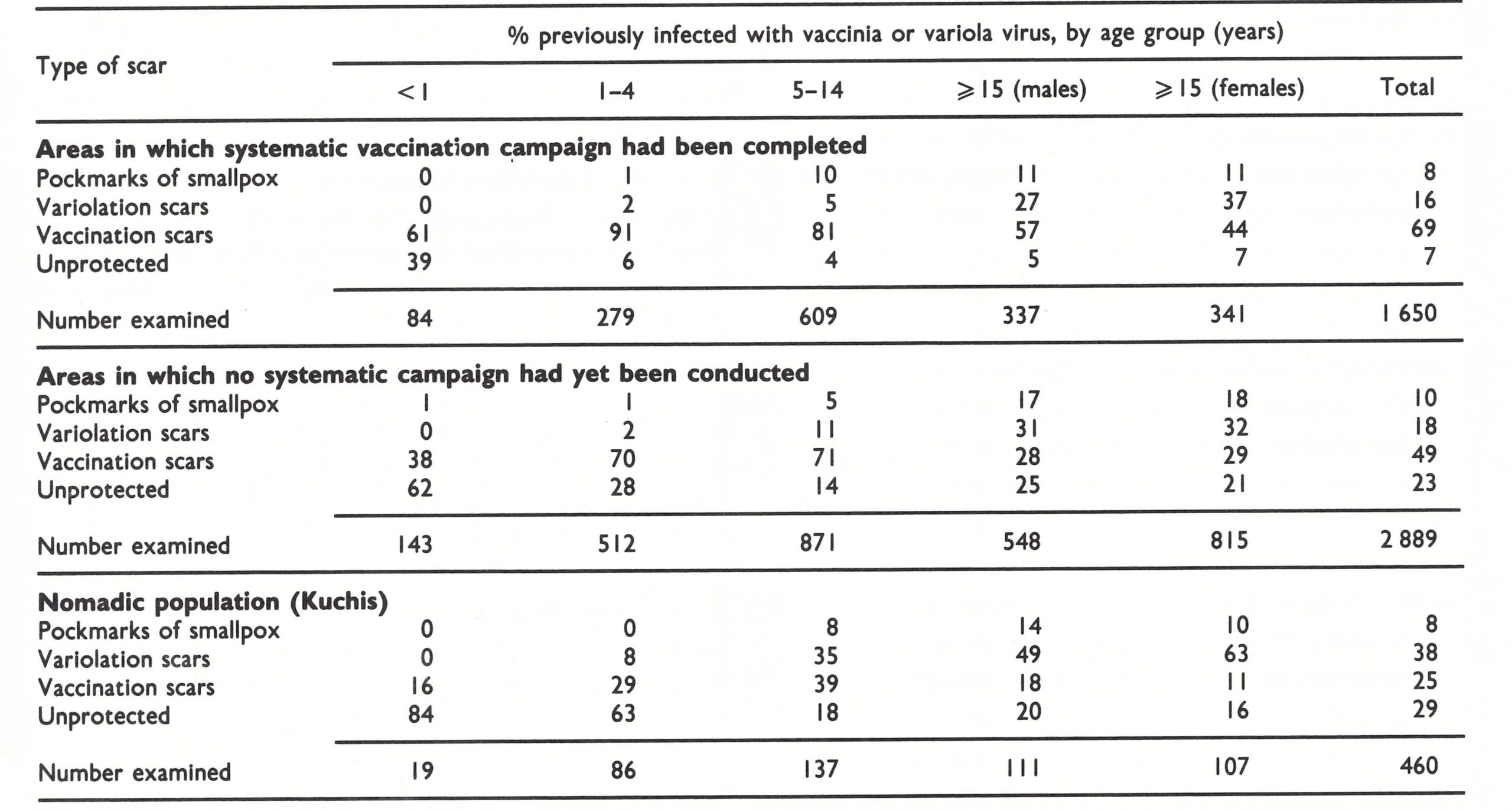
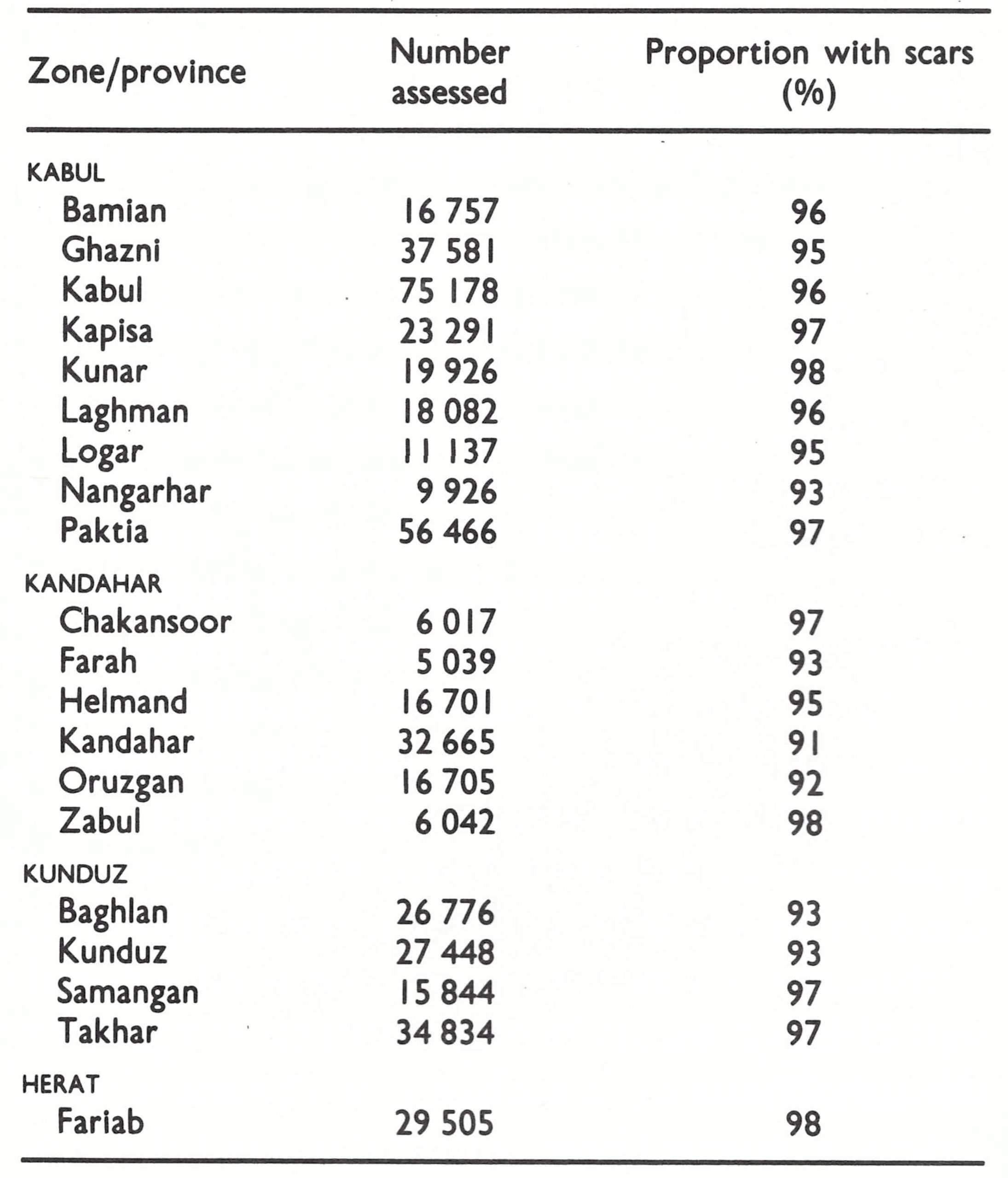
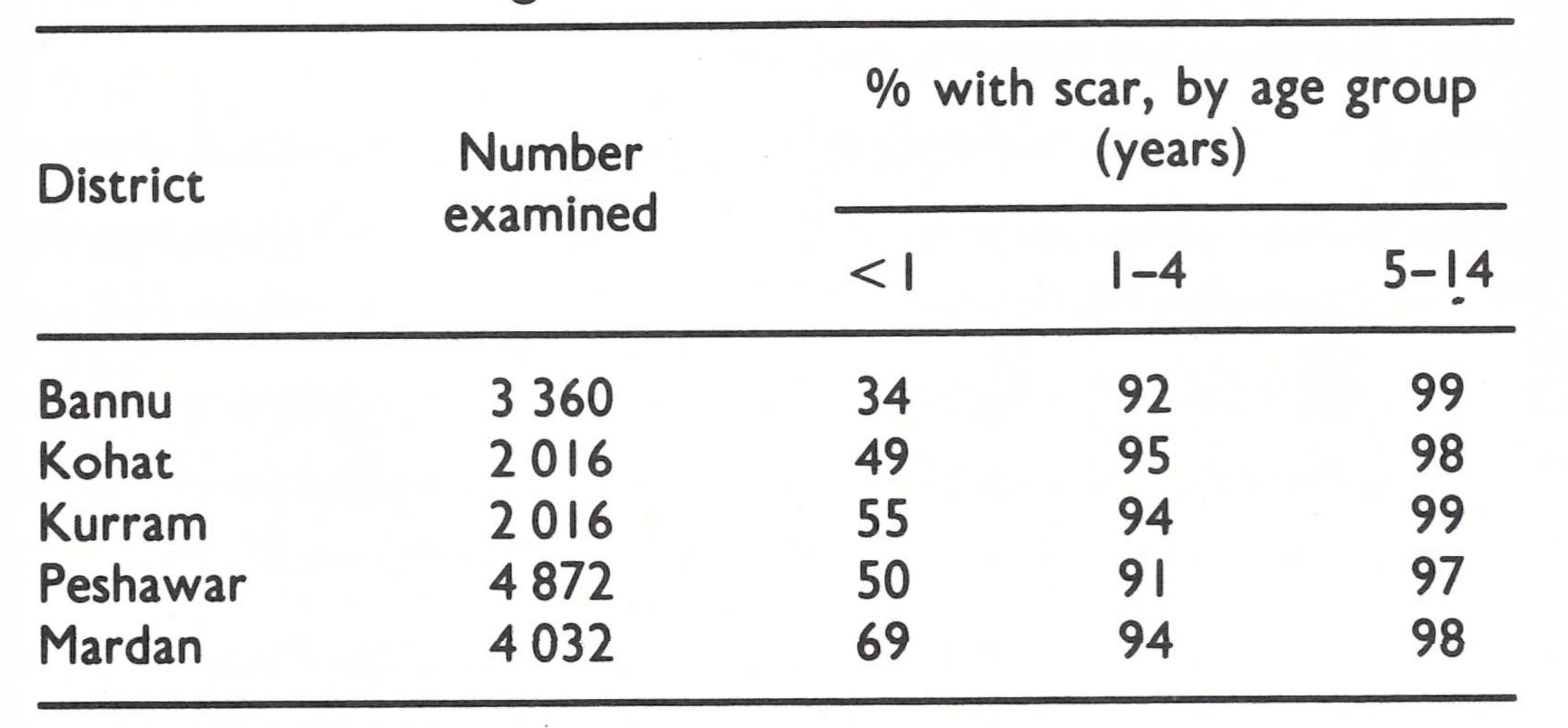
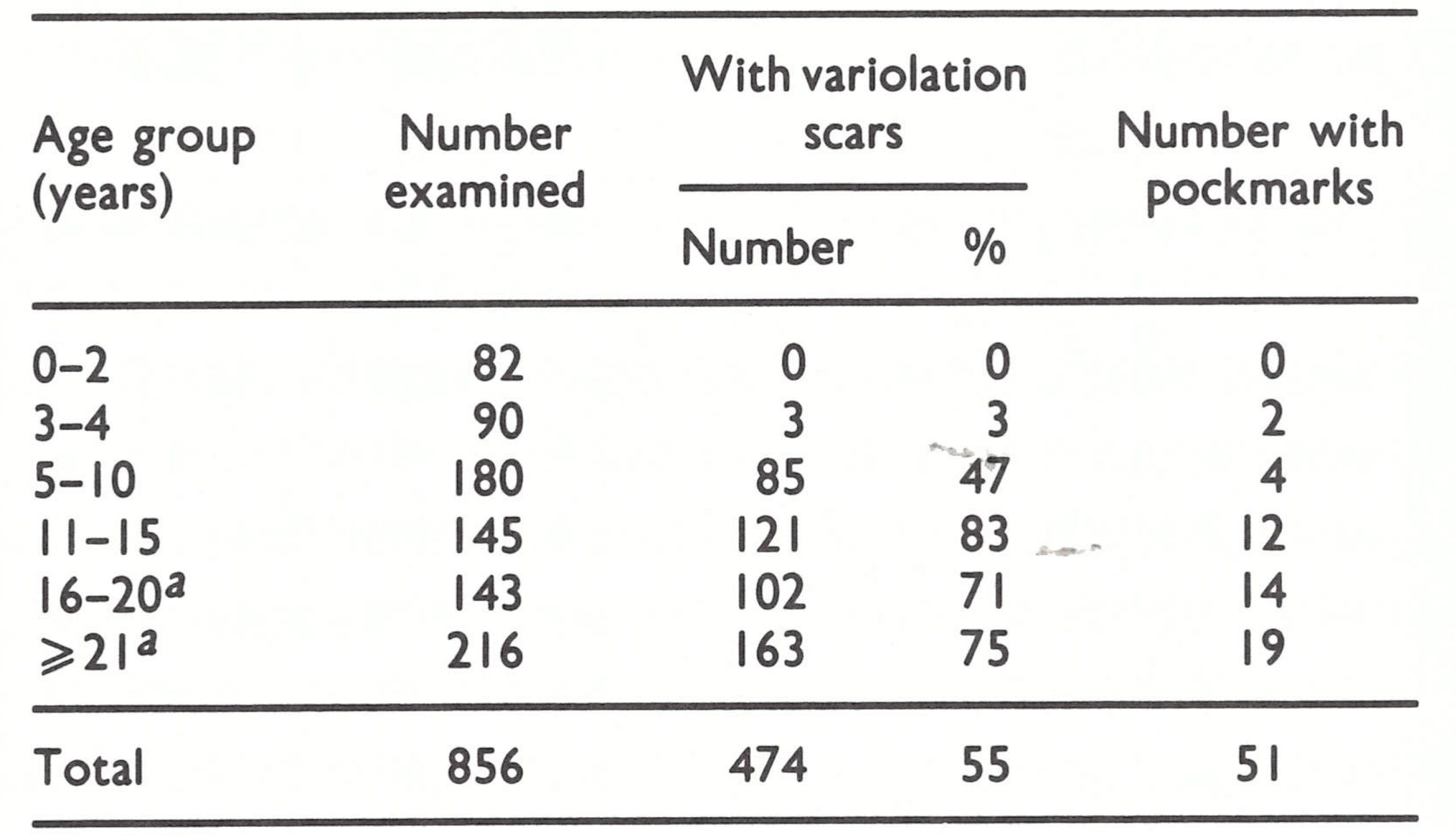
The assessment team travelled widely throughout Afghanistan in August 1969, talking with health staff and others and conducting surveys for evidence of pockmarks and vaccination scars. There were encouraging findings. Everyone with whom they spoke reported that variolation had markedly diminished in recent years, and of 4999 persons examined in their survey, only 3 were found who had been variolated within the preceding 3 years. The reporting of cases was known to be incomplete but, despite intensive search, the team could find no cases not already known to the programme staff. In areas in which the systematic vaccination campaign had been completed, only 7 % of the population remained unprotected (Table 14.3); variolation scars were found in only 5 out of 363 children under 5 years . Even in areas in which a systematic vaccination campaign had not yet been conducted, almost half of the people had vaccination scars and only 23% were unprotected. In nomadic groups, however, only 25% had vaccination scars, nearly 40% had scars of variolation, and 29% remained fully susceptible. The results were encouraging but, at the same time, they had to be interpreted with reservation. Because of time constraints, the assessment teams conducted their surveys in the more accessible areas. Thus, the data undoubtedly indicated a higher level of protection and less variolation activity than might have been expected in the more remote mountainous areas.

Plate 14.2. A: Sayed M. Saidi (1923-1970), President of Preventive Medicine in the Ministry of Health of Afghanistan, provided a new impetus to the programme in 1968. B: Arcot G . Rangaraj (b. 1917) became the senior WHO adviser on smallpox eradication in Afghanistan in 1969 and, with Abdul Mohammad Darmanger, his Afghani counterpart, directed Afghanistan’s first, and highly effective, nationwide health programme. He later served with the smallpox eradication programmes in Bangladesh and in the Arabian peninsula.
Many recommendations were made by the assessment team and gradually, over the next 6 months, order began to emerge. The system of payments improved, greater authority was given to the director of the programme and the pace of operations in the zones increased. Nevertheless, zone directors came and went every few months; the turnover of vaccinators remained depressingly high, as they were regularly summoned for military duty or left for other jobs; efforts to utilize the vaccinators assigned to provinces proved futile.
Methodology of the vaccination campaign
The vaccination campaign was simple in concept but required imagination to execute. Five-man vaccination teams moved systematically through the country, completing their task district by district and province by province. The teams worked for a period of 24 consecutive days, followed by 7 days’ holiday. The senior supervisor, moving in advance of his team, contacted each district and subdistrict political head and, finally, each village chief to explain what the teams were doing and to solicit their cooperation in ensuring that on the day of the team’s visit, the male heads of household would be at home and would agree to let the adult females and children in their household be vaccinated. In most parts of the country, it was possible to vaccinate families only if permission was given by the male heads of household and such vaccination had to be done in the house. The supervisor also explained the hazards of variolation and endeavoured to seek out practising variolators. Variolators, when identified, were sometimes recruited as vaccinators or offered a free supply of vaccine to be used in place of scab material.
A performance goal of 100 vaccinations per vaccinator per day was established . The number was not large, but reasonable considering that many villages could be reached only after hours on foot or horseback, after which each household head had to be individually contacted and his permission obtained to perform vaccination. By the end of 1969, the goal had been achieved by most teams. Initially, the numbers of vaccinations performed were tallied by age group and sex but the vaccinators found it inconvenient to carry paper and pencils and to tally each vaccination performed . A simpler method was adopted. When a team completed work in a village, it simply counted the number of needles used 14. AFGHANISTAN AND PAKISTAN 669 and recorded it, along with the date and the name of the village. The completeness of coverage by age group was determined 1-3 weeks later by an assessment team.
To conduct a systematic vaccination campaign such as this required accurate and detailed maps, but it was soon discovered that the maps provided by the Cartographic Institute and the Malaria Institute omitted many villages and misplaced others. To cope with this problem, the team leader asked each village leader to identify each neighbouring village and its location. These were then added to the map and the map redrawn when necessary.
Methodology for the assessment of vaccination coverage
Assessment of the performance of the vaccination teams played an especially crucial role in the success of the Afghan programme. An assessment team composed of 2 persons visited a 10 % sample of the villages 7-10 days after vaccination to determine the proportion of people vaccinated. Assessment was a new concept that was not readily accepted by the national health authorities. It seemed wasteful to them to assign 2 responsible supervisory staff merely to check the performance of others. They argued, moreover, that if assessment was to be carried out, all persons in every village would need to be examined, an impossible task given the limited resources available. Only with difficulty was it possible to persuade the health authorities of the value of a sample assessment which measured the overall performance of a team in a geographical area.
If only some villages were to be visited, which ones should be selected? One approach would have been to use standard statistical sampling methods, which require that every person has an equal chance of being included in the sample. The correct procedure would then have been to take into account the size of the population in each village in drawing the sample. Given the educational level of the staff, this was considered too complex. Another approach would have been simply to ask the teams to assess 10% of the villages in each geographical area. If this had been done, only the most accessible villages would have been checked, and these would have been the villages that the vaccination teams would also have visited. Not only would a falsely high level of vaccination coverage have been recorded but remote villages in which variolation was prevalent would have been missed. Another scheme was adopted. The name of each village in which vaccination had been performed was written on a piece of paper that was then placed in a box. The assessment team leader drew from the box a number of papers equivalent to 10% of the total, and each of the villages thus selected was then assessed. The process itself was readily understood and it helped to ensure that at least some of the less accessible villages were checked.
Many recommendations were made by the assessment team and gradually, over the next 6 months, order began to emerge. The system of payments improved, greater authority was given to the director of the programme and the pace of operations in the zones increased. Nevertheless, zone directors came and went every few months; the turnover of vaccinators remained depressingly high, as they were regularly summoned for military duty or left for other jobs; efforts to utilize the vaccinators assigned to provinces proved futile.
To facilitate assessment, a simplified form (Plate 14.3) was developed by Dr Keja and Henderson with the assistance of Mr Svend Bragger, a WHO statistician assigned to the Public Health Institute in Kabul. It was decided that in each village chosen for assessment, 85 children under 15 years of age and 60 adults should be examined. Children were the more important group, because it was among them that most cases were occurring. They were also the age group more likely to be encountered when the team visited a village. Because adult levels of immunity were found to be consistently higher owing to previous smallpox or to variolation or vaccination, the assessment of adults was later abandoned. The recording form had 145 boxes, 10 for the age group under 1 year, 30 for the age group 1-4 years, 45 for the age group 5-14 years and 60 for the adult group aged 15 years and over, a distribution roughly approximating to the age distribution of village populations.
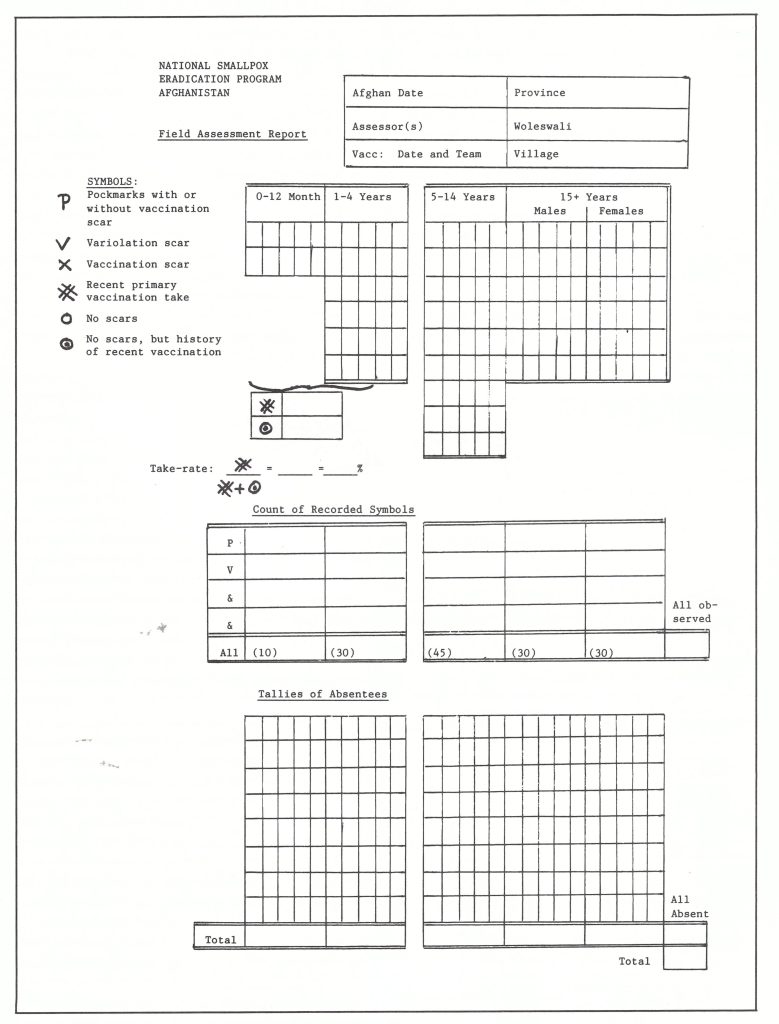

Plate 14.3. Afghanistan: field assessment form, 1969.
The assessor was instructed to begin at one end of the village and to proceed house by house until a sufficient number of persons had been examined so that each box would contain a mark. In examining an individual, he looked first at the face. If there were pockmarks, he recorded a “P” in the box and proceeded to examine the next person. If there were no pockmarks, he looked for a variolation scar on the forearm or wrist. If it was present, he marked a “V” in the box. If neither was present, he looked for a vaccination scar and if he found one recorded an “X”, or “XX” if it was a primary take. If none of these scars was present, he recorded a “0”. He then asked each individual whether he or she had been vaccinated by the team. If the answer was affirmative, a dot was placed within the “O”. When assessment was complete, the numbers of different symbols were summed and a simple calculation was performed. Absentees were tallied at the bottom of the sheet; if they were found to be numerous, the assessment was considered invalid. Experience showed that each team could carry out assessments in 2 villages every day.
With this assessment technique, it was possible to determine the immunity level in the village, the proportion of successful vaccinations, the extent of variolation and the past history of smallpox. The work sheet as well as the final report filled up only one side of a sheet of paper. From the physical condition of the report sheet, it was possible to know whether or not the team had actually performed the assessment: a clean form with all symbols neatly inscribed suggested that the data were contrived.
The method of assessment was not what a traditional statistician would have prescribed and the sample was certainly not “statistically valid”. However, it was understandable to field staff and provided important information. As such, the sample came to be known as “operationally valid”. Eventually, it was adapted for use in many other countries.
Operationally, the goal was established that at least 95% of primary vaccinees should show evidence of a successful vaccination and that not more than 20% of the children under 5 years of age should remain susceptible after a team had vaccinated in a village. Invariably, much higher levels of protection were found among individuals over 5 years of age. Thus, if fewer than 20% of those under 5 years remained susceptible, the overall proportion of susceptible people in the village would be much lower than this, usually less than 10%. If the assessment team found that more than 20% of children under 5 years were susceptible or that the proportion of successful vaccinations was unsatisfactory, the vaccination team was obliged to return to the area to revaccinate the population of all the villages, but its members were not paid a travel allowance. Within months after the assessment teams began work, the proportion of susceptible young children remaining after mass vaccination dropped abruptly from a range of 20-40% to consistently less than 10% and often less than 5%.
Progress in the Vaccination Campaign
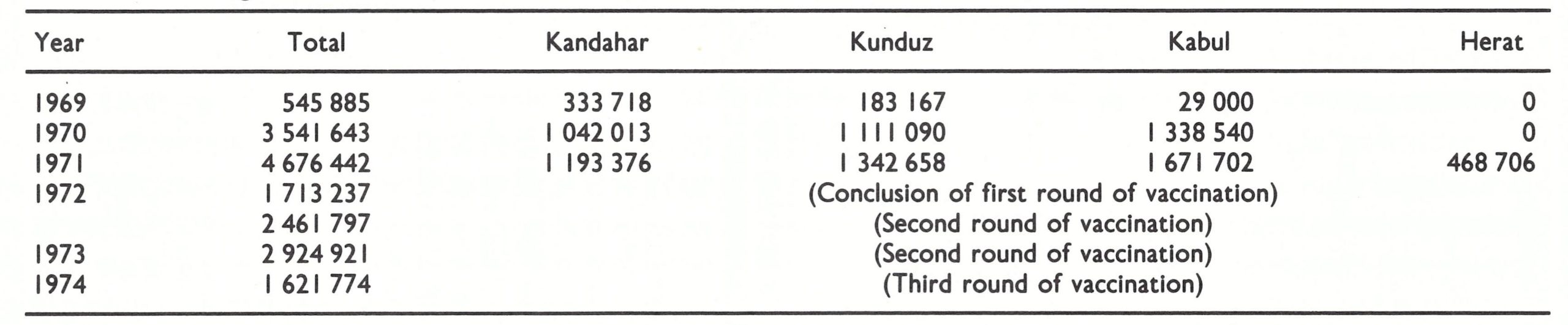
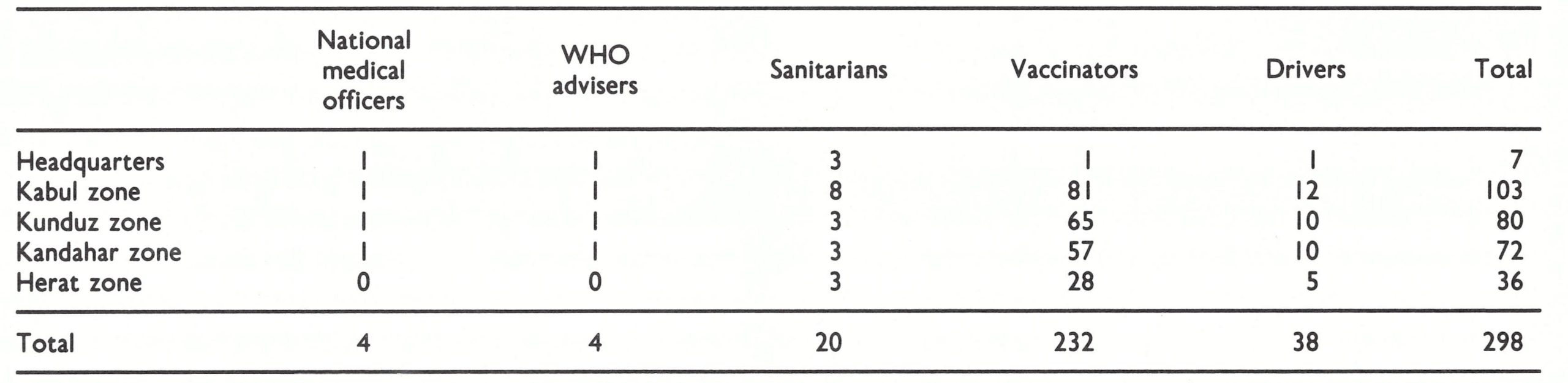
Because of the host of administrative problems and the lack of transport, progress in the vaccination campaign remained unsatisfactory during 1969 (Table 14.4). Only 545 885 persons were vaccinated during the year, two-thirds of whom were in the Kandahar zone. Vaccination was completed in only 3 provinces (Fig. 14.4). However, as systems improved and operations in the Kunduz and Kabul zones got under way, the pace accelerated. By July 1970, more than 300 000 people were being vaccinated each month. During 1970, 3 541 643 vaccinations were performed and work was completed in 10 provinces (Fig. 14.4). Activities extended to Herat, the 4th zone, in 1971 and 4 676 442 vaccinations were performed during the course of the year. By the end of 1971, campaigns had been carried out in all but 4 provinces, and by June 1972, the first round of vaccination had been completed. In all, 10.5 million people had been vaccinated by a staff which at its maximum numbered only 298 persons (Table 14.5). The population of Afghanistan in 1972 was estimated by the government to be 17 million but, in the absence of a census, the actual number was unknown. The data of the smallpox eradication programme suggested that a population estimate of no more than 12-15 million persons would be more realistic.
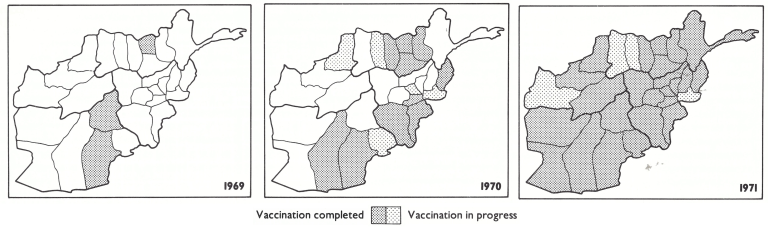
Fig 14.4. Afghanistan: status of the vaccination campaign, by province, in December 1969,1970 and 1971.
On completion of the first round of vaccination, it was decided to undertake a second round, but to vaccinate only those under 15 years of age. The objective of this round was not so much to improve the immune status of the population as to ensure the continued mobility of the vaccination teams, who could both search for cases and detect the presence of variolators in the course of their work. The second round of vaccination was completed in 18 months, during which 5.4 million persons were vaccinated (see Table 14.4). The shorter time required reflected, in part, more efficient programme operations; of greater significance was the fact that village leaders were far more helpful and the villagers more receptive. After the second round of vaccination had been completed, it was decided to perform yet a third round, again to ensure a continuing search for cases and the detection of variolators. During the third round, only children under 5 years of age were vaccinated. This phase of vaccination was completed in just over a year, during which 1 621 774 individuals were vaccinated. Cooperation had progressed to such an extent in some areas that villagers assembled young children at collecting points, thus obviating the need for vaccinators to visit each house.
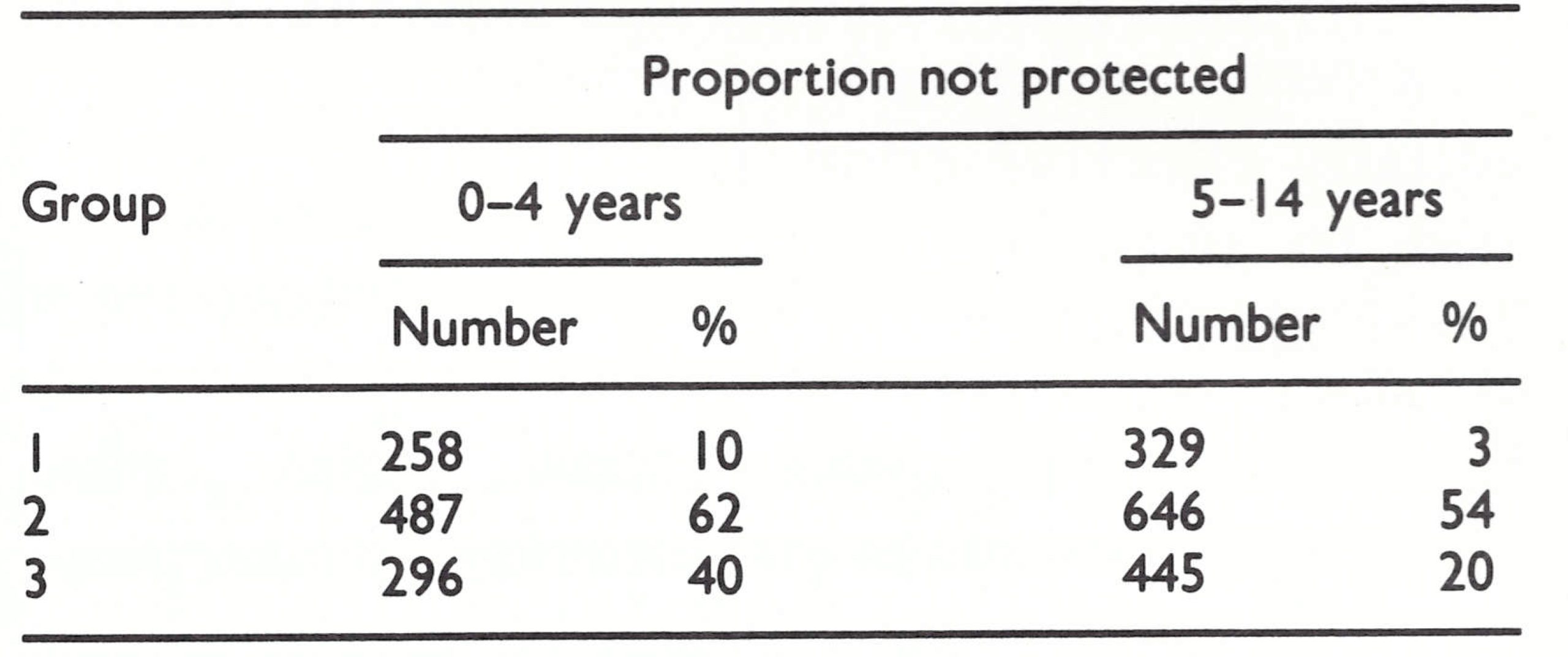
The nomadic and semi-nomadic Kuchis, who were estimated to number more than 2 million, presented a special problem. Entire families wintered in lowland pastures in southern Afghanistan and Pakistan, and, with their herds, moved to upland pastures in the spring. On the way, they travelled in large bands along comparatively well established routes, but once settled, they scattered widely, often in virtually inaccessible areas. Although, when settled, they readily accepted vaccination, they resisted it while travelling, fearing reactions to the vaccine . Many were vaccinated during the course of the systematic campaign but, as shown in a survey of Kuchis in Helmand Province in 1971, vaccinial immunity differed greatly from one group to another (Table 14.6). To ensure more complete coverage, a special summer programme was conducted during 1973 in Ghor and Bamian Provinces, in which the largest proportion was settled.
At the conclusion of the second round of systematic vaccination in 1973, the overall levels of vaccinial immunity in Afghanistan were assessed during a special programme. The levels of protection were among the highest found in any country (Table 14.7).
A Smallpox Surveillance Team
The investigation of a rumoured outbreak in November 1970 in the mountainous province of Oruzgan illustrates the pride and dedication that the teams developed. A team was sent on horseback to elicit information about the outbreak. On its way up a mountain, it encountered metre-deep snow and was forced to turn back. The team then approached the area by another route. Again, it encountered snow; the horses were abandoned and the team members continued on foot for 4 days to get to the villages. They stayed in the villages, moving from one to another to vaccinate. In all they spent 6 weeks vaccinating the inhabitants of villages in the middle of winter in the Oruzgan mountains. When it was possible to carry out a thorough search of the area in the spring, no cases of smallpox were found.
The Elimination of Smallpox : Epidemiological Patterns, 1969
Given the many problems and obstacles, the rapid development of a highly effective campaign of systematic vaccination was an extraordinary achievement. Programme staff, however, undertook at the same time an equally effective effort to improve reporting and to investigate and contain outbreaks. They decided that from September 1969, every reported case of smallpox would be investigated by a zonal containment team, usually accompanied by senior national and WHO staff. The Afghan programme was one of the very few in which both mass vaccination and surveillance-containment measures were simultaneously and successfully conducted.
To improve reporting, provincial medical offices were directed by the Minister of Health to report any suspected case by telephone or telegraph either to the national smallpox eradication office in Kabul or to the zone office. At the same time, the President of the Malaria Institute directed all malaria workers to report cases of smallpox. Meanwhile, programme staff began regular visits to each hospital, health centre and clinic to explain the programme and to ask that every suspected case or rumoured outbreak of smallpox should be reported promptly. Because only 69 out of 326 subdistricts had a health unit and because the malaria programme was not operational throughout the country as a whole, and not notably effective, additional measures were required. Zonal surveillance teams began systematic visits to the subdistrict civil authorities, the maliks and arbabs, to solicit their help and to visit the few existing schools. Each report of a case was investigated promptly by a surveillance team. The promptness of response provided tangible evidence to those reporting that the programme personnel were genuinely interested in receiving reports, and this gradually became widely known. Indeed, some villages which sought vaccination sent false reports, knowing that the report of a case would quickly bring a surveillance team to the village.
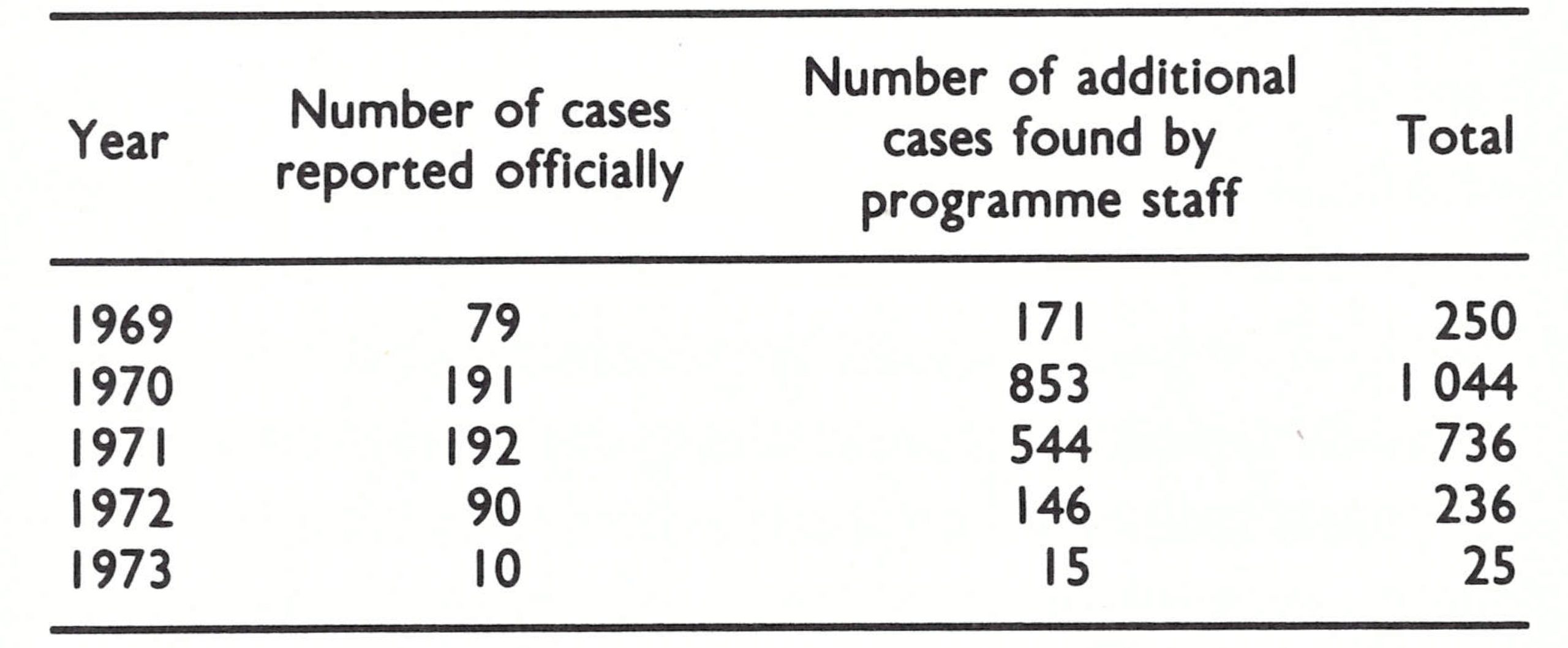
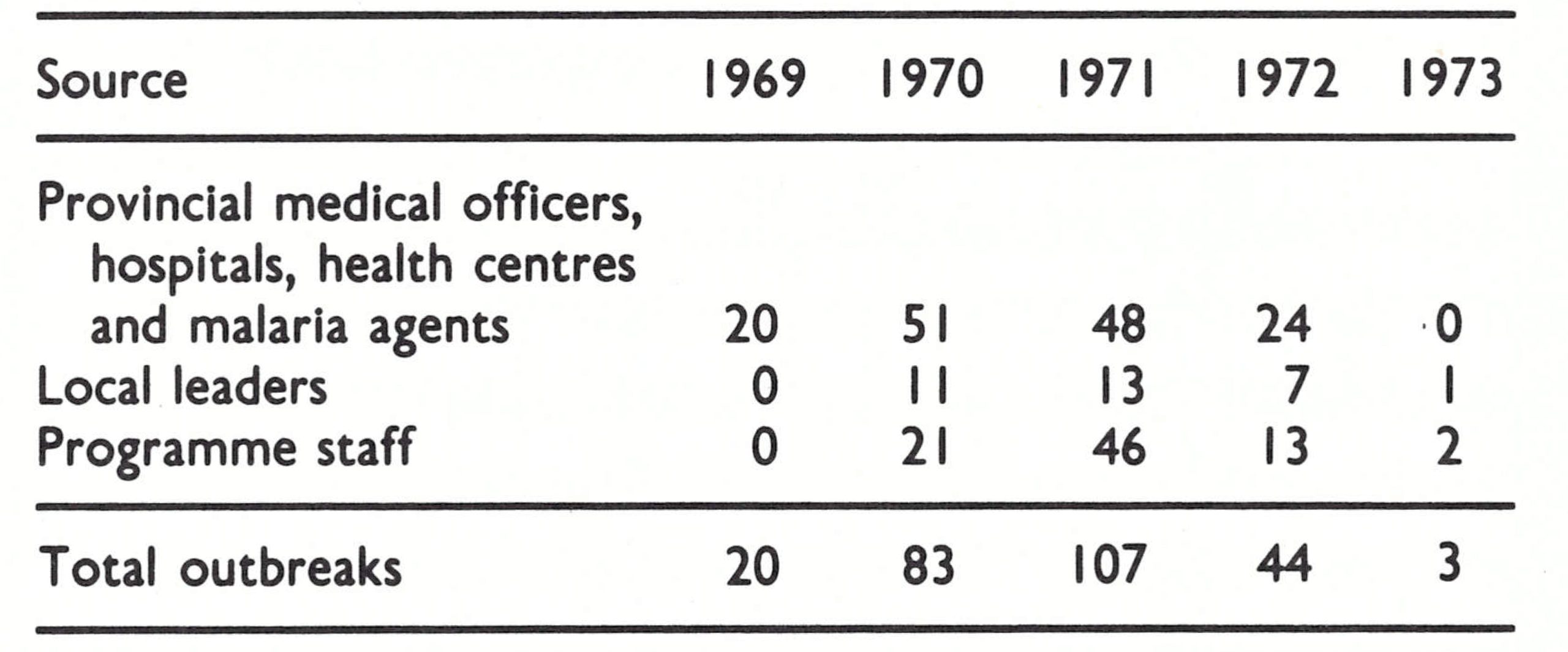
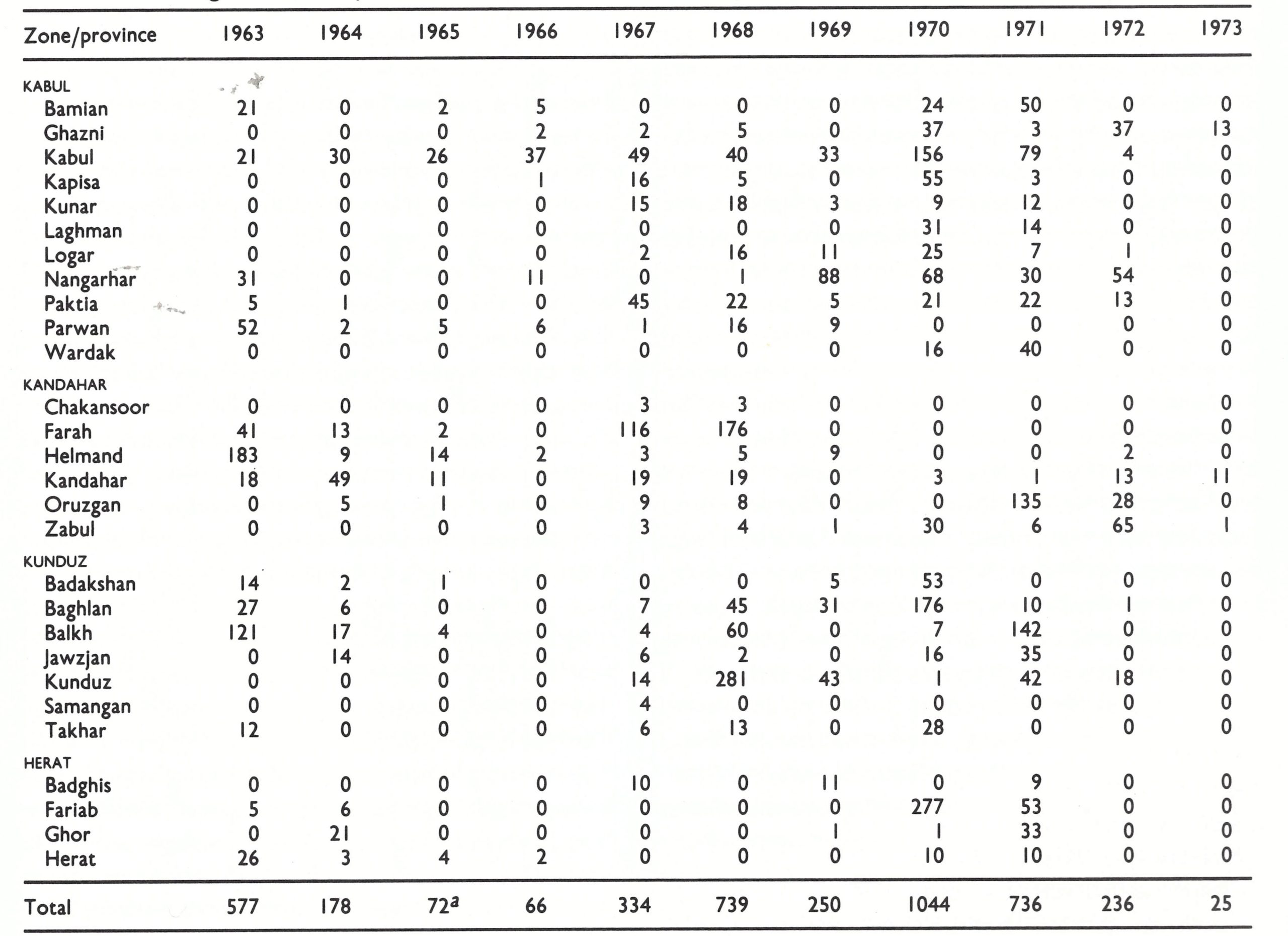
During the last 4 months of 1969, 22 reports of smallpox were received, of which 20 were verified to be outbreaks. In all, 79 cases were reported but the surveillance teams found an additional 171 cases during investigation (Table 14.8). In the course of 1970, with reports being received from many additional sources (Table 14.9), the number increased to 1044 cases in 83 outbreaks. This was the highest total of cases recorded in Afghanistan since 1955. Cases were recorded in 21 of the 28 provinces (Table 14.10) and, as was the case in other countries, the apparent epidemic of smallpox (Fig. 14.5) alarmed the national authorities and fostered substantially greater support for the programme.
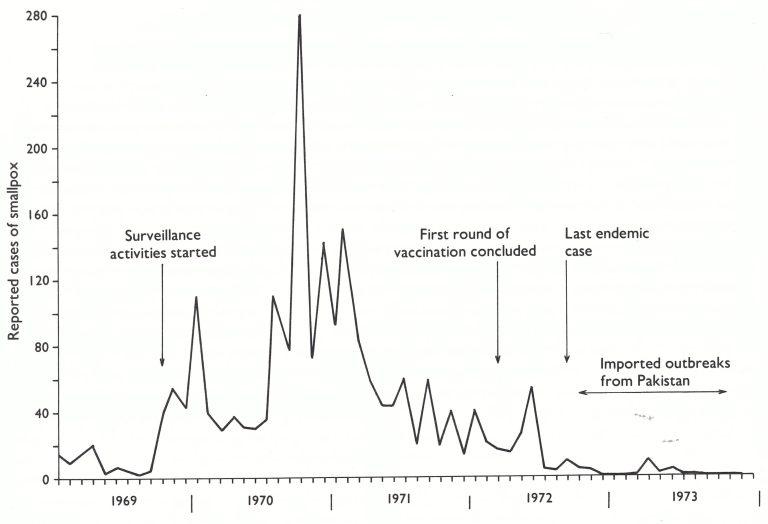
Fig 14.5. Afghanistan: number of reported cases of smallpox, by month, 1969-1973.
Special concern was caused in 1970 by the increasing number of cases in the city of Kabul, and a number of outbreaks in other provinces which were traced to this source. In all, 156 cases (15 % of all cases in Afghanistan) were reported from Kabul, most of which occurred in the congested poorer quarters of the city in which visitors from rural areas often stayed. Originally, vaccination in Kabul had not been planned since extensive vaccination campaigns had repeatedly been conducted there between 1962 and 1968. Because of the outbreaks, however, a special campaign was carried out during the winter months of 1970-1971. As in many other cities, the infectious diseases hospital itself proved to be a problem, 5 of the outbreaks resulting from the spread of smallpox within the hospital. One of the people infected was a Danish student, admitted because of suspected typhoid fever, who developed smallpox after returning to Copenhagen (see Chapter 23). This problem of hospital infection was eventually solved when smallpox eradication staff were assigned to the hospital to ensure the isolation of patients and the vaccination of all people admitted, for whatever reason. With these measures, Kabul and its infectious diseases hospital ceased to be a problem. First round of Last endemic vaccination concluded case Imported outbreaks from Pakistan 1971 1972 Fig. 14.5. Afghanistan: number of reported cases of smallpox, by month, 1969-1973.
The number of outbreaks increased from 83 in 1970 to 107 in 1971, but only 736 cases were found on investigation, substantially fewer than the 1044 cases recorded in 1970.
In 1972, outbreaks were reported in only 11 provinces and the numbers of cases and outbreaks diminished rapidly. Between January and June, 10 provinces recorded 196 cases in 39 outbreaks. After June, smallpox was detected only in the southern provinces of Oruzgan, Kandahar and Zabul, the last indigenous cases occurring in Oruzgan in September, just 36 months after the surveillance-containment programme began. Later in the year, 1 outbreak occurred in Zabul and 2 in Kandahar whose sources of infection were, respectively, the towns of Pishin and Quetta, both in Pakistan.
The Final Outbreaks
Between October 1972 and April 1973, no evidence of endemic smallpox was found despite active search and the investigation of many rumours. However, 3 more outbreaks were yet to be discovered: 2 in April and 1 in June. The following brief descriptions of these outbreaks and how they were discovered, investigated and contained illustrate some of the challenges experienced by the Afghan staff.
Ghazni Province, Abramhel village
On 10 April 1973, a mobile vaccination team heard rumours from villagers of suspected cases in Wor Subdistrict, 85 kilometres away. The team leader and his supervisor went to the area the following day and in the village of Abramhel, 5 kilometres from a barely motorable road, found 3 active cases and 3 close contacts with fever, and learned of a person who had died of the infection. The village, consisting of 9 households and 56 persons, was one of a number of small, widely scattered villages situated on barren mountain slopes rising above an arid plain. A search of this and 12 neighbouring villages began immediately along with containment vaccination. In all, 2411 persons were vaccinated. Systematic vaccination had been conducted throughout the area 3 years earlier but this group of villages had been missed. The first case was that of a 23-year-old man who had travelled some 600 kilometres to the town of Sukkur in Pakistan in search of work (Fig. 14.6). He arrived back in his village after more than a year’s absence, became ill with smallpox and died. In all, 13 cases eventually occurred, 2 of whom had old variolation scars and 7 of whom were vaccinated during the incubation period. Three of these persons died.
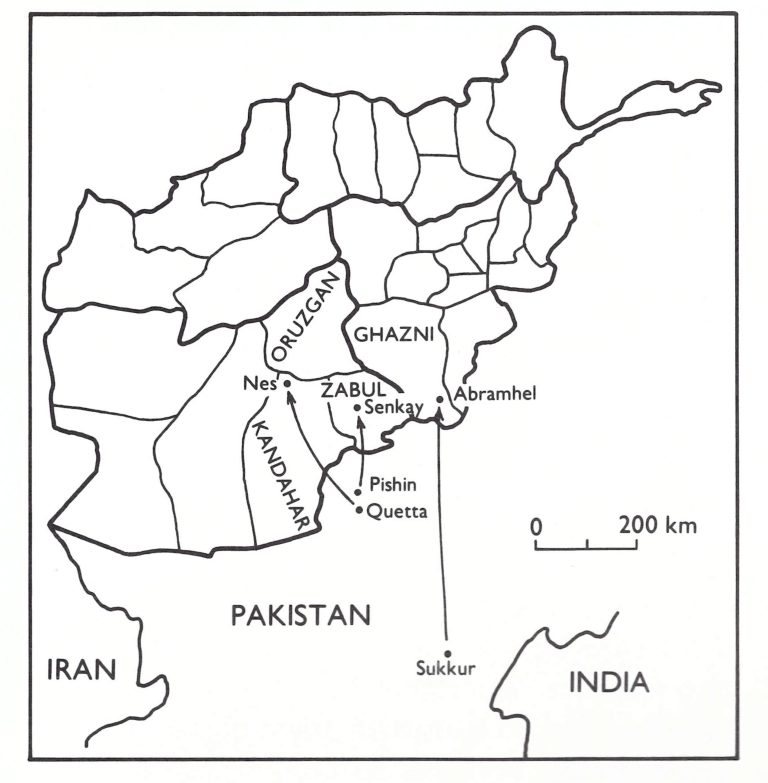
Fig . 14.6. Afghanistan: sources of infection and location of outbreaks, 1973.
Zabul Province, Senkay Woleswali (district)
Fearing that Kuchi nomads might reintroduce smallpox during their spring migration from Pakistan, smallpox eradication teams in 1973 endeavoured to intercept groups of Kuchis in order to detect cases and vaccinate the others. On 29 April, a surveillance team found a 10-year-old child with smallpox among a group which was travelling from Pishin in Pakistan to its summer home in the mountainous province of Oruzgan. Only 5 of 140 persons in the group had not been vaccinated; the patient was one of the unvaccinated. The boy and his mother were isolated in the zone office and 2 vaccinators were assigned to travel with the Kuchis to detect any further cases that occurred. The Kuchis, who were smuggling cloth, feared that they might be reported and left silently, leaving the mother and child and 2 sleeping vaccinators. Angered by this, the mother revealed the intended route and destination of the band, and a vaccination team again intercepted them to keep them under surveillance for 6 weeks. No further cases occurred.
Kandahar Province, Nes Subdistrict
As happened in several countries, the final outbreak was marked by delays and failures in reporting in what was then thought to be a reasonably effective system of notification and containment. On 3 July 1973, the zone office in Kandahar was informed that a number of deaths had occurred in a Kuchi nomad camp some 90 kilometres to the north. Five days had elapsed since the commandant of police at Nes had telephoned this information to police headquarters in Kandahar. The provincial medical officer was notified the same day and he immediately sent a laboratory technician to investigate. The technician returned on 30 June to confirm that the outbreak was smallpox. Instead of directly informing the zone office, a few blocks away, the provincial medical officer wrote a letter to the office on 2 July which was received late the next day. On 4 July, the zone team went to Nes, where they found a Kuchi camp of 45 persons living in 7 tents. In all, 11 cases with 5 deaths had occurred. Surprisingly, a local malaria surveillance agent had visited the camp several days earlier, vaccinated a few people and departed without notifying anyone. Meanwhile, on 2 July, a variolator who lived in Nes had visited the camp, gathered scabs from one of the patients, variolated 10 persons and departed for another province. The team conducted an immediate search and vaccinated the population of the subdistrict, performing some 2300 vaccinations in all. Nine of the 11 cases were among adults. Systematic vaccination had been completed in the subdistrict only 3 months before, but at the time of the team’s visit, only the children and a few women had been in camp, the men having gone far ahead to prepare the next campsite. The first case in the outbreak had been that of a 35-year-old man who had accompanied his uncle to a hospital in Quetta, Pakistan, and had developed smallpox after his return. A cable to Quetta confirmed that at the time of his visit, cases were present in the hospital. Thus, the last known outbreak in Afghanistan was traced to infection probably acquired in a hospital; the report of the outbreak and its containment were delayed by a full 5 days because of poor communication; a health worker who should have reported the cases failed to do so ; the men in the camp who should have been vaccinated only 3 months earlier were missed because they had travelled to another area ; and a variolator was given the opportunity to acquire scabs. Despite extensive search the variolator was never found nor was another case of smallpox detected in Afghanistan.
Conclusion of the Programme
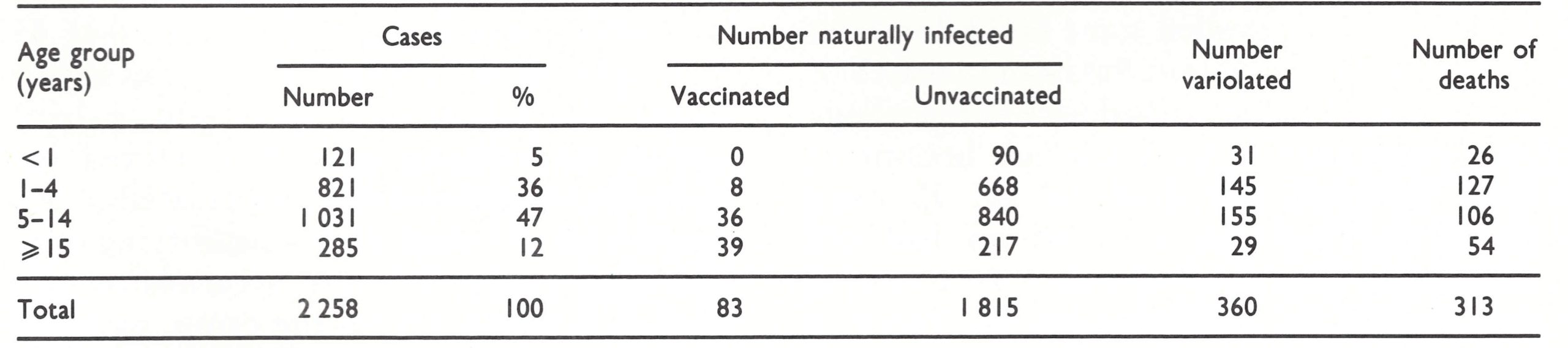
The last outbreaks in Afghanistan were cause for celebration, but with smallpox still endemic in Pakistan and with the spectre of its possible recurrence through the practice of variolation, programme staff could not relax their efforts. The tens of thousands of nomads who began their annual trek northwards out of Pakistan in late February and March were of particular concern. In 1973, the number of surveillance teams in southern Afghanistan was increased and a special programme was begun to intercept nomads during their travels. During this period, different surveil Table 14.11. Afghanistan: reported number of cases of and deaths from smallpox, by age group, 1969-1973a a Excluding 33 cases for which data are not available. lance teams succeeded in intercepting some nomadic groups so often that the leaders of the groups protested against the harassment. To deal with the problem, it was decided to issue a special certificate to the leader after all members of a group had been examined, provided that they all accepted vaccination. When subsequently intercepted by another surveillance team, the group leader simply presented the certificate, assuring the nomads of the right of passage without further examination. Happily, the procedure was well accepted.
Meanwhile, the systematic vaccination campaign was continued, primarily to sustain a continuing search for cases but also to keep the number of susceptible persons as low as possible and so diminish the chance of variolation being revived. In fact, as late as 1976, evidence of attempted variolation was found, but no successful variolations are known to have occurred following the last outbreak in 1973.
Finally, after the interruption of smallpox transmission in Pakistan in October 1974, a reward of 1000 afghanis (US$18) was offered to anyone reporting a case. The number of rumours and reports of suspected cases increased dramatically but, on investigation, none proved to be smallpox.
Epidemiological Data
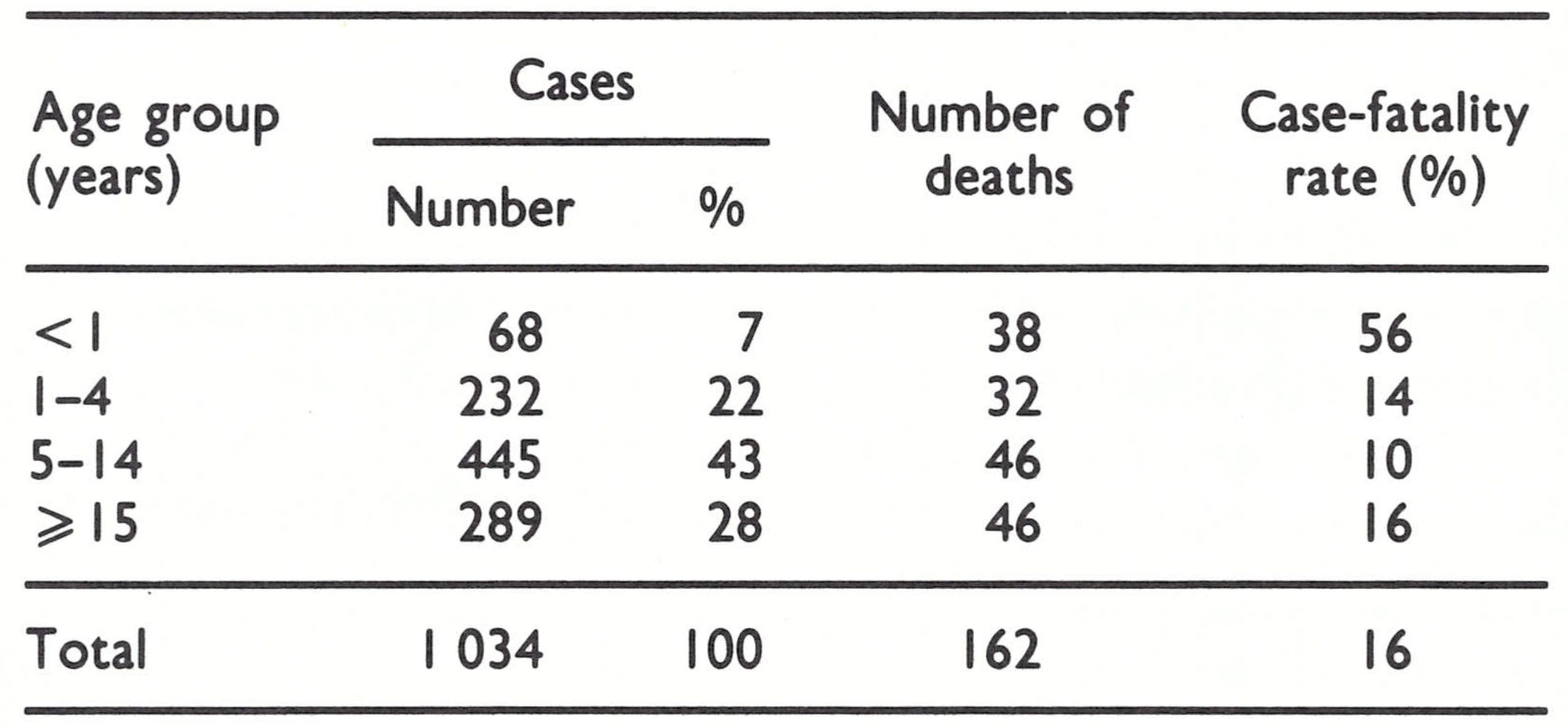
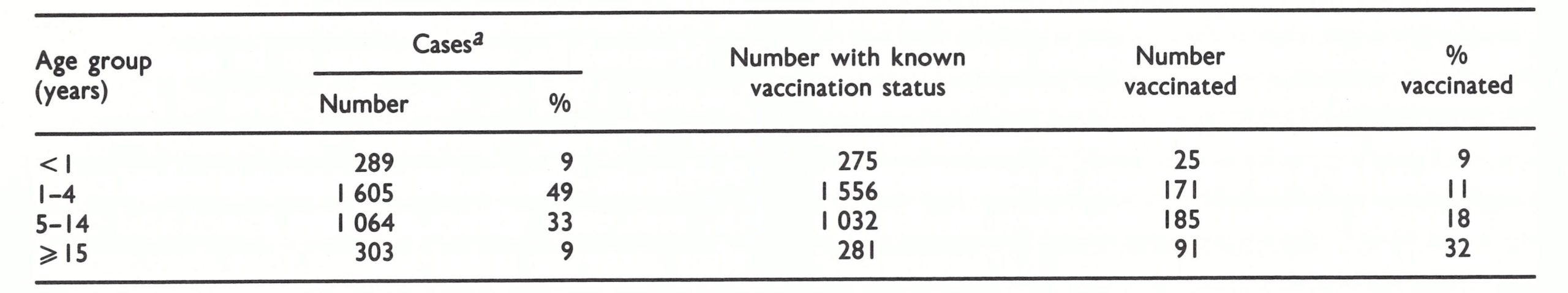
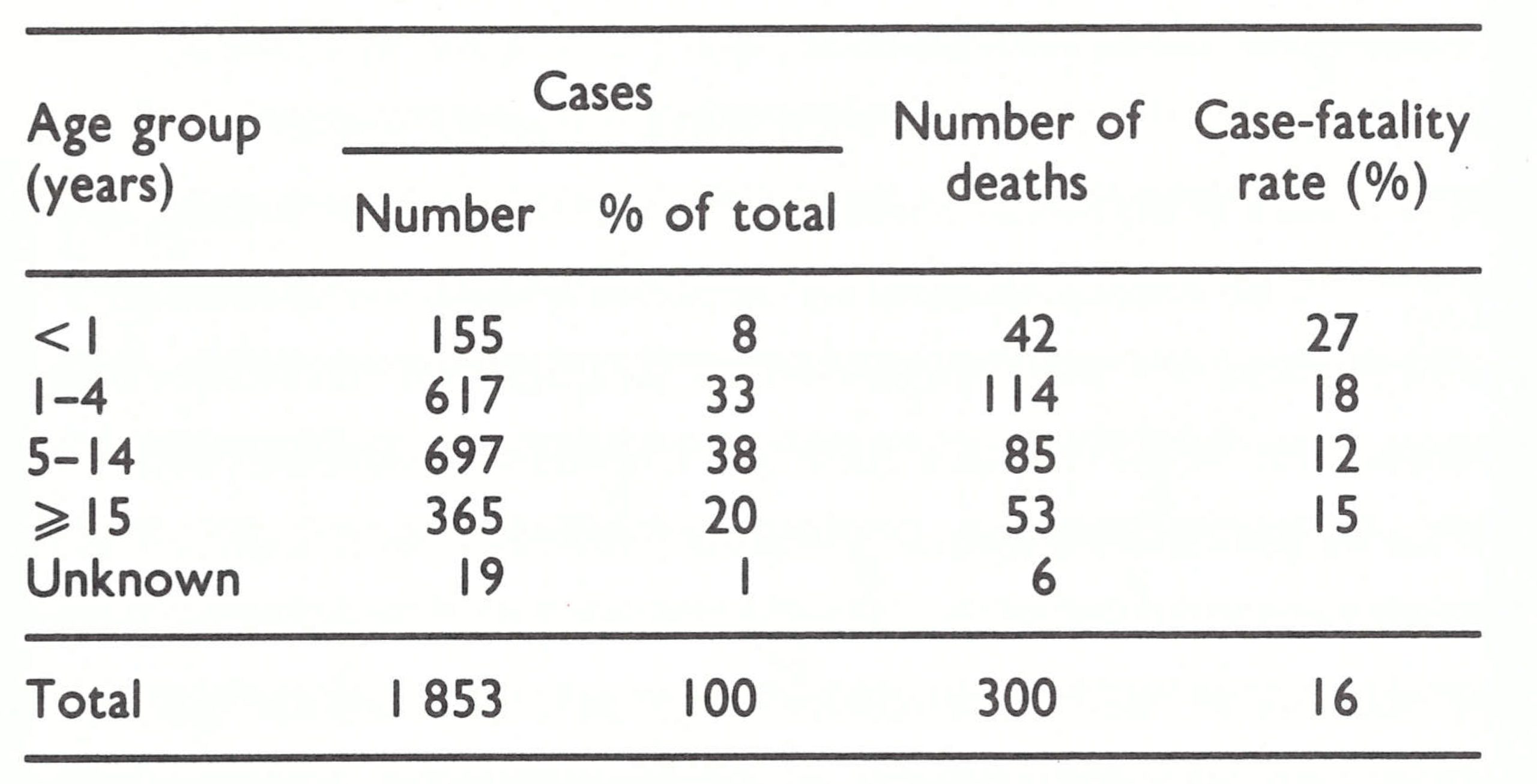
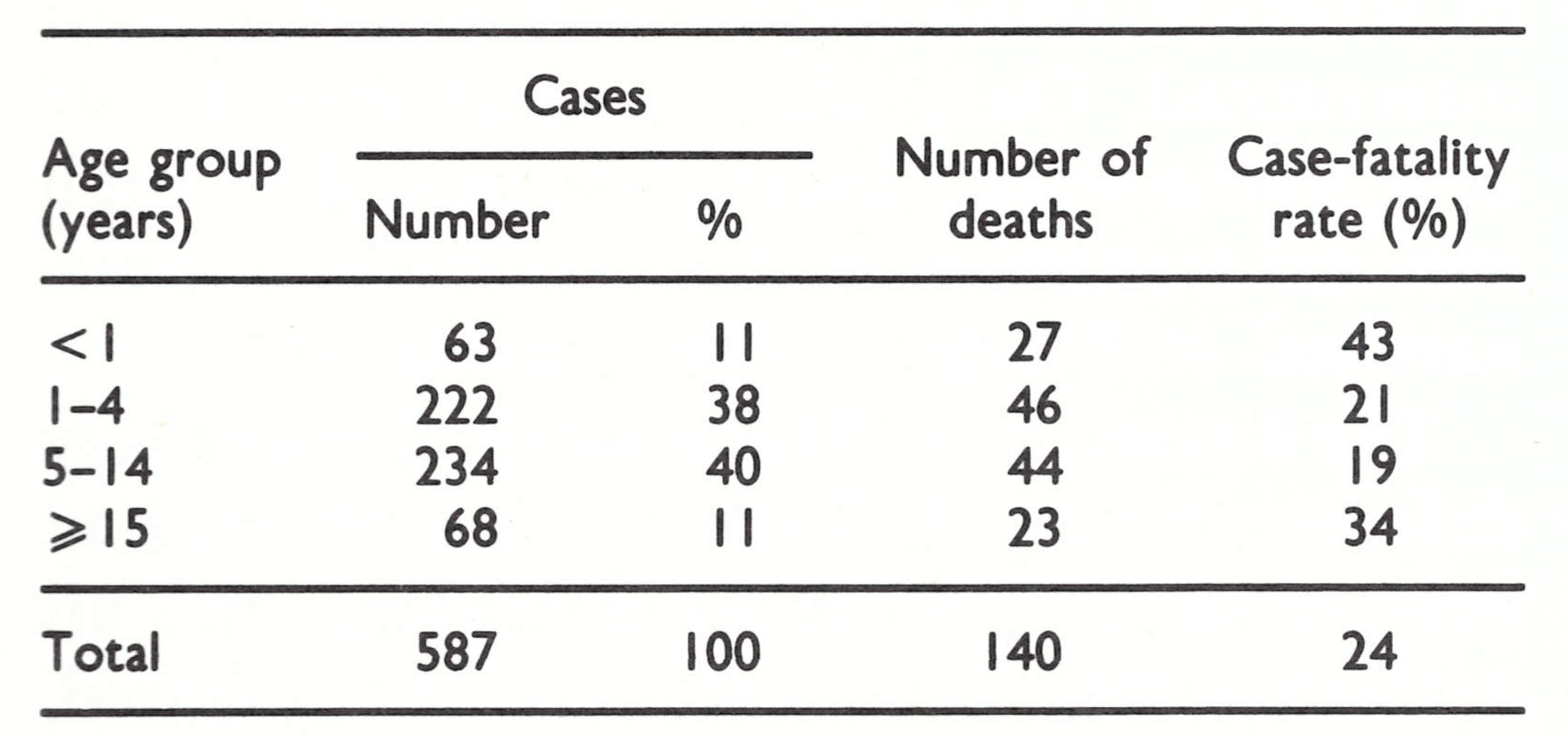
Data on age and vaccination status are available for 2258 of the 2291 cases that occurred between 1969 and 1973 (Table 14.11). Of the total, 360 cases (16%) were among persons infected through variolation. Only 83 (4%) occurred among those who had been vaccinated before exposure.
Because of the isolation of so many villages and areas in Afghanistan and the difficulty of movement from place to place, it was expected that a much larger proportion of cases would be found among adults, but in fact the proportion was not much greater than in Indonesia (11%), with its dense population, and far smaller than in Pakistan (37%). The paucity of susceptible adults reflects the extent of previous smallpox and variolation.
The overall case-fatality rate of 13.8% (313 deaths among 2258 cases) understates the severity of natural infection, including, as it does, 360 cases infected by variolation, among which the case-fatality rate was often 2-3 0,10 , Discounting variolation, the case-fatality rate was about 16%, a figure approximating to that found in the Indian subcontinent.
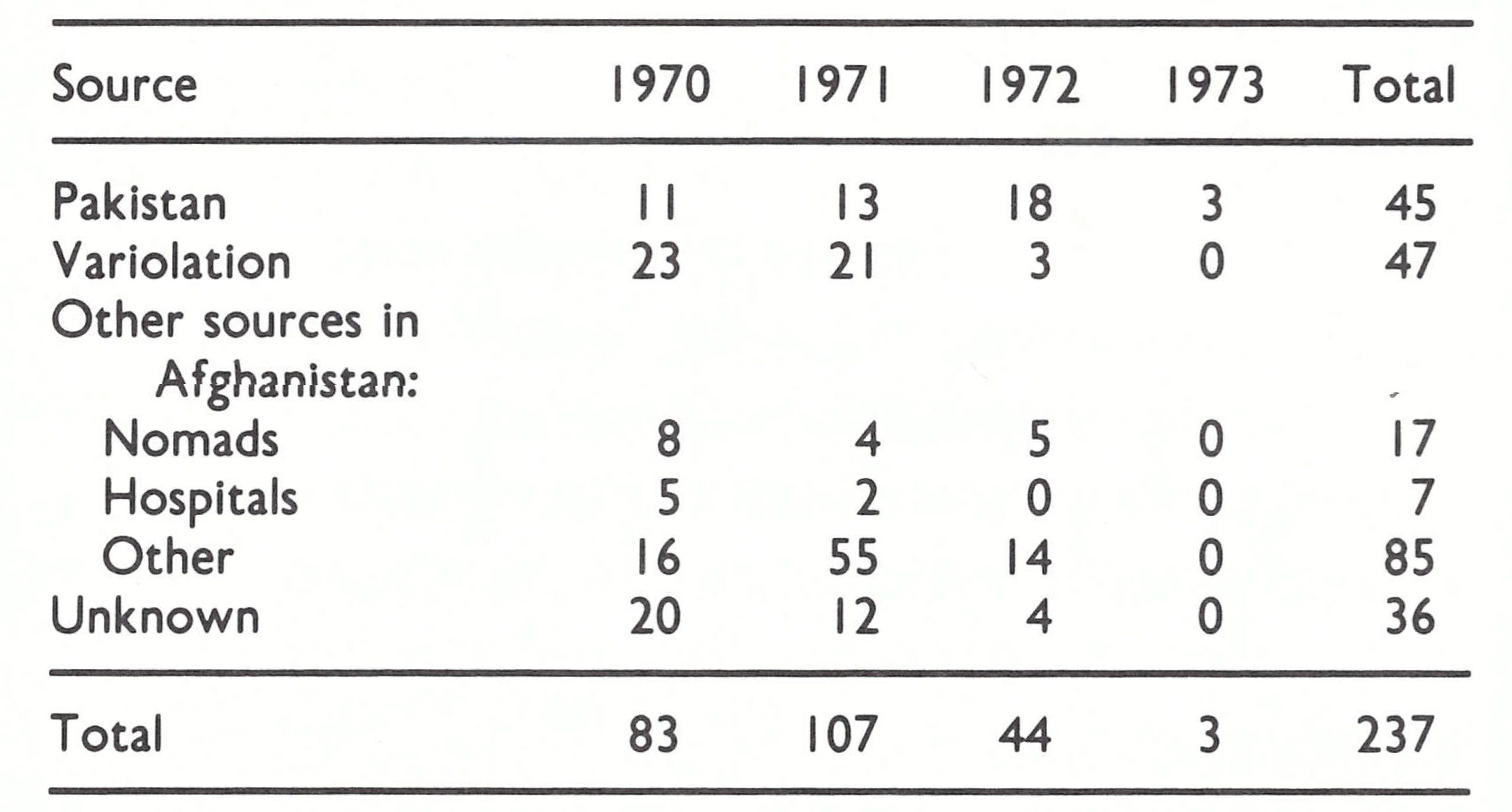
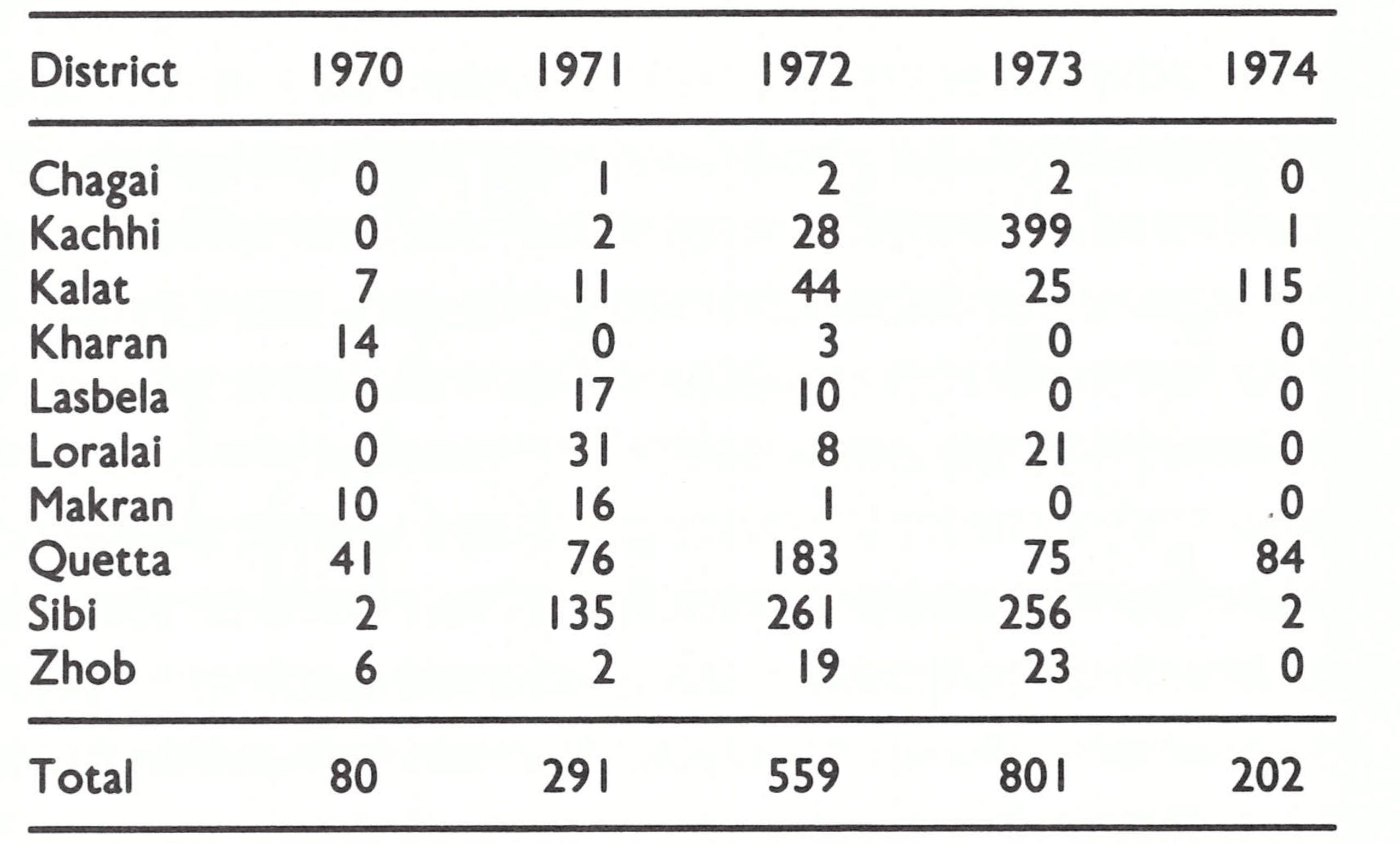
The source of infection of the 237 outbreaks that occurred from 1970 to 1973 is shown in Table 14.12. Of the 201 outbreaks for which a source could be identified, 45 (22%) represented importations from Pakistan and 47 (23%) resulted from variolation. During this 4-year period, the teams investigated a further 345 outbreaks reported to be smallpox but which, on investigation, proved to be chickenpox (202), measles (51) and other skin infections (43). The remainder were rumours without apparent foundation.
Outbreaks which resulted from importations, with one exception (in Badakshan Province), occurred in areas south of the Hindu Kush mountain range in provinces near or on the border with Pakistan. Similarly, outbreaks traced to the nomads (except those in Badghis Province) who migrated from Pakistan to Afghanistan were in these same areas (Fig. 14.7).
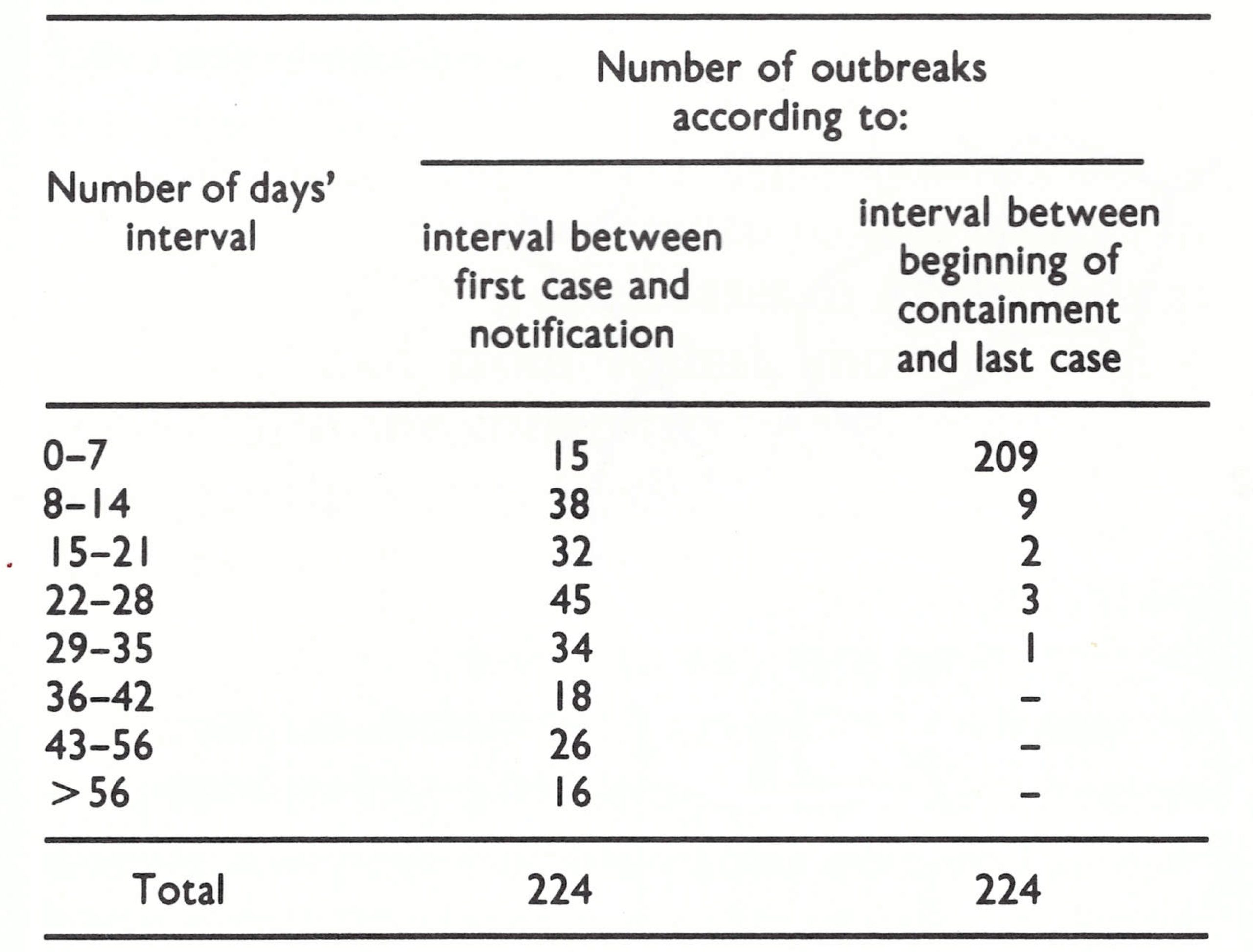
Delays in the detection of outbreaks (Table 14.13) were a problem throughout the programme. The mean interval was just under 4 weeks, the delays being as great in 1972 as they were in 1969-1970. After the outbreaks had been found, however, further transmission did not continue for long. In only 6 out of 224 outbreaks did new cases occur more than 2 weeks after containment had begun, even though many of the outbreaks were on a large scale (Table 14.14).
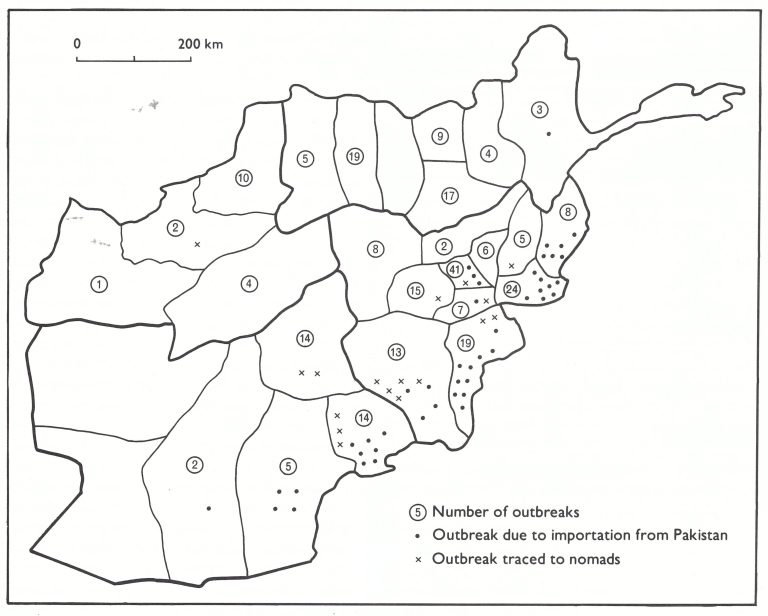
Fig. 14.7. Afghanistan: number of outbreaks by province and location of those caused by importations from Pakistan and those among nomads, 1969-1973.

Fig. 14.7. Afghanistan: number of outbreaks by province and location of those caused by importations from Pakistan and those among nomads, 1969-1973.

Plate 14.4. An Afghan worker vaccinates members of a nomad family in their tent.


Plate 14.5. A: A nomad encampment in the vast, sparsely settled central mountain plateau of the Hindu Kush, Afghanistan. B: A Pakistani woman waves the traditional neem leaves over a sick child. Throughout much of the Indian subcontinent, the leaves of the neem tree were believed to have special healing powers over smallpox.
The Problem of Variolation
Variolation had been thought to be a major, perhaps insoluble, problem. The practice was most widespread in the more remote mountainous villages and among the nomadic Kuchis, its extent being in inverse relation to the people’s ease of access to vaccination. Among the adults in some areas, upwards of 50% bore the scars of variolation. For some, variolation was the only available protection against naturally occurring smallpox and many continued to pay to have variolation performed, even when free vaccination became available. Variolation was a familiar procedure to them and they regarded it as providing permanent immunity.
Priority was given to the identification of variolators: to characterize them, learn about their practices, obtain variolation material from them and persuade them to abandon the practice or to accept vaccine for use instead of variola virus. This was difficult, however, because they feared punishment if they were discovered. Between 1969 and 1973, 61 variolators were contacted and persuaded to abandon the practice. Later, in 1976, a special search for variolators revealed 36 others. The location of the variolators by province is shown in Fig. 14.8. Undoubtedly the numbers found represent only a small fraction of the total.
The variolators performed variolation only on the request of a village or a family, and usually for a fee. Many were farmers and some were religious leaders; other practitioners who were identified included a tailor and 4 women. In almost all cases, the variolator’s father and grandfather had also been variolators and usually only the eldest son was engaged in the practice. Scabs—rarely pustular material—were collected from a recovering patient, preference being given to patients with many lesions who could therefore provide a greater amount of material. None of those interviewed said that they selectively sought to obtain scabs from less severe cases on the assumption that virus from such cases might result in less severe reactions. The scabs were usually kept either as such or in a powdered form. Sometimes, a liquid (e .g .,honey or spices in water) was added either soon after the scabs had been obtained or immediately before inoculation. Because variola virus is exceptionally stable when dried, especially if kept in a cool place, efforts were made to learn from the variolators how long they believed they could satisfactorily store the virus. Most of them stated that it was necessary to obtain new material each year. A few observed that material could be retained for as long as 2 years, but they noted that such material was not reliable and often did not induce the desired infection.
The variolators kept the scabs in all manner of jars and boxes, usually in their houses. A particularly interesting case was that of a variolator who kept the material in a horn, stored in a cave at a high altitude, quite far from his home. Although storage in a cold environment such as this should have served well to preserve the virus, the variolator reported that the material he collected was not very effective if more than a year old.
Six specimens were obtained and tested in WHO reference laboratories. Variola virus was isolated from 4 of them, of which 2 had titres that were presumably high enough to induce infection if inoculated (Table 14.15). The 4 specimens from which virus was isolated were collected between March 1969 and April 1970. One specimen collected in April 1976 consisted of scabs said to have been obtained in Pakistan in October 1974. In this specimen, virions were seen by electron microscopy but the virus did not grow on egg membrane.

Plate 14.6. A variolator demonstrates the traditional way of binding the site of inoculation after variolation. The picture was taken in Afghanistan in 1970.
Variolators were usually known to villagers throughout a subdistrict or district and were summoned only when smallpox began to occur in the area. However, some variolators travelled considerable distances, offering their services to the headman of each village visited. Sometimes, all the susceptible individuals in an entire village were systematically vaccinated, ensuring that none would remain to be exposed to natural infection acquired from those who had been variolated. This was the exception rather than the rule, however.
The usual method of variolation was to suspend the powdered scab material in a paste and to inoculate it either on the dorsum of the forearm or on the wrist, adjacent to the extensor tendon of the thumb (referred to by physicians as “the anatomical snuffbox”). Some did this by superficial linear scratch using a knife and some by multiple puncture using a small bundle of needles. A bandage was then placed over the area. Fever began on about the 4th or 5th day and a lesion appeared on the 7th day. Many of those inoculated developed lesions elsewhere on the body and, although the variolators who were interviewed usually denied that any of their patients had more than 100-200 lesions, surveillance teams found some with more extensive rashes and learned of others who had died.
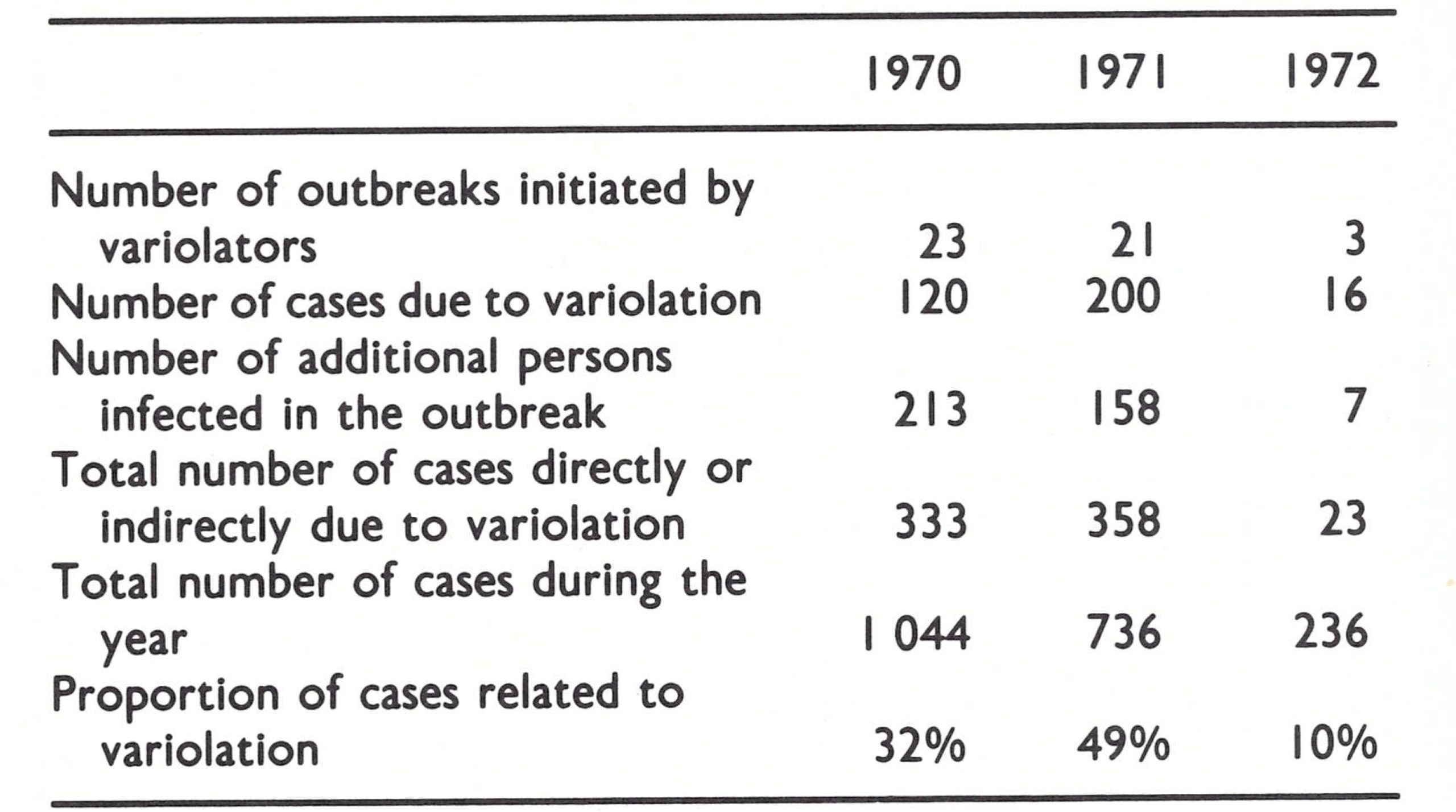
Between 1970 and 1972, 47 out of 237 outbreaks were caused by variolation. These occurred primarily in provinces lying north of the Hindu Kush range and in the central mountainous provinces of Bamian and Oruzgan (Fig. 14.8). As is shown in Table 14.16, 714 cases occurred in outbreaks which had been initiated by variolation—i.e ., more than one-third of all cases in Afghanistan during this 3-year period.
Certainly, variolation was a problem, but considering the large number of traditional variolators, it was less serious than had been expected. Because vaccination was known to most of the population—though it was not always easily available—variolation had already begun to disappear by the time the programme in Afghanistan commenced. The efforts of the surveillance teams to contact all village and subdistrict leaders and to explain to them the adverse consequences of variolation undoubtedly helped to diminish the practice. The immediate response of the surveillance teams to any reports of smallpox cases was also important: vaccination was made widely and freely available before the variolators were able to initiate their activities.
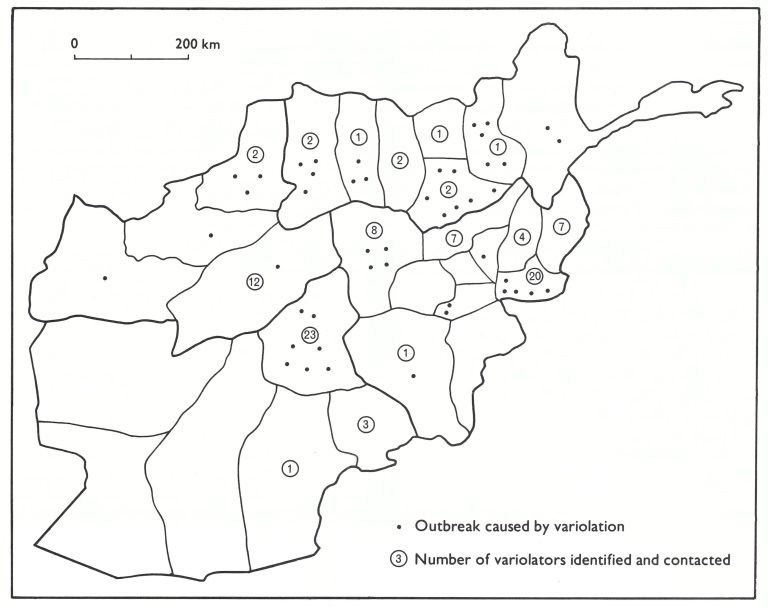
Fig. 14.8. Afghanistan: location of variolators who were identified and of outbreaks caused by variolation.
PAKISTAN
Pakistan and its smallpox eradication programme presented a contrast to the situation in Afghanistan. Most of West Pakistan’s 60.5 million people (1967) lived in the vast Indus river plain and in the Himalayan foothills, where population density was high. The government structure throughout this area was comparatively sophisticated, health services were much more extensive and health personnel were far more numerous than in Afghanistan. A network of roads, as well as train and air connections, and postal and telegraph services facilitated communication. Throughout this area, a programme of smallpox vaccination had been in operation for nearly 100 years; vaccinial immunity was high and variolation was all but unknown. Some remote, sparsely populated areas, however, presented problems almost as formidable as those in Afghanistan. In the northern mountainous areas of Gilgit and Azad Kashmir, in the mountainous districts bordering on Afghanistan and in the vast western deserts of the Baluchistan plateau, government and health services were less well developed, health personnel were few, vaccination had been less extensively practised and a few persons were still being variolated. The inhabitants of such areas, however, constituted no more than 10-15 % of the country’s total population.
In 1967, Pakistan consisted of the provinces of West Pakistan and East Pakistan, separated by the breadth of India and, each essentially autonomous so far as health programmes were concerned. In July 1970, the government decided to divide West Pakistan into 4 provinces and 2 federal regions. Health continued to be a provincial responsibility, the Federal Ministry of Health retaining authority only for health policy, the direction of medical research, standards of medical education and relationships with international organizations. A single smallpox eradication programme in West Pakistan thus became 4 separate and autonomous provincial programmes and 2 federal regional programmes which differed greatly in their methods of operation, rate of progress, and degree of political commitment to eradication. What little coordination existed between the programmes was achieved primarily by the WHO advisers. In December 1971, East Pakistan became the independent country of Bangladesh, whose programme is described in Chapter 16. The present chapter deals only with West Pakistan, designated, since 1971, as Pakistan.
Because of the availability of resources and the more sophisticated government and health structure, the eradication of smallpox appeared to be more feasible in Pakistan than in Afghanistan. Surprisingly, transmission was not interrupted until October 1974, 2 years later than in Afghanistan. Even when the last cases were being detected, the case notification procedure and surveillance system were still so inadequate that many months were to elapse before either national or WHO staff were persuaded that eradication had been achieved. Adherence to traditional mass vaccination, erratic political commitment and poor management were to characterize the programme throughout most of its course.
Smallpox before 1967
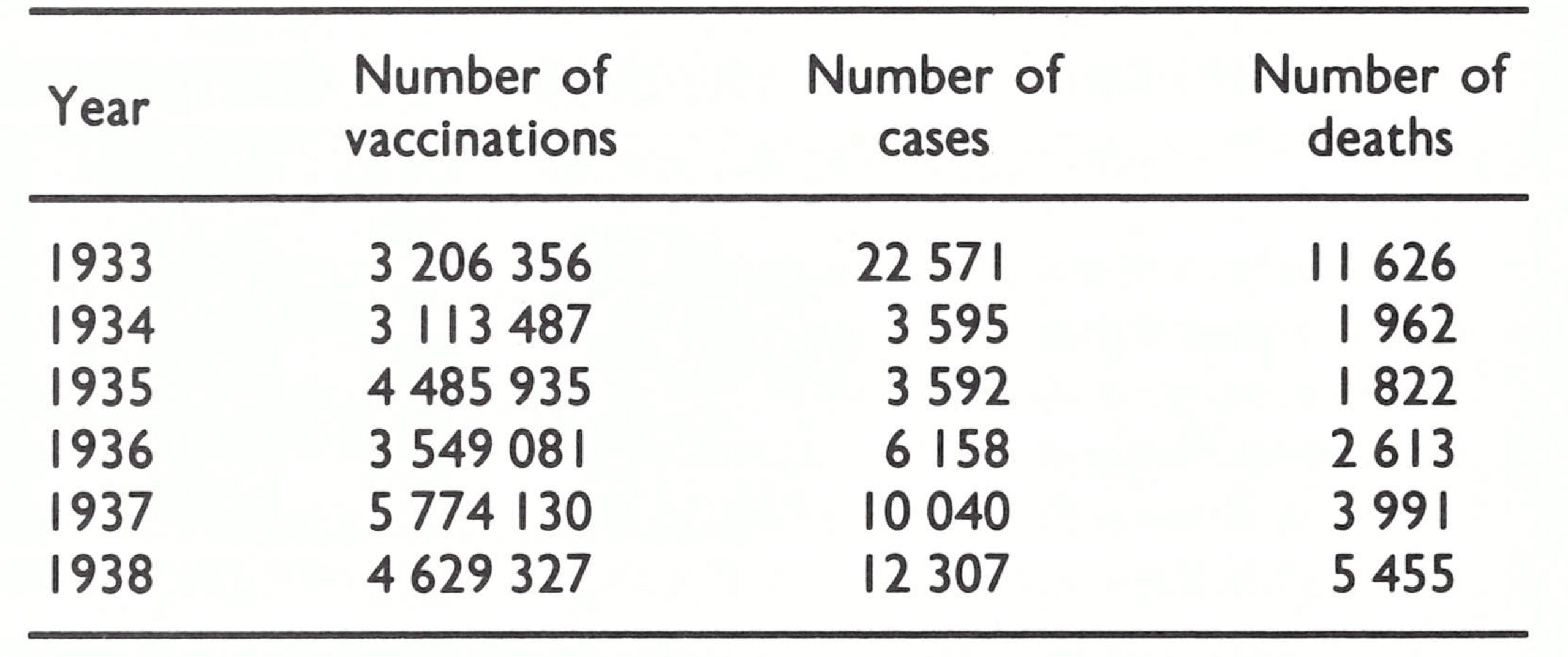
As in Afghanistan, only variola major, the severe form of smallpox, is known to have occurred in Pakistan; and in past centuries, variolation had been widely practised. Smallpox control through vaccination began during the colonial period, before British India became the independent countries of Pakistan and India, and was widely practised throughout the more populous areas until the late 19th century. In the former province of Punjab, which constitutes a major part of Pakistan, a large-scale programme of vaccination began in 1875 under a General Superintendent of Vaccination, who employed 29 supervisors and 121 vaccinators. A Vaccination Act was passed in 1880, and in 1888 local government bodies were created which were responsible for vaccination programmes in their own areas. Indeed, throughout the 1970s, vaccination by “local body vaccinators” (personnel paid by local government authorities) continued in most parts of Pakistan. Liquid vaccine produced at the Punjab Vaccine Institute in Lahore was used. The extent of vaccination is illustrated by data from the former Punjab Province for the period 1933-1938. Each year, 3.1-5.8 million vaccinations were recorded in the province, whose population was only 24.8 million (1935) (Table 14.17). Nevertheless, the number of notified cases of smallpox remained high and major epidemics recurred every 4-6 years.
Although the vaccination campaign undoubtedly had an impact on the incidence of smallpox, the effect was not impressive in comparison, for example, with that of the campaign in Indonesia, in which smallpox was eliminated during the same period . This was probably due to the fact that the vaccine used in Punjab was the thermolabile liquid product rather than the dried, heat-stable variety employed in Indonesia.
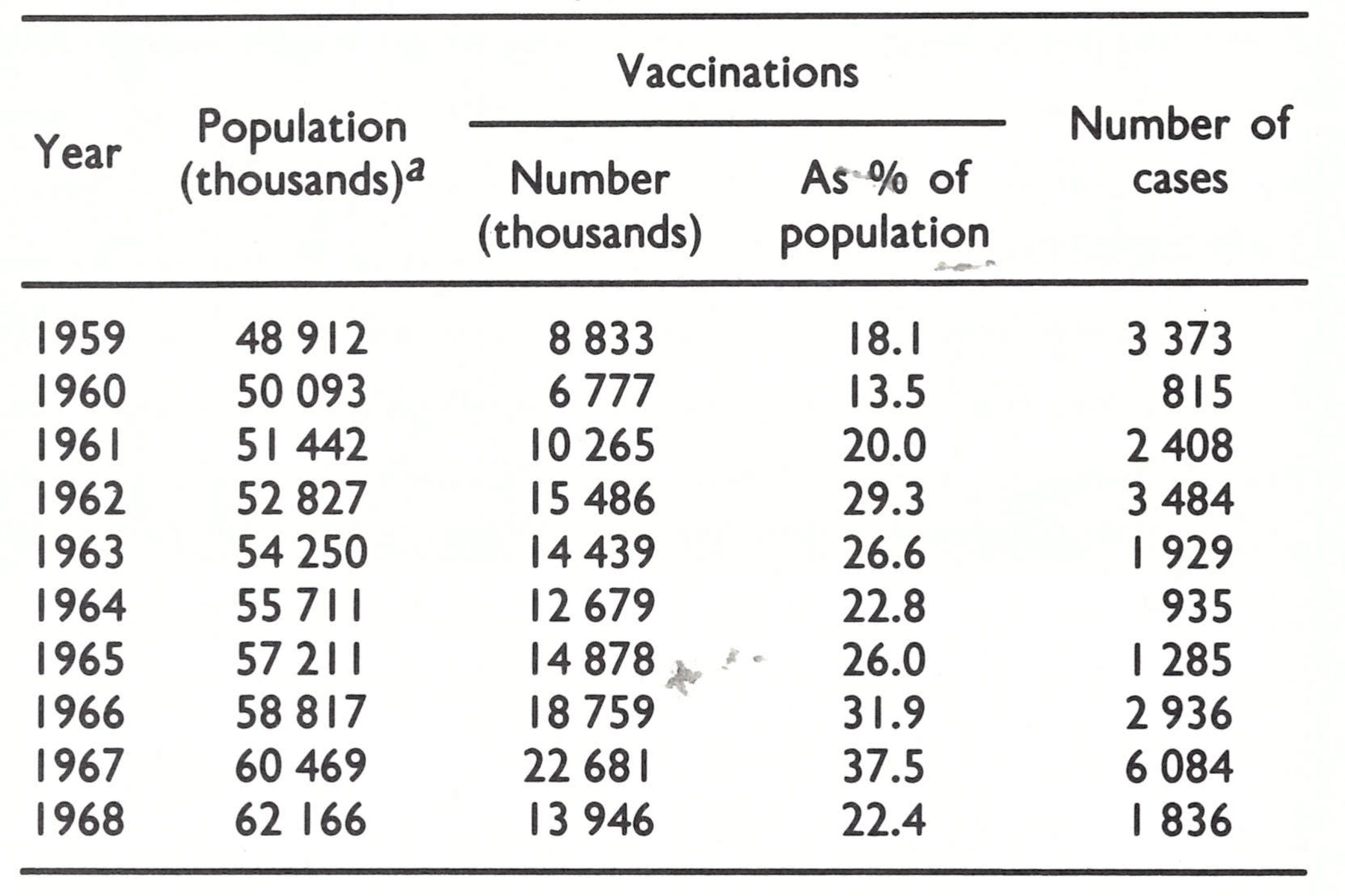
Following independence, local body vaccinators continued to vaccinate using the liquid vaccine. In the period 1959-1968 the reported number of vaccinations performed each year represented a proportion of the population ranging from 14% to 38%; moreover, the number of primary vaccinations reported to have been performed was greater than the number of newborn infants. In view of the fact that, in 1968, there was 1 vaccinator for every 40 000 persons, the numbers of reported vaccinations are believable. None the less, smallpox continued to occur, with peaks in incidence every 4-6 years (Table 14.18). As later studies were to show, the number of reported cases was only a fraction of the total that actually occurred. However, the once widely prevalent practice of variolation ceased in all but a few remote, less populous mountainous and desert areas, where it continued to exist until the end of the programme.
Programme Strategy
Immediately after the decision of the Nineteenth World Health Assembly in 1966 to intensify the smallpox eradication programme, the Director of WHO’s Regional Office for the Eastern Mediterranean, who fully supported the programme, had recruited the energetic Dr Ehsan Shafa, a veteran of Iran’s successful smallpox eradication programme of, the early 1960s, as the regional adviser on smallpox eradication. In March 1967, Dr Shafa first consulted government officials in Lahore to discuss the development of a programme. Separate schemes were drawn up for East and West Pakistan. The plan of operations was signed by WHO in August 1967 but not by the government until April 1968.
The procurement of supplies began in the hope that the programme might be launched by the end of 1968 . A WHO adviser was assigned in September 1968 and supplies were delivered that autumn. However, the programme did not commence until June 1969. Five more years were to elapse before smallpox transmission was finally interrupted. A host of administrative problems hampered the programme from its inception, and during 1971, activities everywhere were curtailed because of the civil war. However serious these problems, the principal deterrent to progress was the protracted delay in taking cognizance of the findings of a group of investigators at the Pakistan Medical Research Centre in Lahore and of the strategy worked out by them.
The Lahore centre was supported by the government of Pakistan and the United States National Institutes of Health; it was one of four international centres for medical research and training in which United States and local scientists collaborated in medical research programmes. The investigators themselves decided which studies should be undertaken; those in the Pakistani centre decided to study the epidemiology of smallpox in West Pakistan. In May 1966, they began a 1-year study of smallpox in a rural district with a population of 1.2 million near Lahore and later undertook additional studies in urban Lahore and in other districts better to define the epidemiology of the disease (Ali & Heiner, 1971; WHO/SE/69.13, Heiner et al.; Heiner et al .,1971a,b ; Mack et al .,1970, 1972a, b ; Thomas et al .,1972). The studies, which are described in the next section, were the most comprehensive to be undertaken during the whole global eradication programme. The principal investigators (Dr Ashgar Ali, Dr Nusrat Fatima, Dr Gordon Heiner, Dr Muzaffar Khan, Dr Fred McCrumb, Dr Thomas Mack and Dr David Thomas) prepared a series of important papers which were distributed to WHO smallpox eradication programme staff throughout the world beginning in 1968; most of these papers were published in scientific journals between 1969 and 1972. The data argued persuasively for giving the highest priority in Pakistan to the detection and containment of outbreaks, especially during the season of lowest incidence, and to special vaccination campaigns in urban areas. The applicability of the strategy was soon supported by observations in western Africa, Brazil, Indonesia and East Pakistan, as programmes throughout the world gave increasing emphasis to surveillance and containment. Ironically, West Pakistan was among the last to commit itself fully to this strategy.
In most countries, but especially those in the Indian subcontinent, the belief that it was necessary to vaccinate every member of the population to achieve eradication was accepted doctrine. That the development of reporting and surveillance systems was at least equivalent in importance to mass vaccination was an alien concept. In West Pakistan, the principal WHO advisers up to 1971 were veterans of the successful eradication programme in Iran in the early 1960s. There, smallpox transmission had been interrupted through a large-scale vaccination campaign; surveillance was an unknown quantity. However rational the surveillance-containment strategy might be, it was extensive vaccination to which they were committed and to which they devoted their principal energies.
Before describing the programme and its evolution in West Pakistan, it is of interest to review the findings of the group from the Pakistan Medical Research Centre, which document the status of smallpox and its epidemiology in West Pakistan at the time the programme began.

Plate 14.7. After a vaccination session, Pakistani schoolchildren hold their sleeves away from their arms to allow the remaining vaccine lymph to dry off. This was the customary practice with liquid vaccine in most countries, although vaccinations were equally successful if the excess moisture was wiped off immediately. In many countries in which mass campaigns were conducted, only a small proportion of the children attended school but they were often vaccinated at 6-month intervals by vaccinators eager to fulfil the quotas set for them.
Studies of Smallpox in West Pakistan, 1966-1967
Investigators from the Pakistan Medical Research Centre first studied the occurrence and patterns of transmission of smallpox over a 1-year period, beginning in May 1966 in a single district. Their stated objective was to determine the best strategy to interrupt transmission (Mack et al .,1970, 1972a, b ; Thomas et al.,1972). Sheikhupura District, an agrarian area of 2312 square kilometres and a population of 1.2 million, of which 85% lived in 1700 villages, was selected for study. Since 1946, the district had recorded about 50 smallpox cases per annum with occasional years during which several hundred cases were reported. During the 1-year period of study, cases were identified by the epidemiologists through the field investigation of reports to the district health officer and rumours received from civil servants and travellers and through routine inquiries in villages. Control measures, if conducted, were performed by the local health authorities.
During the year of study, 146 cases in 23 villages were officially reported to the district health officer. The investigators, however, discovered 1040 cases in 121 outbreaks and subsequently estimated, by sample survey, that an additional 40 outbreaks and approximately 180 cases had occurred that had not been detected. Thus, even in this district, which had a reasonably extensive health structure, little more than 10% of all cases were being reported. The true incidence was about 1 case per 1000 population, a figure far higher than that recorded in the most highly endemic countries during this period and an incidence substantially greater than was detected subsequently in any year in any district of West Pakistan.
Data regarding the age and outcome of illness were reported for 1034 of the patients The age distribution and case-fatality rates were similar to those observed elsewhere in the Indian subcontinent: 29% of cases occurred among children under 5 years of age and a similar percentage (28%) among persons aged over 15 years (Table 14.19). In all, 16% died, but among infants (under 1 year) case-fatality rates reached more than 50%.
Despite the substantial number of cases, sample surveys of 15 villages showed a remarkably high proportion of persons who had previously been vaccinated. Among 6000 persons examined, 88% had either vaccination scars or the pockmarks of smallpox (Thomas et al .,1972). Three-quarters of the cases had occurred among the 12% who had not been vaccinated before exposure (Table 14.20). Among the unvaccinated household contacts of cases, 88% developed smallpox, compared with only 7% of people who had been vaccinated at some time.
Studies of smallpox transmission in 6 rural districts showed that vaccinated persons who experienced infection transmitted the disease to others only one-fourth as often as did unvaccinated persons with smallpox (Heiner et al., 1971b; see Chapter 4, Table 4.10).
In brief, smallpox transmission was sustained primarily by perhaps 150 000 persons of Sheikhupura District’s 1.2 million residents. Pakistan’s vaccination campaign had been more effective, at least in this district, than had been thought. A later study, done in Lahore Municipal Corporation, showed even higher levels of protection . In Lahore, 93 % of all persons surveyed showed vaccination scars or the pockmarks of smallpox. Even among infants under 1 year of age 39% were protected, and among children aged 1-4 years 84% were protected (WHO/SE/69.13, Heiner et al.; Ali & Heiner, 1971).
The seasonal fluctuation in incidence was significant (Fig. 14.9), the peak occurring during the colder, drier months of November to the end of March. By September, at the end of the hot summer monsoon, smallpox had all but vanished (Thomas et al., 1972); in the first week of September 1966, only 1 village in the entire district was infected. However, even at the peak of the transmission season, not more than 50 of the 1700 villages in the district were infected at one time.
The outbreaks were often small and most terminated spontaneously. Smallpox was found to spread far less readily than measles or influenza, for example . Nearly one-third of the outbreaks consisted of single cases and in only half of the 121 outbreaks did new cases develop more than 4 weeks after the first case had occurred (Thomas et al., 1972). Even when transmission did occur, an average of only 2.4 new cases was recorded during each 2-week period. The larger outbreaks were of greater epidemiological importance . More than 50% of outbreaks with 5 cases or more were identified as sources of other outbreaks, compared with only 15% of outbreaks with fewer than 5 cases.
Contrary to what many supposed, smallpox was rarely transmitted at large public gatherings or transferred from place to place by nomads. Most infections were acquired as a result of contact with the patient in his own home (Thomas et al., 1972).
A further significant observation was the identification of large urban areas as important foci for spread Of 74 outbreaks for which a specific source of infection could be determined, 42 (57 %) could be traced directly or indirectly to cities, in which only 19% of the Punjabi population resided (Thomas et al .,1972).
The group of investigators pointed out that if Sheikhupura District and the Lahore Municipal Corporation were representative of other areas with regard to vaccinial immunity levels, a mass vaccination campaign had, to all intents and purposes, already been carried out. They recommended that instead of conducting another mass campaign, attention should be focused on the detection of cases and the containment of outbreaks, especially in urban areas. Such an approach would be especially effective during the summer, when only a few localities were infected. Because the disease spread slowly within and between villages, they believed that few resources would be required to cope with the outbreaks. Even if the reporting of cases was not improved, the effective containment of those that did come to notice should have a significant impact, since, as had been found, the larger outbreaks were reported more often and were most frequently responsible for spread to other localities. Because of the importance of cities in transmission, it was reasoned that urban areas should be given priority in mass vaccination campaigns, if such were to be conducted, and that emphasis should be placed on primary vaccination.
The observations in Sheikhupura District were subsequently found to be applicable throughout most of Pakistan. Not all areas had as high levels of vaccinial immunity as Sheikhupura, but everywhere successful immunization had been far more extensive than anyone had believed and the epidemiological pattern of spread of smallpox was similar. The recommendations of the group of investigators proved to be sound when they were eventually put into practice in Pakistan in 1972.
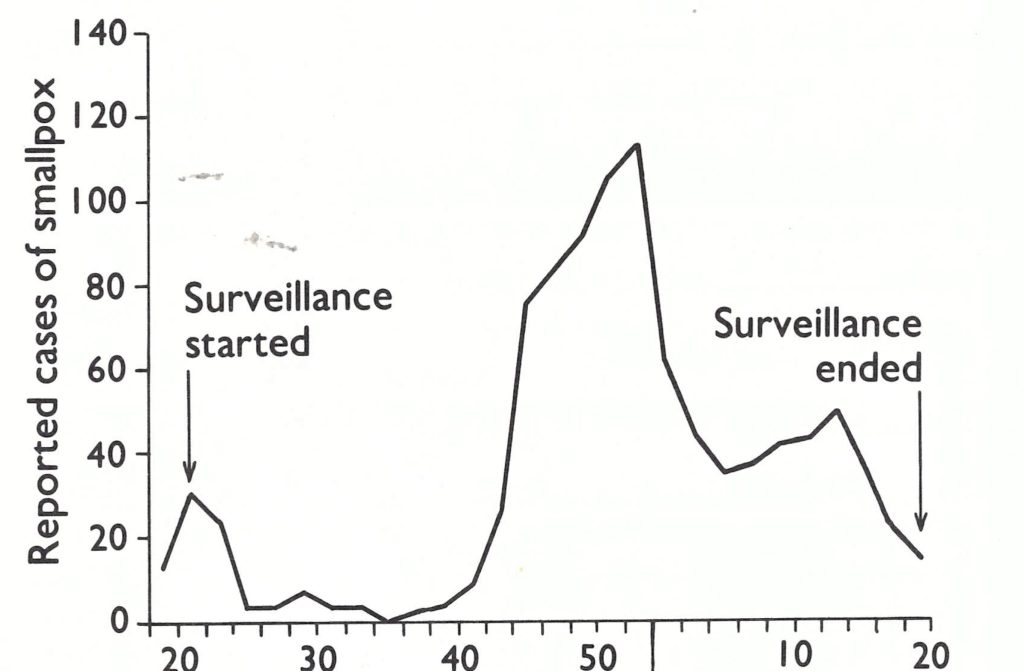
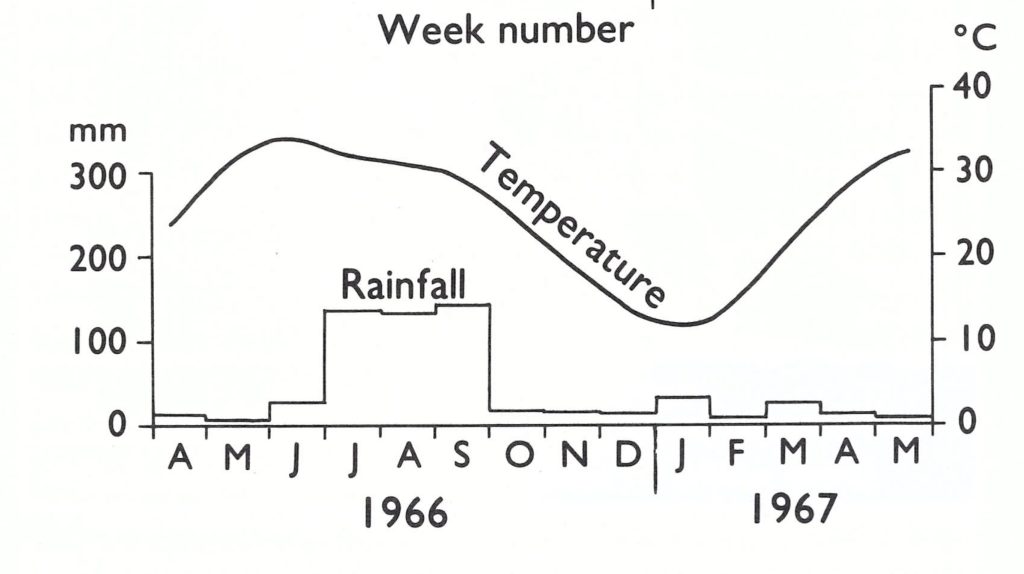
Fig. 14.9. Pakistan, Sheikhupura District: number of reported cases of smallpox in relation to meteorological data, by 2-week intervals, 1966-1967.
Beginning of the Mass Vaccination Campaign, 1968-1969
The plan of operations was signed in August 1967 by WHO and in April 1968 by the government, in Islamabad . Planning, procurement of supplies and recruitment of staff took longer than expected, but in June 1969 field operations finally began. West Pakistan, in 1969, was divided into 6 health regions, each comprising about 8 districts. Each district had a population of 1-2 million. The plan called for systematic mass vaccination campaigns in 2 regions each year. When the mass vaccination campaign was completed in a region, maintenance vaccination would be introduced to vaccinate neonates and migrants and to revaccinate the entire population every 3-4 years (Table 14.21).
The inhabitants of the two most populous health regions of Sargodha and Lahore, in which Sheikhupura District was located (Fig. 14.10), would be the first to be vaccinated. The campaign was to be directed by 2 provincial medical officers assisted by the WHO adviser and, at each health region office, by 2 medical officers, plus supporting clerical staff. At the health region level, a unit composed of 10 vaccinators and a superintendent of vaccination were to undertake surveillance activities and to control epidemics. The primary operational unit was the district, in which the campaign was to be directed by a full-time medical officer, a district superintendent of vaccination and teams of 10 vaccinators. A complement of 50 vaccinators for every million persons was considered necessary. This number was determined on the assumption that each vaccinator would perform an average of 100 vaccinations a day over 200 working days each year. Each operational group of 50 vaccinators would have a group leader and 5 assessors to check performance; vaccination was to be conducted village by village and house by house, the inhabitants of each locality to be vaccinated systematically by an operational unit of 10 vaccinators. The units would continue work in a locality until a number equivalent to 85-90% of the estimated population had been vaccinated. As in Afghanistan, the plans called for the teams to spend 24 consecutive days in the field, followed by 7 days’ leave. A 10% sample of the vaccinations performed was to be assessed 1 week after vaccination. In addition to the surveillance-containment unit at regional level, a 10-man surveillance and containment unit was to be established in each district. The projected manpower required and the number available as at December 1968 are shown in Table 14.22.
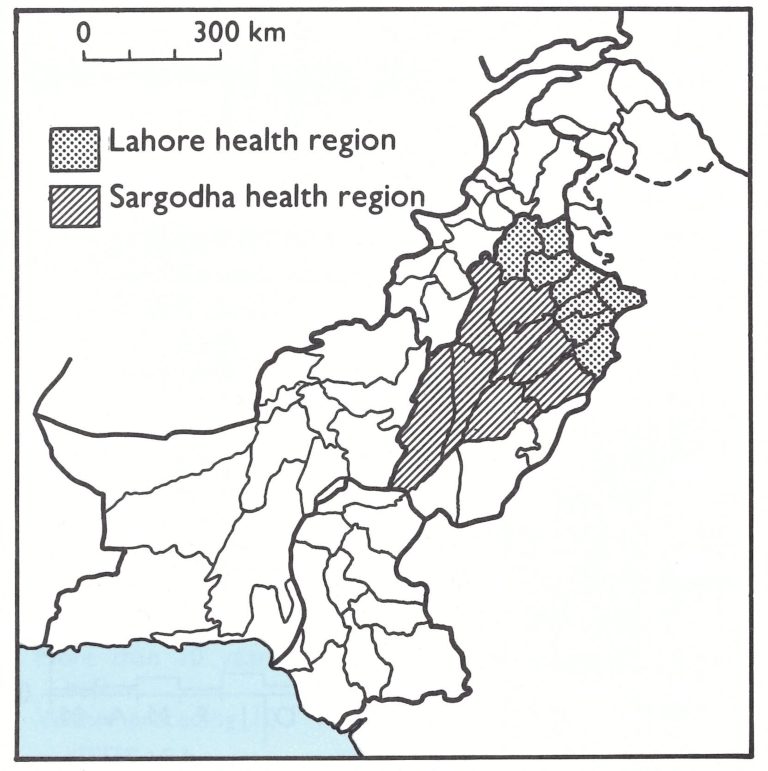
Fig. 14.10. Pakistan: districts to be vaccinated, 1968-1969.
WHO agreed to provide US$200 000 in support of the programme, for the purchase of 25 Land Rovers, 125 motor cycles, 1300 bicycles, 25 refrigerators, a stock of bifurcated needles, and miscellaneous supplies. (Eventually WHO provided approximately US$1.3 million to the programme, as well as 70 million doses of vaccine (Table 14.23).) Freeze-dried vaccine produced at the Institute of Public Health, in Dhaka, East Pakistan, was to be used. It was calculated that the government of West Pakistan would need to increase its budget for smallpox eradication from 1 334 650 rupees to 2 728 480 rupees (US$278 800-570 000) for each of the 3 years of the Intensified Programme. It was expected that the previous level of financing would be adequate to cover the maintenance phase.
The findings and recommendations of the research group from Lahore did not become available until shortly after this plan was drawn up in August 1967. Even so, sufficient ments for the smallpox eradication resources were foreseen in the plan to permit programme, 1969 surveillance and containment activities of the type recommended.
By December 1968 major problems had become apparent. The government did not increase the budget but, in fact, decreased it by 30%—to 1 million rupees. The plan envisaged the use of local body vaccinators as part of the complement of personnel but they were responsible to their own union councils (administrative units each responsible for a population of about 10 000) and the councils, in turn, to the Ministry of Basic Democracy. As the WHO adviser was to report: “A number of vaccinators have been appointed under political pressure and many of them are recommended by influential persons and are engaged in other duties or private jobs.” Likewise, vaccinators in the municipal areas were under an entirely different jurisdiction, and there was no coordination of their activities with those of the provincial or regional staff. The problems of programme direction were further complicated when supervisory staff indicated that they could not travel to the field because the government’s travel allowance was too meagre to cover the cost of even the most austere board and lodging. Last but not least of the difficulties was that no provision had been made for the purchase from programme funds of freezedried vaccine from the government’s quasiindependent Dhaka laboratory. Up to this time, liquid vaccine had been purchased by union councils with their own funds and no administrative mechanism existed to permit these funds to be diverted to the purchase of freeze-dried vaccine.
One by one, the problems were solved or partially solved by a variety of means . Because vaccine production at the Dhaka laboratory was found to be inadequate to supply more than East Pakistan, WHO provided freezedried vaccine which had been contributed by various donors, primarily the USSR. WHO agreed to provide funds to supplement the travel allowance of national supervisory staff to permit them to travel to the field. The Ministry of Basic Democracy was, with difficulty, persuaded to issue an order to the union councils directing local body vaccinators to work with the programme, an order which was subsequently ignored as often as it was respected. Eventually, the national government authorized additional funds to recruit the requisite staff.
The programme in the 16 districts began in June 1969, but outside these districts no effort was made to develop reporting or surveillance activities. Even in the 16 districts, the socalled “fire-fighting” and surveillance teams did little. Indeed, in Lahore, one of the principal urban centres, a surveillance programme was not established until May 1972.
In all, some 1600 government staff participated in the unnecessary mass vaccination campaign in the 2 regions. The campaign was completed at the end of May 1970. One million primary vaccinations and 22 million revaccinations were recorded in a population of 27 million persons. Between March and May, 313 000 persons in 546 localities were examined to determine the level of vaccinial immunity achieved. The survey revealed that only 3.7% of them had neither a vaccination scar nor the pockmarks of smallpox. Even making allowance for possible errors in the assessment, it was apparent that the residual number of susceptible individuals was small but, as the research group from Lahore had shown, the number of unprotected persons had not been large when the vaccination campaign began. The marginal improvement was confirmed by a study in a division in which the health services were the least adequate: before the campaign, 10.5% of the population were found to be unprotected; after its completion, 8% remained unprotected.
Table 14.23: Pakistan : WHO support provided to the smallpox eradication programme, 1967-1978 (US$)
a Excluding supplies of vaccine (about 70 million doses).
b WHO records reflect support given to both West Pakistan and East Pakistan (which became the independent state of Bangladesh In December 1971). Approximately half of the total was provided to West Pakistan and these are the figures shown in the table.
One Programme Becomes Six, July 1970
On 1 July 1970, the administrative divisions of West Pakistan were abruptly changed by the government as part of the x 400- efforts to cope with increasing tensions in the oa relationships between East and West Paki- E stan. As has been mentioned above, the o 300- province of West Pakistan was divided into 4 independent provinces and 2 small, federally administered regions in the north of the v 200- country (Azad Kashmir and Gilgit) (Fig. 14.11). The populations of the provinces differed greatly in size: Punjab, 32.1 million; 93C Sind, 11.9 million; North-west Frontier 1 Province, 9.5 million; and Baluchistan, 1.61 million. The 16 districts in which the mass vaccination campaign had been conducted were all in Punjab Province, along with 3 additional districts. Early in the autumn of 1970, mass vaccination was completed in these 3 districts, during which an additional 200 000 primary vaccinations and 2.4 million revaccinations were reported to have been given. However, as shown in Fig. 14.12 and Table 14.24, the total of 25.6 million vaccinations performed in Punjab Province had little impact on the reported incidence of smallpox.
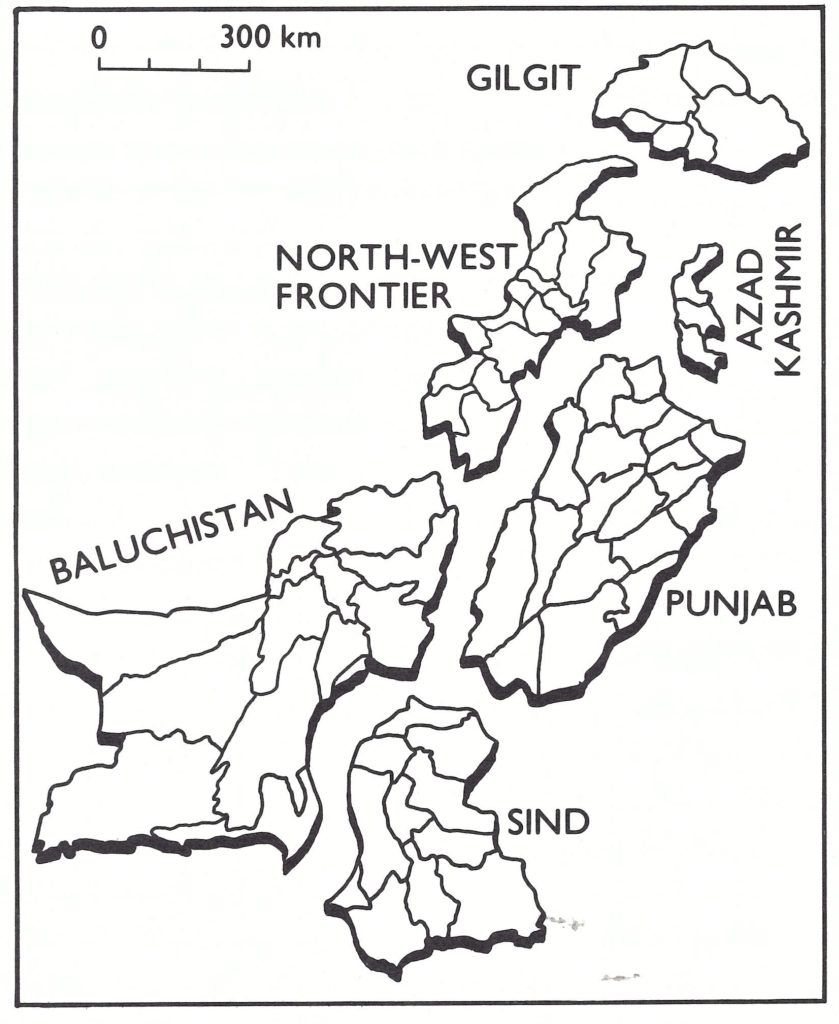
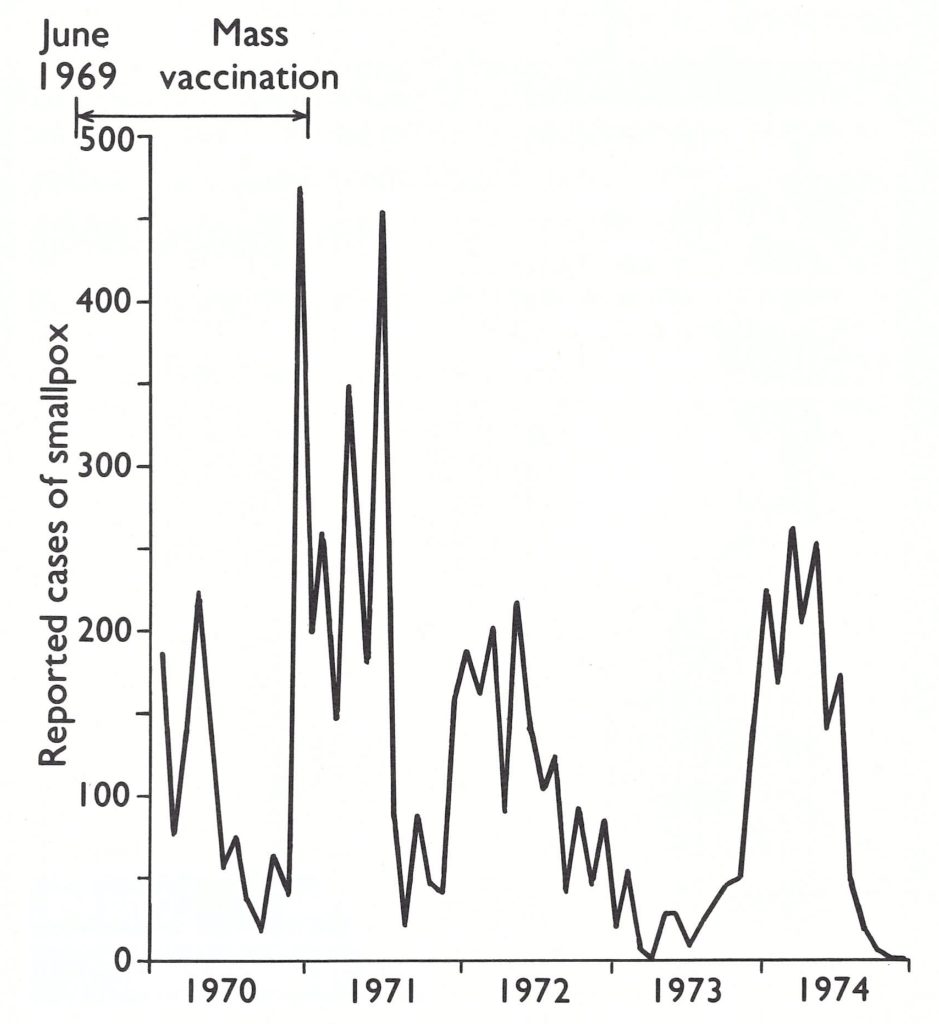
Fig. 14.11. Pakistan : provinces (or federally administered
areas) and districts in July 1970.
Fig. 14.12. Pakistan,Punjab Province: number of reported cases of smallpox, by month, 1970-1974.
The failure of the campaign to have any apparent effect on the reported number of cases might be thought to reflect a better notification of cases, which masked the effect of the vaccination campaign. In fact, however, the surveillance teams functioned poorly and the notification system was not improved during this period.
Because of the subdivision of West Pakistan into 4 separate provinces and because each of the provinces was granted almost total autonomy in health matters, new provincial governments had to be persuaded of the need to undertake a smallpox eradication programme, to create some sort of organizational structure, to establish a budget and to recruit and/or assign personnel. In 3 of the provinces, no smallpox eradication activities had yet been undertaken. The national government and the national programme director had responsibility for the signing of agreements with WHO to permit advisers to be assigned and equipment to be provided, but had no authority over field activities except in the remote and sparsely populated Azad Kashmir and Gilgit.
The constraints on federal authority are illustrated by the frustration experienced in endeavouring to establish a vaccine production facility in the newly constructed national laboratories in the capital, Islamabad. In 1970 WHO offered to provide equipment for vaccine production and consultant assistance to establish a facility, which, it was hoped, would produce vaccine for the whole of West Pakistan. The federal government insisted that this could be done only if the government of Punjab transferred funds to the federal government that had previously been used to finance the now defunct liquid vaccine production unit at Lahore. After prolonged negotiation, agreement was reached and WHO ordered and delivered the production equipment. Because of Punjab’s later refusal to honour the agreement, the equipment was never used. Vaccine for the programme continued to be provided by WHO, initially from various donors but after 1973, from the Pasteur Institute in Iran, which donated large amounts of vaccine to WHO.
In an effort to establish a programme encompassing the entire country, an interprovincial meeting was convened in December 1970 to seek the agreement of all provinces to undertake programmes. Two years had elapsed since the projected commencement of the programme in West Pakistan, but little had been achieved, except for mass vaccination in 19 districts. Meanwhile, the incidence of smallpox had remained virtually unchanged (Fig. 14.13). The lack of accomplishment after the expenditure of effort in districts with the most developed government and health structures and the greatest resources offered little encouragement for success at a national level.
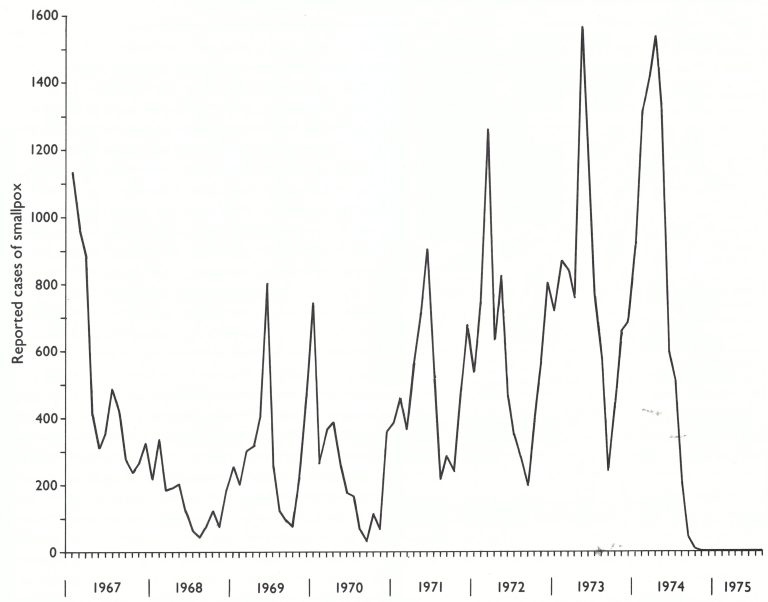
Fig. 14.13. Pakistan: number of reported cases of smallpox, by month, 1967-1974.
The Fourth Year of the Programme, 1971
At the meeting in December 1970, representatives of each of the provinces of West Pakistan agreed to give high priority to smallpox eradication: to create the necessary administrative structure, to develop a reporting and surveillance system and to seek the necessary funds for a systematic mass vaccination campaign. WHO agreed to recruit 3 additional advisers so that one could be assigned to each province, the senior adviser continuing in his capacity as national counterpart as well as adviser to the programme in Punjab. Additional supplies and equipment were ordered by WHO and travel allowances were provided for senior supervisors in all provinces. Meanwhile, because title to the vehicles and other equipment provided by WHO remained with the Organization, some supplies from Punjab Province were transferred to other provinces, an otherwise impossible action in the case of governmentowned supplies.
It was agreed that interprovincial meetings would be held twice a year to coordinate the 4 separate programmes. However, each programme developed more or less independently, employing different strategies and achieving varying degrees of success. All of them encountered difficult obstacles, in the first instance because of the diversion of resources due to the civil war in East Pakistan, and then as a result of the tension between India and Pakistan at that time. In December 1971, when East Pakistan became the independent state of Bangladesh, these difficulties abated and additional resources were made available to all programmes. Three additional WHO advisers were recruited, arriving between March and June 1971. They were assigned, respectively, to Sind, North-west Frontier Province and Baluchistan. However, little was done during that year in Baluchistan, or in Sind except in the city of Karachi.
In 1971, Punjab Province appeared to be the best candidate to achieve the early interruption of transmission. Because 60% of the population of West Pakistan lived in that province, it was believed that the interruption of transmission there would provide an impetus to the other provinces. A programme had been in operation for 3 years, the mass vaccination campaign had been completed, and few susceptible persons remained. The reporting system had improved little since 1968, but with the vaccination campaign finished, smallpox staff found themselves with few responsibilities other than to develop a surveillance-containment programme. In May, 8 assistant superintendents of vaccination and 19 vaccinators were trained in surveillance activities and began working in 2 teams under the direction of the Provincial Smallpox Eradication Officer, Dr M. B. Khawaja, who was succeeded by Dr Mohammed Rafique. In the summer of 1971, all district health offices were ordered to send weekly telegrams to report the number of cases discovered during the week. With 1407 health units (172 hospitals, 893 dispensaries, 39 rural health centres and 303 maternal and child health centres) in which cases might be identified, it was reasonable to expect that the reporting of outbreaks would be quite complete if a system could be developed.
Because there were only 2 large teams engaged in search and containment in a province of 32 million people, and because telegraphic reports were then being received from less than half of the districts despite the provincial order, many outbreaks continued to be overlooked. More important, little was done in urban areas-the chief foci for the dissemination of smallpox. Programmes in the urban areas were the responsibility of the municipal corporations, each of which had its own health structure, and these, independent of provincial policies and supervision, continued to carry out traditional routine vaccination campaigns.
During 1971, the Punjab surveillance teams investigated 81 outbreaks, in which 561 cases had been reported ; an additional 1475 cases were discovered. Although the total of 2036 cases was the same as that recorded in 1969, when the vaccination campaign began, the number of cases declined sharply in the latter half of the year, only 20-90 being reported monthly between July and November.
Meanwhile, in North-west Frontier Province, an energetic WHO adviser, Dr G. P . Marchenko, arrived in March 1971. With the help of an able provincial medical officer, Dr Mohammed Ayaz Khan, the province launched a mass vaccination campaign in May in 4 of its most populous districts-Peshawar (the capital), Mardan, Hazara and Swat. In contrast to Punjab, case detection was specifically emphasized as an important component of activity. Numerous cases were discovered by the vaccination teams (Table 14.25 ; Fig. 14.14). By the end of the year, 2654 cases had been detected, most of which (2132) were in the 4 districts in which the campaign was being conducted. This was 5 times the number recorded during the preceding year. The “epidemic” alarmed provincial authorities but stimulated political interest and support, which continued throughout the rest of the programme.
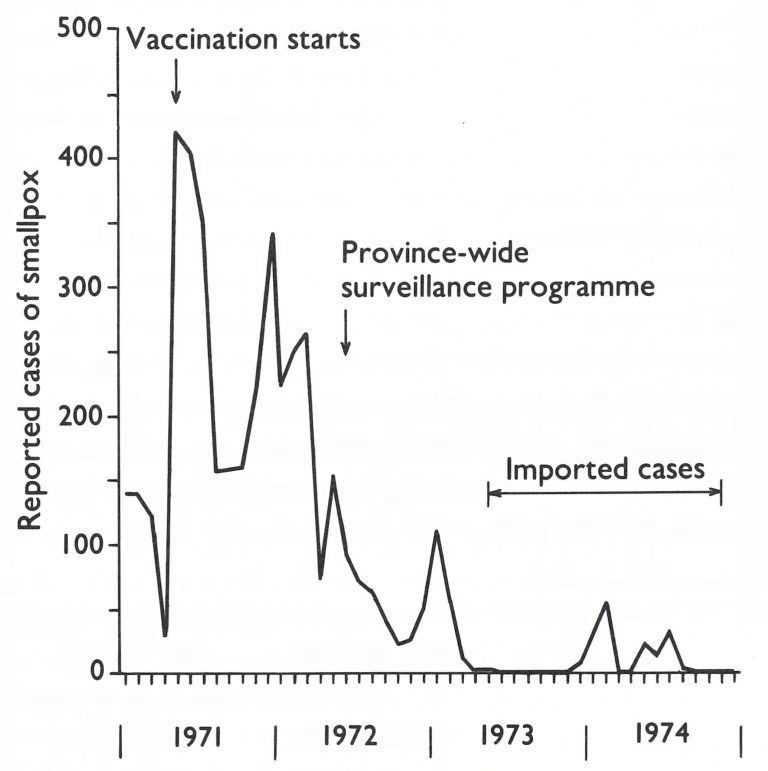
Fig. 14.14. Pakistan: North-west frontier Province: number of reported cases of smallpox, by month, 1971-1974.
Commencement of Country-wide Activities, 1972
During 1972, smallpox eradication programmes were introduced in Sind and Baluchistan Provinces and activities at last extended throughout most of the country. The provincial programmes progressed at different speeds and encountered such different problems that each is described separately. The remarkably successful programme in North-west Frontier Province is dealt with first. Transmission was interrupted only 2 years after the programme had begun, but the area was inundated by importations from the other 3 provinces for more than a year thereafter. Next to be discussed is the programme in Punjab, with its large population and attendant operational problems, and then the inadequately supported and poorly organized programmes in Sind and the sparsely populated Baluchistan. Table 14.26 shows the number of reported cases by year for each of the provinces during the period 1970- 1975.
North-west Frontier Province
North-west Frontier Province extends from the foothills and mountains of the Himalayas along the border with Afghanistan to the plains of the Indus river in the east and south-east (Fig. 14.15). About three-quarters of the population are traditionally independent Pathans, some of whom at that time enjoyed semi-autonomy in federally administered tribal areas in the mountainous districts of Waziristan, Khyber, Kurram, Malakand and Mohmand. Extensive vaccination campaigns had been conducted during the preceding years throughout the plains and foothills, as in Punjab, but in some sparsely settled mountainous and tribal areas variolation continued to be practised.
The house-to-house vaccination campaign, which began in May 1971 in 4 districts, was completed in June 1972 A staff of 350 persons vaccinated 3.6 million people (about 80% of the 4.4 million inhabitants of the area). Initially, the search for cases and the containment of outbreaks were limited to these 4 districts. In July 1972, vaccination campaigns were initiated in the districts lying in the Indus river plain (Kohat, Bannu and Dera Ismail Khan) and efforts were made to launch campaigns in the tribal agency districts . The latter were soon abandoned, however, when it was discovered that frequently only 5% or less of the population would accept vaccination. Data on the efficacy of the vaccination campaign are available from surveys conducted in 1973 in 5 districts. The results were, in general, comparable to those in Punjab (Table 14.27).
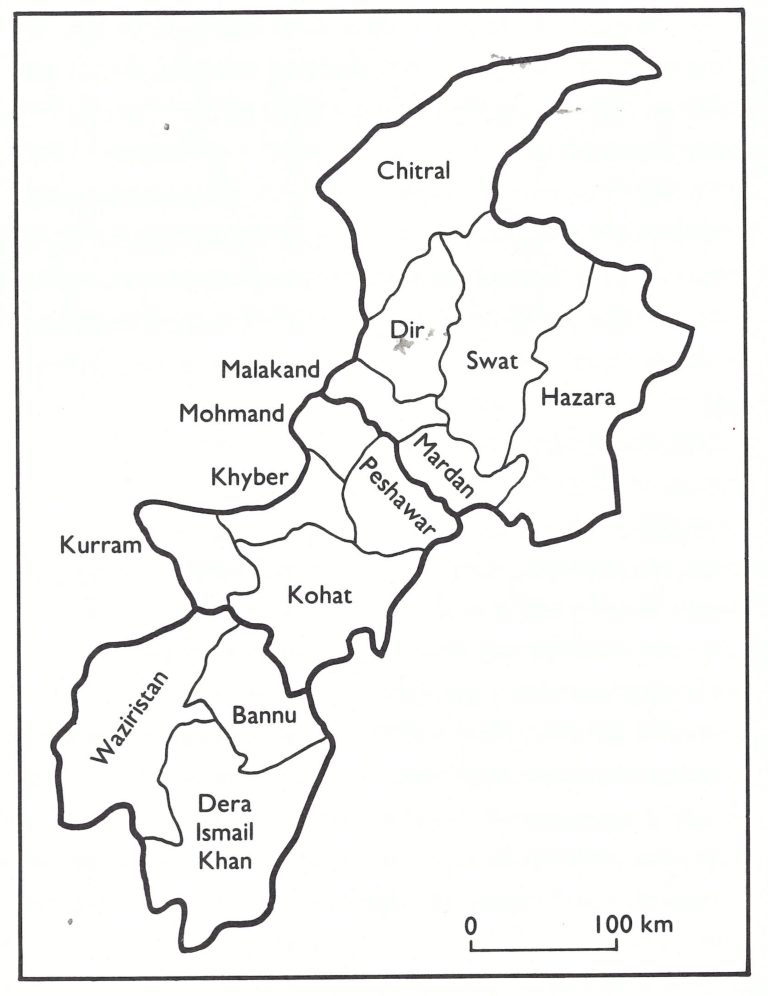
Fig. 14.15. Pakistan: districts of North-west Frontier Province, 1973.
Simultaneously with the beginning of a vaccination campaign in the Indus river plain, case detection and outbreak activities were extended throughout the province. Six “fire-fighting” teams, each with a vehicle, were trained and assigned responsibility for designated districts to improve case notification and to detect and contain outbreaks . Meanwhile, in Peshawar, the capital, 20 teams of 2 persons each began a house-to-house search for cases. When cases were discovered, an 8-man team carried out containment vaccination. For the first time in Pakistan, the strategy which had been recommended 5 years earlier by the Pakistan Medical Research Centre team was finally to be implemented.
The number of cases steadily decreased during the late spring and throughout the summer—the seasonal low point in smallpox transmission—and from October to the end of December, only 100 cases were discovered, of which 98 were in Peshawar District . The outbreaks all occurred near Peshawar City, in small villages frequented by smugglers from the tribal areas. None of the outbreaks was large but containing them proved difficult because the villages were considered to be dangerous, especially at night, and the villagers often refused to provide information about cases. Additional impetus was given to the programme, however, when in November a new WHO adviser arrived—Dr Reinhard Lindner, who had played an important role in developing the surveillance-containment strategy in Indonesia. Gradually, the problem in Peshawar came under control, and in April 1973 the last cases occurred in that district.
Meanwhile, cases began to be reported in January 1973 in the tribal areas of Kurram and Khyber, probably introduced from Peshawar. The teams were permitted to enter the area only with a military guard and only after assuring tribal leaders that they would not vaccinate them but would merely document the numbers of cases and deaths. In all, 101 cases were recorded in the outbreaks . Fortunately, smallpox transmission ceased spontaneously, probably in response to the traditional practice in villages of isolating cases and permitting only those previously infected with smallpox to care for the patients
During the first 6 months of 1973, the only cases detected in the entire province apart from those in Peshawar and the KurramKhyber tribal area were 2 imported into Mardan from Punjab Province in January, and 2 in Swat notified in May following an importation from Karachi. By May, it appeared that transmission had been interrupted. The vaccination campaign was stopped and the vaccinators were assigned solely to a search for cases. A reward of 25 rupees (US$2.50) was offered to anyone who detected a case. Numerous rumours were investigated but no cases were found. In October, the reward was doubled.
In November, however, importations began, primarily from Punjab but also from Sind and Baluchistan. Between November 1973 and September 1974, 35 outbreaks and 173 cases occurred. Of 34 outbreaks for which a specific source could be identified, all could be traced to Punjab, except 3 from Sind and 1 from Baluchistan. All but 3 of the cases were in the northern districts of Hazara (136 cases), Swat (26 cases), Dir (7 cases) and Mardan (1 case). The province’s final outbreak of 3 cases occurred in the southern district of Dera Ismail Khan, the last on 7 August 1974. Subsequent extensive search and a reward which was progressively raised to 200 rupees, then to 500 rupees and finally to 1000 rupees failed to uncover further cases.
Only partial data are available regarding the age distribution and vaccination status of cases in the province (Table 14.28).
As in Afghanistan, only a small proportion of cases occurred among adults, of whom, however, one-third had scars indicating previous vaccination. Fifty-eight percent of the cases occurred in children under 5 years of age, and although 10% were reported to have been vaccinated before onset, in some instances vaccination had been performed late in the incubation period during containment vaccination.
The achievements of the programme in North-west Frontier Province were notable. In April 1973, less than 2 years after the start of activities, transmission was interrupted, despite a health structure inferior to that of either Punjab or Sind Province, despite the greater difficulties of transport and communication and despite the existence of large population groups which refused vaccination. One might suppose that the authorities of other provinces would have found its programme and strategy instructive but, in fact, they openly doubted the reported results. In rancorous interprovincial meetings, they expressed scepticism and denounced the authorities of North-west Frontier Province for asserting that after April 1973 the only cases of smallpox that had occurred there had been imported from their provinces. Most adamant and vocal were representatives from Punjab Province.
Punjab Province
During 1972, Punjab Province strengthened its surveillance programme. Instead of 2 large surveillance groups, more surveillance teams of smaller size were created, each of which travelled extensively to improve reporting from the districts (Fig. 14.16) and to search for cases village by village. In all, 1495 cases were detected, 500 fewer than in 1971, when reporting was far less complete. Outbreaks were detected and contained reasonably quickly—73% being detected within a month of onset and 97% within 2 months.
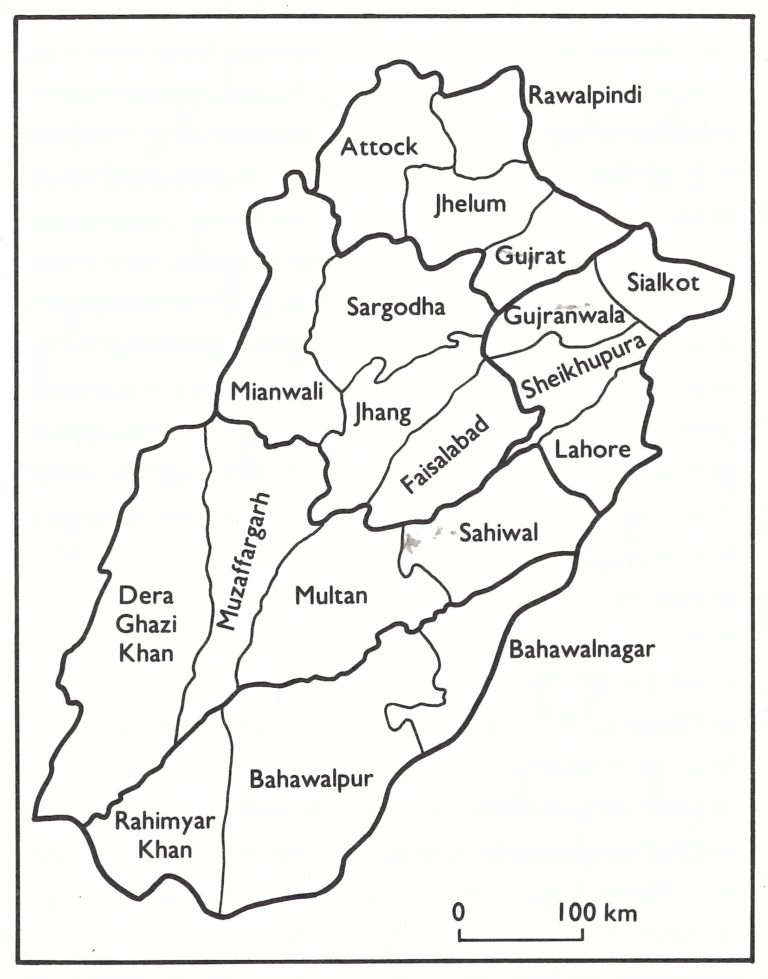
Fig. 14.16. Pakistan: districts of Punjab Province, 1973.
Little was done in urban areas, however, until May 1972, when special measures were taken to control smallpox in Lahore, the provincial capital . In the municipal corporation, 75 vaccinators were then working in 34 vaccination centres, only rarely leaving these centres to vaccinate people in the surrounding community or to detect and contain cases. It was agreed that a WHO adviser would be assigned to work in the corporation and, in May 1972, 6 sanitarians were trained in methods of case detection. One each was assigned to 4 sectors of the city and 2 were retained at headquarters to investigate cases brought to the infectious disease hospital. Each of the 34 vaccination centres was designated a primary reporting unit, which would send reports weekly, and 51 of the 75 vaccinators were assigned to a house-to-house search for cases; a special containment team of 10 vaccinators was stationed at the provincial office. A report prepared in October documented 314 cases in 52 outbreaks in Lahore District, primarily in slum areas around the perimeter of the city. ‘Almost one half (41.4%) of the cases were detected within 2 weeks of onset and 72% within 1 month. Only 4 outbreaks were traced to importations from other districts and these resulted in a mere 7 cases. However, numerous outbreaks, originating in Lahore, were identified during 1972 in other districts in the central and northern parts of the province. Indeed, between July and September, 37 % of all cases in Punjab could be traced to Lahore. Cases in the city continued to occur primarily among unprotected persons, who had been found, in a 1969 survey, to constitute only 6.9% of the total population (Ali & Heiner, 1971). Although immigration may have increased the proportion of susceptible persons somewhat during the 3 succeeding years, a continuing vaccination campaign served to sustain vaccinial immunity. Attack rates among contacts in infected households substantiated the fact that those who had previously been vaccinated were at significantly less risk than the unvaccinated (Table 14.29).
The importance to the province of controlling smallpox in Lahore had long been pointed out and this was fully substantiated when an effective programme was finally begun. Coincidentally with a decrease in incidence in Lahore, the number of reported cases of smallpox in Punjab, as well as in neighbouring North-west Frontier Province, fell sharply during the summer of 1972 and continued to decline during the autumn and winter months.
The programme was so successful that during March 1973, at the time of highest seasonal transmission, only 2 cases were detected in Lahore and only 8 in the entire province of Punjab. The Provincial Director of Health Services decided that the programme had succeeded and decentralized the surveillance operation. The Provincial Director of the Smallpox Programme was informed that he should undertake no further field travel and the WHO vehicle assigned to him was given to another medical officer. Each of the 5 divisional deputy directors of health services was assigned responsibility for one of the surveillance teams, and they in turn directed the teams to undertake other duties, primarily cholera vaccination. Surveillance in Lahore effectively ceased.
Through late October, the reported incidence of smallpox remained low; in fact, from 2 September to 20 October, no cases whatsoever were reported in Lahore District. It was the calm before the storm (Fig. 14.17). In late October smallpox outbreaks were again detected in Lahore, although investigations revealed that the city had, in fact, never been free of the disease. During December small pox spread widely through the city and cases began to appear in other districts and in North-west Frontier Province. By the end of December, 8 districts of Punjab had recorded outbreaks.
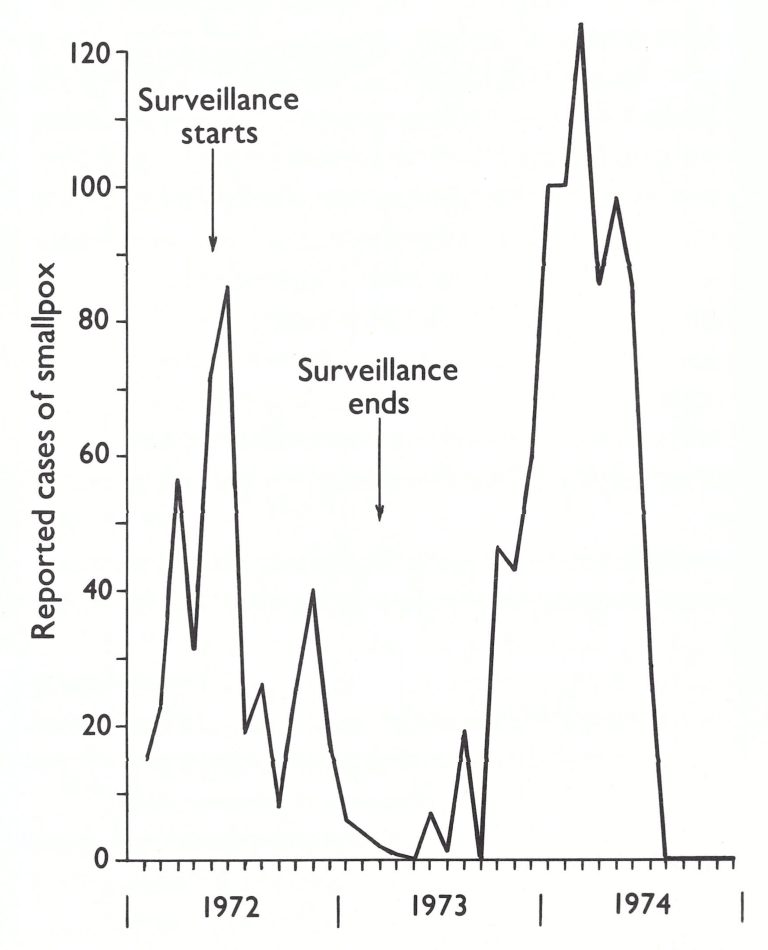
Fig. 14.17. Pakistan, Lahore District: number of reported cases of smallpox, by month, 1972-1974.
Despite the enormous resources and energies that had been devoted to the programme in Punjab, the situation had deteriorated to such an extent that conditions were not much better than they had been before the initiation of the mass vaccination campaign more than 5 years earlier. As at December 1973, the provincial smallpox eradication programme, such as it was, consisted of 4 wholly independent and uncoordinated components: (1) the Provincial Smallpox Eradication Officer with 8 assistant superintendents of vaccination and 14 surveillance agents; (2) 5 divisional surveillance teams under the direction of deputy directors of health services; (3) 19 independent district health offices, each with supervisors and vaccinators—some 1200 persons in all; (4) the municipal corporations, with their separate staffs.
It had been demonstrated beyond question in North-west Frontier Province that smallpox transmission could be interrupted even in difficult areas if the available resources were effectively managed. The problem in Punjab was to obtain an adequate political commitment, an appropriate strategy and a stability of leadership for long enough to permit this to be done.
Three events ultimately provided the necessary stimulus to a political commitment. The first was the recording in 1973 of 9258 cases of smallpox, the country’s highest total since 1948. Although this could be attributed to more complete notification, the political authorities were alarmed and began both to query the performance of health officials and to make greater resources available. The second event was the interruption of transmission in Afghanistan in 1972, which caused some embarrassment in Pakistan. Afghanistan, considered to be a far less developed country, pointedly and repeatedly indicated to the Pakistani authorities that all its cases since mid-1972 had resulted from importations from Pakistan . The third incident was India’s decision in the summer of 1973 to mobilize its vast resources of health manpower to undertake monthly village-byvillage searches to detect and contain outbreaks throughout the country. Optimistically, the Indian government forecast that the interruption of transmission would occur between January and June 1974. With Bangladesh and Nepal making excellent progress, it appeared that by late 1974 Pakistan might well be the last reservoir of smallpox in Asia.
Manpower in Punjab was not a problem but leadership and management were. A change occurred in February 1974 with the arrival of a new WHO—adviser Dr Omer Sulieman, the dynamic former director of the successful eradication programme in the Sudan. Within weeks, a moribund programme began to revive, and only 10 months later Punjab recorded its last case.
On his arrival in Lahore, Dr Sulieman reported on the situation: no plan or targets had been committed to paper; the concept of surveillance was accepted in principle but ignored in practice; officials continued to insist that vaccination targets should be met in all areas ; there was no search for cases; containment was poor; and cooperation between different groups was so lacking that even data regarding cases were not forwarded to the provincial office.
The Secretary of Health extended full support and ordered district and municipal corporations to cooperate with the programme. A written document establishing guidelines and technical commitments was prepared and distributed; surveillance teams were reconstituted and trained; a reward of 10 rupees for each new outbreak reported was announced; and vaccinators were asked to search for cases among the groups of people they vaccinated. To intensify the search, population planning and malaria eradication staff were directed to undertake a house—tohouse search for I week each month. When it was found that women were better received by the people and were more effective in searching for cases, 12 000 were employed between February and May; most of them were traditional birth attendants or municipal sweepers. In addition, during March, a special 2-day house-to-house search was conducted in Lahore by 50 000 schoolchildren and their teachers. They discovered 1800 persons with rash and fever of whom 13 were suffering from previously undetected smallpox.
Between February and May, substantial progress was made in the detection and containment of outbreaks but the smallpox incidence remained high. This was due, in part, to more complete reporting and, in part, to the high seasonal transmission. By June 1974, it was apparent that the cities of Lahore, Multan and Lyallpur (Faisalabad) were the key problems, accounting for the majority of cases and representing the source of infection of many rural outbreaks. In these cities, containment activities were strengthened, in line with the procedure then operating in India, by assigning a supervisor and 3 vaccinators to each outbreak to list and to vaccinate all residents and to stay in the area to vaccinate visitors until the outbreak was controlled. A vaccinator was also posted at each infected house until the last case had recovered. Efforts were also made to find and vaccinate all relatives, wherever they resided.
Whatever their instructions, some district health officers continued to rely on vaccination rather than surveillance and so, in June, routine vaccination was officially suspended and vaccinators were assigned solely to search and containment activities. To improve coordination, the Secretary of Health began to hold monthly meetings with all district health officers to emphasize his personal concern. In July, the health officers were relieved of other official duties in order to supervise a village-by-village search programme which covered one-third of the province’s 23 692 villages each month. This programme was similar to that which had begun in India almost a year before.
With a declining number of cases and outbreaks partly because of better control activities and partly because of the seasonal decline in smallpox incidence-it was possible to exercise better supervision in each remaining outbreak. Careful efforts were made to trace the source of cases and containment was tightened. Finally, on 16 October 1974, the last case of smallpox in Punjab, and in Pakistan as a whole, occurred in Multan City The search continued, enhanced by the offer of a growing reward, but no further cases were found.
In Punjab, less than 10 months had elapsed since the introduction of the first wellcoordinated province-wide programme of surveillance-containment and the occurrence of the last case. However, almost 6 years had passed since the beginning of the programme.
Baluchistan Province
Until 1972, little was achieved in the eradication programme in Baluchistan, the most sparsely populated and least developed of Pakistan’s 4 provinces. It occupies 40% of Pakistan’s land area and is composed of desert and rolling hills with few roads. Only 10% of the land was arable, most of it being in the eastern districts, in which the population was concentrated (Fig. 14.18). Baluchistan was a new province, created in July 1970, and the government structure was only beginning to take shape. Communication and travel were difficult; the postal service was all but nonexistent; and fewer than 100 physicians were employed there. Vaccinial immunity in Baluchistan was substantially lower than elsewhere in Pakistan, as was demonstrated by a scar survey performed in 1976 in 3 of the districts in which health services were the best (Table 14.30).
A mass vaccination campaign began in 1971 in the more populous north-eastern area of Quetta, Pishin and Zhob, employing some 30 vaccinators and some 20 support and supervisory staff. In fact, little was achieved, the numbers of recorded vaccinations for the province actually showing a decline, from 549 000 in 1970, to 422 000 in 1971.
Fig. 14.18. Pakistan: districts of Baluchistan Province, 1973.
In May 1971, a WHO adviser was assigned to the province, but the difficulties of maintaining even a few vehicles in operation in the field proved formidable. In the latter part of 1971 and in 1972, some outbreaks were investigated and vaccinations performed in and around Quetta, the capital, but little progress was made until the summer of 1972, when it was decided that a mass vaccination campaign was not feasible and the effort was abandoned. Surveillance agents were then posted to each district and 5 mobile teams, each composed of 4 persons, were constituted ; 2 of these undertook a search for cases and 3 performed vaccinations in what were considered to be vulnerable areas. The number of reported cases increased from 80 in 1970 to 291 in 1971 and to 559 in 1972 (Table 14.31). Cases were reported from each of the 10 districts in 1972, but most of them (444) were in Quetta and the nearby town of Sibi, in which the mobile teams were working. In all, the teams themselves detected 486 (87%) of the cases.
The surveillance programme futher improved following the arrival in February 1973 of an experienced WHO adviser, Dr P . R. Arbani, a national of Indonesia who had worked in the smallpox eradication programme in that country . By July, weekly reports of cases began to be received routinely from all districts. With improved training and increasing involvement of the few existing district and local health staff, cases were detected more quickly and were better contained. During 1973, 165 outbreaks with 801 cases were documented . With the exception of 2 cases in Chagai, all cases were reported from the more populous north-eastern districts.
By 1974, the surveillance programme was functioning far more effectively. Only 40 outbreaks with 202 cases were discovered during that year, of which 27 were detected within 2 weeks of onset; 30 of the 40 outbreaks consisted of only I or 2 cases (Tables 14.32 and 14.33). The last 4 outbreaks (of 2, 18, 23 and 65 cases respectively) occurred in Baluchistan in the summer of 1974 and were associated with variolation in Kalat District. Although the outbreaks were quickly detected, many cases among variolated children were already late in the incubation period before the team arrived.
After April 1973, all cases and outbreaks occurred near Quetta, in which the isolation ward of the civil hospital served as the principal focus for the dissemination of infection. In addition to being the source of Afghanistan’s final outbreak, mentioned earlier, the hospital was the focus of infection of 25 additional outbreaks over a 3-year period (including the last 4 outbreaks in Quetta), all of which were traced to patients who had contracted the infection there. Despite continuing efforts by provincial smallpox eradication staff to persuade the responsible hospital authorities to isolate patients and to vaccinate all persons admitted to the hospital, here, as at so many other hospitals, little was done until smallpox eradication staff were assigned to perform these duties.
Baluchistan recorded its last case on 30 August 1974. An extensive search was then organized throughout the vast, sparsely settled desert areas of its western provinces but no cases were found. Transmission had been pox in outbreaks, 1973-1974 successfully interrupted in less than 2 years after a surveillance programme had begun—and without benefit of a mass vaccination campaign. The costs were low The total expenditure by the government over a 3-year period from mid-1971 to mid-1974 was 610 000 rupees (US$61 500), or US$0.24 per head of population.
Fewer than one half of the cases in Baluchistan were among children under 5 years of age; one-fifth were among persons aged 15 years and over (Table 14.34). The generally older age distribution of cases reflects the occurrence of smallpox in comparatively isolated population groups among whom, in contrast to the situation in Afghanistan, variolation had not been widely practised in recent years.
The Last Outbreak in Baluchistan
Four weeks had elapsed without the reporting of a case in Baluchistan, when, on I August 1974, the assistant commissioner of a subdistrict reported to the district health officer in Kalat that he had heard rumours of smallpox in the area. A team immediately went to investigate and discovered cases in 4 villages (population 585) located at the top of a mountain, accessible only on foot. The first case had been exposed at Quetta's civil hospital in May and had become ill on returning home. On 4 June, a variolator was summoned; he took scabs from the patient and variolated the residents of the 4 villages. Between 4 June and 15 August, there were 108 cases and 9 deaths, as shown in the following table:
| Age group (years) | Natural infection | Variolation | ||
|---|---|---|---|---|
| Number of cases | Number of deaths | Number of cases | Number of deaths | |
| < 1 | 0 | 0 | 3 | 2 |
| 1-4 | 2 | 0 | 19 | 0 |
| 5-14 | 3 | 0 | 26 | 0 |
| ≥ 15 | 11 | 2 | 44 | 5 |
| Total | 16 | 2 | 92 | 7 |
None of those infected had ever been vaccinated . Although the inhabitants of the 4 infected villages had a low level of vaccinial immunity, 90% of the people in surrounding villages were found to have been vaccinated .
Sind Province
In Sind Province, which mainly comprises a flat alluvial plain, 40% of the population lived in urban areas, including the cosmopolitan city of Karachi (Fig. 14.19). It was comparable to Punjab in the extent of its health programmes and personnel and in the availability of transport and communication facilities. In all, Sind had 120 hospitals, 918 dispensaries, 103 rural health centres and subcentres, and 116 maternal and child health clinics. In 1972, vaccinial immunity was found by survey to be over 95% in Karachi, and although lower in the rural areas, generally speaking it was probably comparable to that in Punjab and much better than that in Baluchistan or in North-west Frontier Province.
Except in Karachi, the smallpox eradication programme was effectively ignored until the autumn of 1972. Early in 1971, the Karachi city authorities consolidated into a single organization the vast numbers of vaccinators who had been employed by a variety of different administrative jurisdictions, to undertake systematic vaccination and a programme of case detection. Three, later 6, surveillance teams and 3 containment teams complemented this effort, which proved so successful that between July and September 1971 no smallpox cases were found in the city. A week-long, city-wide search in mid-November confirmed the absence of cases. Karachi, however, was Pakistan’s largest city and principal seaport and numerous travellers from all over the country passed through it. Most of them were from other parts of Sind in which the smallpox incidence was probably higher than anywhere else in Pakistan. Importations led to a number of cases (369 in 1972, 335 in 1973 and 252 in 1974), and some outbreaks in other parts of Pakistan were traced to Karachi. However, smallpox in Karachi remained a minor problem in comparison with the situation in Lahore.
Provincial health authorities exhibited little interest in the programme until the autumn of 1972. The existing smallpox eradication staff of 724 persons, including 644 vaccinators (1 for every 23 000 persons) continued a routine vaccination campaign during which 3-4 million people were reported to be vaccinated annually. Reluctantly, the provincial authorities had agreed to the assignment of a WHO adviser, Dr M. Chamsa, who arrived in June 1971. Efforts had been made to mount a special vaccination campaign but lack of government support soon caused the attempt to be abandoned, and attention was focused on surveillance. With only limited resources available, this commenced in the autumn of 1972. Outbreaks were soon detected in every district 727 in all, with 3661 cases (Table 14.35)—4 times the number of cases reported during the previous year. Even so, weekly reports were not received from all districts, nor was an active search for cases begun until late in 1972.
By the autumn of 1972, national and WHO staff had become increasingly concerned about the inadequacy of the Sind programme and the lack of interest on the part of the health authorities. By that time, the smallpox incidence was declining rapidly both in Punjab and in North-west Frontier Province. The programme in Baluchistan was proceeding slowly, but since the population of the province amounted to only 1.9 million, it was of less concern. In Sind, which was much more densely populated, an effective programme was vital. Accordingly, in November 1972, WHO convened a special seminar in Karachi in which provincial officials from all over Pakistan participated, together with cases of smallpox, by district, 1970- smallpox eradication officers from other countries in the Eastern Mediterranean Region. The site had been deliberately selected in the hope of awakening the interest of senior officials in Sind . Henderson observed in his opening remarks:
“As for Sind, the considerable delay in initiating the programme and the many administrative problems encountered leave more yet to be done in the Province than in the other three . . . I can say honestly to you that in no other previously or presently endemic region are so many engaged in smallpox eradication ; in no other endemic region are health services, transport and communications so well developed nor the populations so willing to accept vaccination.” (SE/72.9, Henderson .)
Despite the fact that the surveillance system in Sind had improved little, the total of recorded cases in 1972 rose to unprecedented levels. This event, coupled with the conference, served at last to stimulate the health authorities to undertake a more effective programme.
Following the conference, activities were reorganized. Additional surveillance teams were constituted for search and containment Table 14.36. Sind Province: interval between first and soon the number of reported cases and last cases of smallpox in outincreased dramatically (Fig. 14.20), from 3661 breaks, 1972-1974 in 1972 to 7848 in 1973. Even so, detection was greatly delayed and when outbreaks were found, containment was poorly executed. The problem was apparent from the observation that 43 % of all outbreaks in 1972 and 24% in 1973 lasted more than 4 weeks (Table 14.36); 15% of all outbreaks in 1972 and 9 % in 1973 had 11 or more cases (Table 14.37).
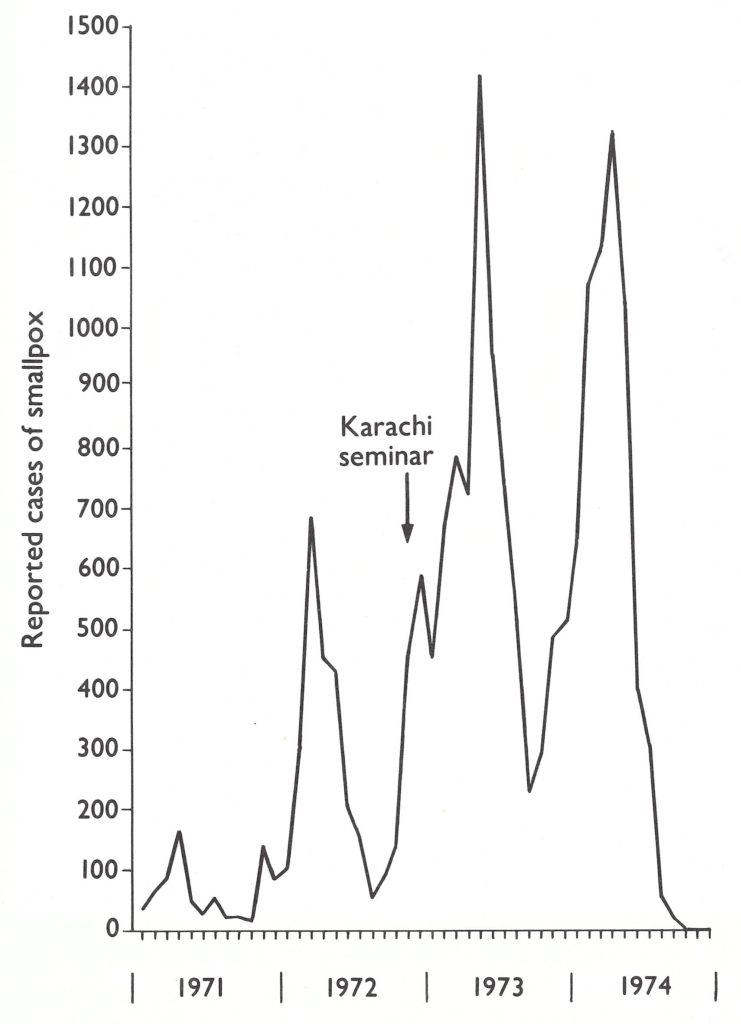
Fig. 14.19. Pakistan: districts of Sind Province, 1973.
Fig. 14.20. Pakistan, Sind Province: number if reported cases of smallpox, by month, 1971-1974.

Plate 14.8. Participants in the training seminar in Karachi, Pakistan, in November 1972. Left to right, front row: Khin Mu Aye (WHO), A . J . Hajian (WHO), A. K . Tabibzadeh (WHO), A . W . Katpar (Pakistan), D . A . Henderson (WHO), E. Shafa (WHO), F . Jurji (Iraq); Back row: N . Mohammad (Afghanistan), A . M . Darmanger (Afghanistan), unidentified, M . A . Dardmal (Afghanistan), M . Salehi (Afghanistan), G . D . Suleimanov (WHO), V. V . Fedorov (WHO), unidentified.
By the autumn of 1973, it was apparent that additional measures would be required . Whatever had been said about a change in strategy, district and local supervisory staff continued to be preoccupied with routine vaccination, undertaking case search and outbreak containment only with reluctance. Accordingly, in October 1973, activities were implemented that were similar to those which had been developed in India. To emphasize that the objective of the programme was to detect cases, vaccinators were redesignated “surveillance agents”. Teams of 2-3 persons were scheduled to visit once a month all villages (usually 100-150) in 2-3 union council areas to detect and contain outbreaks. Activities were supervised on the spot by a district superintendent of vaccination and a district smallpox eradication medical officer. Several provincial teams assisted in districts with the greatest problems. In Karachi, staff of the family planning and malaria control programmes participated in the search for cases. To encourage participation, a reward of 5 rupees (US$0.50) was offered to anyone finding a case. However, as a provincial surveillance officer observed, even this sytem of active search was poorly executed, the searchers devoting more time to obtaining the signatures of village leaders and teachers to prove they had been to the village than to searching for cases. The comparatively few special surveillance teams actually discovered more cases through questioning schoolteachers and persons encountered during their travel.
The results were dramatic nevertheless. Cases were discovered more promptly and were better contained. In 1974, 50% of all outbreaks consisted of only a single case and only 43 out of 1272 (3%) lasted more than 4 weeks.
During the summer of 1974, the number of cases fell steeply, from 1100 in May to 300 in June and only 55 in August. This corresponded to the customary seasonal decline in incidence observed throughout Pakistan, but with the momentum of search and containment achieved during the winter months, the few remaining outbreaks were more effectively contained. Finally, on 28 September, the last case occurred in Sanghar District, just prior to the beginning of the seasonal increase in transmission. However, programme staff remained sufficiently sceptical of the adequacy of surveillance that months were to elapse before they expressed confidence that transmission had in fact been interrupted.
Cases and deaths in Sind for the period 1972-1974 are shown in Table 14.38. Half of all the cases were in children under 5 years of age and only 8% were in individuals aged 15 and over, a marked contrast to the situation in Baluchistan. The overall recorded case-fatality of only 9% was unusually low for the subcontinent. Data from the city of Karachi (Table 14.39) suggest that this probably reflected incomplete notification of deaths in a province in which surveillance was notably poor.
As noted before, surveillance in Karachi had been consistently better than in the rest of Sind since 1971 and the cases which occurred during 1973-1974 had resulted primarily from importations from other parts of the province. Even when standardized for age, case-fatality rates were substantially greater than for the province as a whole, almost certainly reflecting more complete documentation of deaths rather than a difference in virus strains. A similar phenomenon had been observed in Indonesia, in which case-fatality rates were far higher in the city of Jakarta than in the surrounding West Java Province.
Northern areas of Pakistan-Gilgit and Azad Kashmir
In the federally administered, sparsely populated areas of Gilgit and Azad Kashmir, no special programmes were launched until 1974. Because the problems in the more populous areas of Pakistan were so formidable, neither national nor WHO staff considered it desirable to divert resources to these areas before then. It was hoped that in these northern areas, in which the population density was low, the transmission of smallpox might terminate spontaneously or be interrupted by control measures if cases were introduced. This proved to be the case. The population in Gilgit, estimated to be 450 000, lived in 5 different valleys in scattered hamlets and very small villages. A single rough road, open only 2 days a week, connected this area with the large urban centre of Rawalpindi, located in Punjab Province; as for connections by air, the single daily flight was often cancelled owing to bad weather. Between 13 000 and 100 000 vaccinations were recorded each year by hospital and dispensary staff. A reporting system was all but nonexistent. To assess the status of this area, an extensive search was conducted in the summer of 1976 but no evidence of recent cases of smallpox was discovered. Two unreported outbreaks were documented: 1 person in the eastern part of the region had developed smallpox and died in 1972, a week after returning from Karachi; and, in January 1971, 37 cases had occurred in the town of Gilgit, the largest urban centre in the region. Following the Gilgit outbreak, health staff, assisted by army personnel, had vaccinated nearly 150 000 persons. No surveys were done to document the levels of vaccinial immunity but it is doubtful that they were high.
Azad Kashmir, like Gilgit, is sparsely settled (population in 1975, 1 558 000), the people living in villages widely scattered over about 11 500 square kilometres of mostly hilly terrain. Many of the men travelled outside the area for work and, as a result, smallpox was introduced sporadically. In 1973, a special vaccination campaign was conducted by personnel of the 184 stationary health units, during which 1 381 294 persons were reported to have been vaccinated. Because of the lack of supervision or assessment of the programme, this figure was thought to be exaggerated. No information regarding cases was available before 1974,when an epidemiologist was assigned to the area. Between February and June, he documented the occurrence of 14 cases in 7 separate outbreaks, the last case occurring on 11 June 1974. No data were collected concerning the source of infection although it is assumed to have been the neighbouring province of Punjab. Extensive search in 1976 by special teams assisted by malaria control staff and local health personnel confirmed the absence of smallpox.
Variolation in Pakistan
Variolation continued to be practised in isolated areas in Pakistan throughout the duration of the programme but it was far less extensive than in Afghanistan or Ethiopia and did not significantly affect progress . As has been noted above, the last cases in Baluchistan occurred in an isolated desert area of Kalat District, but evidence of recent variolation was also observed in the southern desert of Punjab and in mountainous tribal areas bordering Afghanistan.
Variolation in Punjab was limited to the Rahimyar Khan desert near the borders with Sind and Baluchistan ; this practice persisted through 1973, and one unsuccessful attempt was detected as late as 1974 . A survey in 3 districts in this desert area revealed extensive variolation in the past but no evidence of it in the preceding 4 years except in Rahimyar Khan (Table 14.40).
In the tribal areas of North-west Frontier Province, variolation by traditional variolators, as in Afghanistan, had been common. An investigation was conducted in 1976 in one such area in Mohmand Agency during which the inhabitants of 31 villages were checked for the scars of variolation and the pockmarks of smallpox (Table 14.41).
More than three-quarters of the population over 10 years of age had variolation scars but surprisingly few had pockmarks . Evidence of variolation and/or pockmarks was seen only in children 3 years of age and older . This was supportive evidence that variolation had ceased, since it was usually performed when children were 1-2 years of age.
CONCLUSIONS
Following the occurrence of the last case of smallpox in Pakistan in October 1974, extensive searches were repeatedly conducted throughout the 4 provinces and 2 federally administered regions to confirm the absence of smallpox ; a reward of 100 rupees, later increased to 5000 rupees, was offered to anyone reporting an outbreak. Because of the programme’s earlier record of poor performance and the inadequacy of surveillance, uncertainty existed until the end of the year as to whether transmission had actually been interrupted. Only after several months of continuing search during the period of high seasonal transmission did national and international staff begin to feel reassured.
The situation in Afghanistan was entirely different. Since 1970, continuing efforts had been made to strengthen reporting and all outbreaks had been carefully investigated, their sources traced and the outbreaks contained. Surveillance was sufficiently extensive that when cases ceased to be detected, the Afghan staff were confident within a matter of weeks that natural transmission had ceased. However, since smallpox was still widely prevalent throughout Pakistan, there was a serious risk of its being reintroduced into Afghanistan and becoming re-established there. Indeed, transmission was interrupted more than 2 years earlier in Afghanistan than in Pakistan. Importations did occur but an effective surveillance programme quickly detected and contained the outbreaks.
In Afghanistan, there were few resources and only a rudimentary health infrastructure. Nevertheless, a highly effective programme rapidly took shape once a national commitment to the programme was made. In Pakistan, the resources were extensive, immunity was already high and a sound scientific basis for a programme had been elaborated . That Pakistan required so much longer to interrupt transmission reflects the difficulties of endeavouring to replace entrenched traditional doctrine-in this case, “100% vaccination”-with an alternative strategy that called for the detection and containment of outbreaks. Progress was unquestionably impeded by the attitude of some WHO advisers who, for so long, were not completely persuaded that this approach was correct. The delegation of authority and responsibility for health policy and programmes from national to provincial level further compounded the problem. Although national authorities attended the World Health Assembly, discussed global health policies and made commitments on behalf of Pakistan, provincial authorities bore the responsibility for deciding policy and priorities within their own jurisdictions. Some supported an eradication programme while others exhibited little interest. National authorities could do no more than exhort and cajole. In consequence, a successful effort in North-west Frontier Province was jeopardized by the sudden collapse of the programme in Punjab, and both programmes were compromised by repeated importations of smallpox from Sind and Baluchistan, neither of which exhibited interest in smallpox eradication until late in the programme.
The question arises, in respect of Afghanistan, whether surveillance-containment measures alone might have succeeded, in view of the fact that transmission was interrupted so rapidly once these measures had been taken. Given the extent of variolation, it seems doubtful, in retrospect, that the staff could have dispensed with mass vaccination and the accompanying programme designed to educate village leaders and the villagers themselves about the dangers of variolation and the advantages of vaccination.
In 1968, the attainment of eradication in Afghanistan had been considered to represent the Intensified Programme’s most difficult challenge. With the interruption of transmission there, senior WHO staff speculated anew as to which country or area might constitute the insuperable obstacle to global eradication. A few thought that it might be Ethiopia. Most, however, conjectured that it would be the populous country of India, which was generally believed to be the original home of smallpox and in which, perhaps, unique factors of climate, crowding, etc., permitted transmission to persist as in the case of cholera. In the next chapter we shall turn to the programme in India.